Advocates of mental health parity propose legislation that would require all private health insurance to establish the same deductibles and co-payments for physical and mental health care services. They see these proposals as ways to end discrimination against the mentally ill. However, parity legislation is more likely to make the current system worse, by imposing an arbitrary rule that would make it even more difficult for doctors, patients and insurers to find better ways of delivering health care. Rather than acknowledge the considerable differences that exist between mental and physical health care and modifying government policies to account for them, parity would make our current problems worse in eight ways:
Higher Costs.
The United States already spends a greater percent of our national income on health care than any other country – an amount equal to $4,700 for every person in America, or $18,800 for a family of four! Most of this total is paid in taxes to support someone else's health care. A parity mandate would make those costs even higher. According to PricewaterhouseCoopers, the mandate would increase insurance premiums by 10 percent.
Note that higher costs do not necessarily mean more or better services. Among developed countries, the history of health economics teaches one clear lesson: If you increase demand without increasing supply, you end up paying higher prices for the same services with which you began. Other countries experienced severe health care inflation when they adopted national health insurance. The United States experienced it after creating Medicare and Medicaid.
An increase in the demand for mental health services will not produce an increase in supply unless there are unemployed or underutilized doctors, nurses, facilities and so forth. There is no problem in increasing the supply of pharmaceuticals. But where are all the underutilized doctors and nurses?
Of course it would be possible, through economic incentives, to induce personnel to switch to mental health from some other health care field. But the result would be more money spent with no more health care made available. The extra services received by some mental health patients would be offset by fewer services available to other patients.
Note that although the supply of doctors is relatively inelastic, untrained potential providers – from pop psychologists to amateur therapists – abound. Without controls, the use of these nonmedical personnel could explode. And although an enormous amount of money is spent on "talk therapy" every year, its value remains unclear. (See The Case Against Mental Health Parity: Part III.)
More Uninsured.
Health insurance mandates imposed by state governments have already priced as many as one out of every four uninsured out of the market for insurance. A parity law would make things worse.
According to a Blue Cross Blue Shield estimate, for every 1 percent increase in the cost of health insurance premiums due to mandated benefits, 3 percent of small employers are forced to drop health coverage for their employees. Thus if parity legislation increases the cost of premiums by about 10 percent, 30 percent of small employers would no longer offer coverage to their employees. A Congressional Budget Office study estimates that for every 1 percent increase in premiums, 200,000 Americans lose their insurance. This implies that a nationwide parity law would cause 2 million additional people to be uninsured.
Higher Taxes.
More uninsured means that more people would be unable to pay their medical bills and would rely on free care from the public sector instead. That means a bigger burden for taxpayers.
More Managed Care.
One way to avoid the abuses of managed care is to have managed care plans compete against other plans on a level playing field. But a parity law would tilt the field in favor of managed care. This is because almost all parity laws have a managed care loophole: They tie the hands of fee-for-service plans while leaving managed care plans free to restrict services virtually at will. Studies show that managed care can reduce the cost of mental health care. But if the deck is stacked in favor of managed care, patients can be worse off.
In general, any limits on care in an insurance contract can also be achieved through a carefully drafted agreement with providers. Parity advocates seek to eliminate clauses in insurance contracts that, say, limit the number of physician visits or days in a hospital. But insurers can achieve these same results through contracts that give providers economic incentives to withhold care. Thus a parity law does not necessarily mean that the mentally ill would get more care. They might get less. In fact, the General Accounting Office (GAO) concluded that health insurance benefits for the mentally ill were reduced after Congress passed the last mental health parity mandate. (That mandate requires any cap on mental health benefits to be the same as any cap on physical health benefits.)
Less Innovation.
A parity requirement would essentially outlaw attempts to experiment and innovate with different payment schemes. For example:
- One South African insurer got lower costs and better outcomes by enrolling diabetics in centers of excellence with the insurer paying two-thirds of the cost and the patient the other one-third from a Medical Savings Account. The next step is to try the same approach with asthma. Could this model also work for substance abuse patients? If the parity advocates have their way, Americans may never find out.
- The federal government and the Robert Wood Johnson Foundation have collaborated on pilot programs in several states that give physically disabled Medicaid patients control of some of their own health care dollars – allowing them to directly purchase such services as help with bathing, eating and dressing. Could such an approach also work for the mentally disabled? Again, if the parity advocates have their way, we may never know.
Worse Health Outcomes.
Independent of managed care, a parity law is likely to lead to worse health outcomes than with the opposite approach: encouraging a variety of payment mechanisms, depending on the nature of the illness. A parity law would certainly be worse than what could be achieved with flexible Medical Savings Accounts. Evidence from South Africa suggests that patients spending from their own MSAs are able to control drug costs as well or better than managed care, without the expense of managed care. (See the Figure.)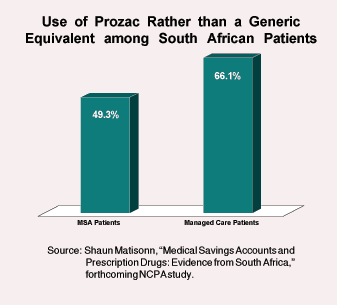
A Slippery Slope for Other Illnesses.
Although parity advocates are focused on mental health, the logic of their argument is that we should have the same payment rules for every illness. The result would be no centers of excellence for diabetes or asthma patients with special patient cost sharing. This is bad economics – and bad health care.
A Slippery Slope for Other Special Interests.
The history of mandates at the state level follows a pattern: Once a state passes a mandate in an area, a slew of special interests spring forth to ask for more mandates. For example, after state governments required insurers to cover mental health, we got more laws:
- Forty-two states have laws stipulating that if insurers provide coverage for psychiatrists, they must also provide coverage for psychologists.
- California and nine other states mandate coverage for marriage counseling.
- Vermont, North Carolina and Maine mandate coverage for pastoral counseling.
Elevating this special interest feeding frenzy to the national level can only result in higher costs and more people uninsured.
John C. Goodman is president and Wess Mitchell is a research assistant with the National Center for Policy Analysis.