A cornerstone of President Bush's approach to health care reform is the creation of Association Health Plans (AHPs). Intended to control costs and improve access to coverage for small employers and individuals, AHPs would allow bona fide business and professional associations to offer health benefits to their members.
For example, the National Restaurant Association would be able to offer insurance to employees of mom and pop diners across the country. A regional association of auto dealers would be able to do the same for its members' employees. By grouping together individuals or many small businesses, these associations could take advantage of the economies of scale in group buying. AHPs would also be permitted to self-insure – something that only large companies are able to do today – and avoid many costly regulations state governments have imposed on the market for health insurance.
Advantages
AHPs offer a number of advantages, including:
- Marketing Efficiencies. Relieving every auto dealer or print shop from having to seek out its own coverage, AHPs would enable associations to comparison shop on behalf of hundreds or thousands of member companies.
- Increased Choice for Employees. Representing perhaps thousands of companies with tens of thousands of workers, associations could offer an array of benefit plans and allow employees to choose the plan that best met their needs.
- Reduced Administrative Costs. By self-funding their benefit programs, an association could gain many of the administrative savings large employers enjoy. In the small group and individual insurance market, one-fourth to one-third of every premium dollar is spent on administrative costs, including premium taxes, commissions, compliance costs, etc. Large, self-funded employers are exempt from many of these costs and can reduce them to as little as 10 or even 5 percent.
- Consistent Regulations. Rather than having to comply with the disparate regulations of 50 states, the association would have to comply only with federal regulations identical for all of their member companies. The difficulty of keeping up with changing state requirements has forced many established associations to stop offering coverage in recent years.
- Fewer Mandated Benefits. Mandated benefits for such services as social worker visits and in vitro fertilization represent a particularly burdensome form of state regulation. The states have passed more than 1,500 mandated benefit laws. While employers are not required to provide employee health insurance, if they provide any coverage they must also cover their state's politically inspired mandates.
Employers who are large enough to pay directly for the health care services consumed by their employees, rather than buying insurance from an insurance company, already enjoy these advantages. But many employers are too small to self-fund their benefits and must purchase coverage from a state-regulated insurance company instead.
Costs for Small Businesses
According to a recent survey sponsored by the Kaiser Family Foundation (KFF) and conducted by the Health Research Educational Trust (HRET), only 55 percent of companies with 3 to 9 employees offer coverage, compared to 74 percent of those with 10 to 24 workers, 88 percent of firms 25 to 49 workers, and 99 percent of firms exceeding 200 workers. The Employee Benefits Research Institute (EBRI) reports that the number of uninsured is directly correlated with the size of the firm they work for. [See Figure I.]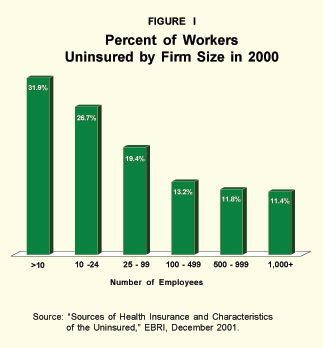 "High premiums" are the reason cited by 68 percent of all companies with fewer than 200 employees that do not offer coverage.
"High premiums" are the reason cited by 68 percent of all companies with fewer than 200 employees that do not offer coverage.
The Opportunity to Self-Insure
The KFF/HRET survey found that fully insured plan premiums have risen faster than self-funded plan premium equivalents in each of the last five years. [See Figure II.] Premiums increased by 61.3 percent for fully insured plans, compared to 42.5 percent for self-funded plans.
The increases in insurance premiums are even more startling when compared to the overall medical inflation rate of about 4 percent per year over the same period. The usual explanations for health care cost increases – aging population, new technology, price increases – are not sufficient to explain the difference. If anything, these factors should have a greater effect on health costs for the general population than on the cost of employer-based plans, since the latter seldom cover the elderly, and should be insulated from price increases due to negotiated contracts. The cost differences between insured and self-funded plans are even harder to fit into the traditional explanations. New technology, an aging workforce, and increasing prices for health care services should not affect smaller insured employers more than larger self-funded employers.
PricewaterhouseCoopers (PWC) attempted to explain some of the differences in a recent report prepared for the American Association of Health Plans. PWC included some factors that would apply across the board and contribute to medical inflation generally, such as medical advances, general inflation and increased demand due to an aging population. But it also identified some trends unique to employer-based coverage, especially to fully insured employers. These include the more than 1,500 state mandated benefits, additional federal mandates, duplicative and confusing regulations, a growth in litigation, and fraud and abuse. These factors account for more than one-fourth of the recent run-up in premiums, according to PWC.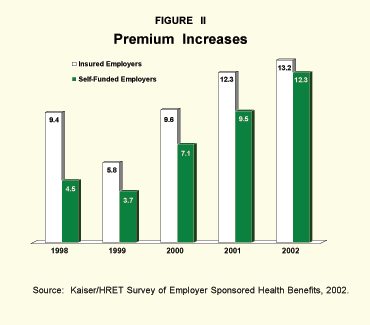
Not cited by PWC, but also likely to affect premiums for small businesses and individuals, is the so-called underwriting cycle, in which insurers compensate for underpricing benefits in some years by increasing premiums faster in other years. Since self-funded employers don't pay premiums, but simply pay the health care expenses incurred by their employees, they should be exempt from the underwriting cycle. The KFF/HRET survey reveals that premium increases from 1995 to 1998 were actually lower than general medical inflation. The underwriting cycle would explain why premiums for insured employers rose so much faster than self-funded plans from 1998 though 2001, then leveled off to approximate the rate of increase experienced by self-funded employers in 2002.
Conclusion
Federally regulated, self-funded Association Health Plans would help expand the small group market and allow small employers to enjoy many of the advantages that larger employers currently have. They would lower direct costs by reducing regulatory compliance costs, lowering administrative expenses and increasing marketing efficiencies.
They also would help stabilize the market by avoiding the underwriting cycle of premium spikes and dips that plague the fully insured market today. And they would enable even the smallest employer to give employees a choice of health plans.
Part Two answers the critics of Association Health Plans.
Greg Scandlen is a senior fellow in health policy with the National Center for Policy Analysis.