Support is growing for a proposed solution to the rising number of uninsured Americans: a health insurance tax credit. If properly designed and implemented, a tax credit would allow uninsured, low income individuals and families to purchase affordable, quality health insurance.
To be effective, a health care tax credit must meet some specific criteria: (1) It must be refundable for lowwage workers (that is, they get the subsidy even if they have no tax liability); (2) The credit must be advanceable, so that it can be used to pay monthly premiums as they come due, rather than a lump-sum payment received when tax returns are filed on April 15; (3) It must not come with costly mandates that raise the cost of insurance and price healthy people out of the market; (4) It must be widely available, so that the market is large enough to attract many buyers and sellers; (5) It must be limited in dollar amount so that it does not encourage wasteful spending; and (6) It should be compatible with Health Savings Accounts (HSAs).
The Tax Credit Under Current Law: One Step Forward. In 2002, Congress created a health care tax credit for individuals who have lost their manufacturing jobs to foreign competition. Also eligible are individuals whose pensions are endangered because their former employer went belly up. The goal was to help this vulnerable population afford health insurance by giving them a credit worth 65 percent of the cost of their premiums. Yet, only six percent of those who may be eligible have taken advantage of the credit. Why?
Unfortunately, in designing the credit, under the Trade Adjustment Assistance (TAA) program, Congress took one step forward and three steps back. The forward step is that the credit is advanceable and refundable, allowing individuals with modest incomes who owe little or no income tax to receive the federal subsidy as their premiums come due.
Guaranteed Issue Regulations: One Step Back. But Congress took a step back by mandating that any insurance company offering policies to the eligible population must provide coverage to all individuals who qualify for the credit, regardless of their medical condition. This restriction, known as guaranteed issue, may sound like a way to protect consumers, but it actually harms those who need coverage by driving up prices. When insurance companies are forced to accept all applicants, they raise premiums to guard against loss. Subsequently, business dwindles because neither sick nor healthy people can afford the policies, so carriers leave the market, and rates go up as competition decreases.
These outcomes have been borne out repeatedly in all eight states that have imposed guaranteed issue on insurance carriers in the market for individually purchased insurance. For example, when New Jersey imposed guaranteed issue on all health insurers, state premiums skyrocketed to more than double the national average. As recently as September 2004, New Jersey's average individual insurance premium was $4,080, compared with the median average of $1,656. The state of Kentucky has now done an about-face, repealing guaranteed issue after 45 insurers left the state and consumers had no access to affordable coverage.
Likewise, when Congress mandated guaranteed issue on carriers participating in the TAA credit program, they received very few takers. According to the U.S. Treasury Department, of the 39 states participating in the program, 20 have no private carriers offering a policy and 14 states have only one private insurer offering a plan. The resulting lack of competition drives up prices, limits choice, and, ultimately, limits consumer participation and coverage.
Limiting the Market: A Second Step Back. Congress took another step back when it chose to limit the TAA tax credit mostly to individuals near retirement age and living on meager unemployment benefits – a population with more limited means and significantly higher health needs than most other uninsured. A recent Government Accountability Office report found that to use the tax credit, those eligible had to spend 13 percent to 25 percent of their monthly income on premiums. Testing a tax credit on this population, combined with inflated prices due to guaranteed issue, was a recipe for failure.
Encouraging Wasteful Insurance: A Third Step Back. Another flaw in TAA health credit design is that it provides an unlimited, partial subsidy, rather than a dollar-for-dollar credit up to a maximum limit. Individuals must pay 35 percent of the cost of their health insurance, with taxpayers picking up 65 percent. This encourages waste by subsidizing the last dollar of insurance spending as much as the first dollar. By contrast, a 100 percent tax credit for the lowest income purchasers could reduce the cost of a modest – but still comprehensive – policy to zero. Limiting the credit to a fixed amount requires individuals to pick up 100 percent of the additional cost for policies with more expensive coverage.
The Bush administration's proposed tax credit avoids this problem by offering a flat dollar-for-dollar credit to low income individuals ($1,000) and families (up to $3,000). The credit phases out gradually for those with higher incomes (more than 200 percent of the poverty level), but the fact that it is limited avoids the incentive to spend wastefully.
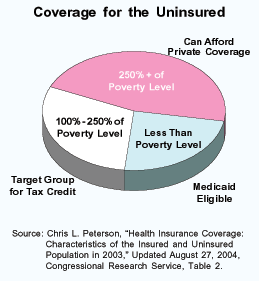
Prospects for a Workable Tax Credit. The good news is that tax credits can work if they are well designed and target the right buyers. The majority of today's uninsured are working individuals and families with very modest incomes. They earn too much to qualify for Medicaid, but not enough to afford coverage without assistance. They may be in jobs where health insurance is not offered or cannot afford their share of their company's coverage. In fact, more than 80 percent of uninsured individuals have full or part-time jobs and more than 30 percent have incomes that are 100 to 200 percent of the federal poverty level. This should be the target group for a health tax credit. [See the figure.]
This uninsured population is relatively young and eminently insurable at reasonable rates. In most states, the limited credit proposed by President Bush would pay for between half and two-thirds of the average cost of health insurance (based on a full $1,000 tax credit and eHealthInsurance's estimated median average individual premium of $1,656 annually).
For uninsured individuals with chronic health conditions, coverage should come through state high-risk pools, programs that already exist in 33 states. These pools allow the small percentage of the uninsured with serious health conditions to obtain health insurance coverage that is capped at 150 to 200 percent of the average premium cost in that state. This cost could be offset with tax credits, thus providing a safety net for a vulnerable population, while keeping premiums more affordable to others.
Tax Credits for Health Savings Accounts. Congress should also consider using tax credits to help people afford the newly created Health Savings Accounts. HSAs are attractive to those with modest incomes because premiums are much lower with high deductible policies coupled with HSAs. A portion of the tax credit ($700 for individuals, $2,000 for families) could be used to purchase insurance and the remainder ($300 for individuals, $1,000 for families) could be deposited directly into a tax-free HSA to use for deductible expenses under a Bush administration tax proposal. HSAs, which are portable from job to job and into retirement, provide an excellent way for individuals and families to accumulate savings for health expenses.
Laura Trueman is executive director of the Coalition for Affordable Health Coverage (CAHC.net).