"For more than 50 years, employers have been the main providers of health insurance coverage."
Many employers are concluding that it is time to rethink the way they provide health insurance benefits for their employees.
For more than 50 years, employers have been the main providers of health insurance coverage for Americans. There have been dramatic changes during those years. Fifty years ago, only half of all Americans had any health insurance coverage, and most of that was hospital indemnity coverage that provided a fixed dollar payment for a certain number of days in a hospital.1
"In 1960, more than half of the health care dollars were spent out of pocket."
Through the 1950s and 1960s, employer-based coverage grew in both numbers of people covered and richness of benefits. By 1965, 72.5% of the population was covered by some form of private health insurance, with half (50.3%) of these covered by "major medical" plans – double the percentage just five years earlier (26% in 1960).2
Despite the growth in employer-sponsored coverage, most health care spending continued to be paid out of pocket. As Figure I shows, in 1960, out of total health care spending of $23.6 billion, $13.1 billion (55.5%) was paid out of pocket, $5.4 billion (22.9%) by private third-party payers, $3 billion (12.7%) by state and local government, and only $2.1 billion (8.9%) by the federal government.3
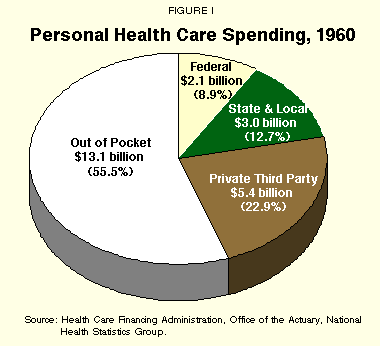
"The percentage of out-of-pocket health care spending has shrunk dramatically since the creation of Medicare and Medicaid."
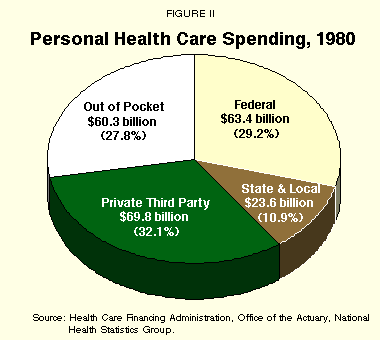
This changed dramatically after the creation of Medicare and Medicaid. By 1980, as shown in Figure II, total health care spending reached $217.0 billion, with only 27.8% out-of-pocket. Private third party payers picked up 32.1% and the federal government paid 29.2%.4
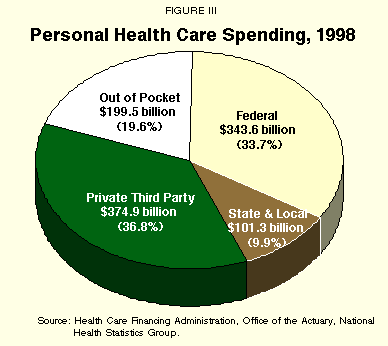
These trends have continued. In 1998, with total health care spending of $1,019.3 billion, the federal government was paying for more than a third (33.7%), as Figure III shows. Out-of-pocket spending diminished to 19.6% of the total, and third party payments grew to 36.8%.5
Not surprisingly, the flood of new federal money and the decrease in out-of-pocket spending resulted in health care inflation and an increasing share of national income going to health care after 1965. As a percentage of Gross National Product, health care spending increased from 4.6% in 1950 and 1955 to 5.2% in 1960, 5.9% in 1965, 7.2% in 1970 and 8.3% in 1975.6
In response to this alarming growth, the federal government imposed a series of new laws and regulations intended to slow health care inflation:
"The flood of new federal money and the decrease in out-of-pocket spending resulted in health care inflation and an increasing share of national income going to health care."
-
President Nixon imposed wage and price controls in August 1971. The controls were lifted for most of the economy in January 1973 but retained for health care until April 30, 1974.7
-
Legislation creating Professional Standards Review Organizations for Medicare was enacted in 1972. This law was intended to supervise physician practice to ensure appropriate treatments and lengths of stay and to restrain costs.8
-
The Federal HMO Act of 1973 provided seed money for HMOs that met certain federal standards, and exempted these HMOs from state regulation. It also included a "dual choice" provision that required employers with more than 25 employees to offer an HMO option.9
-
The National Health Planning and Resources Development Act of 1974 created an elaborate health planning system aimed at controlling the growth of hospitals and other health care facilities.10
-
Also, the Employment Retiree Income Security Act (ERISA) was enacted in 1974. ERISA enabled employers to escape state regulation by self-insuring their health benefits.
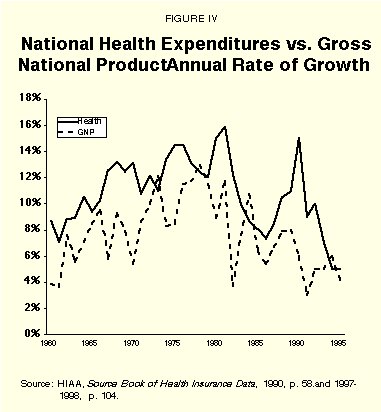
Despite all these efforts, health care costs continued to rise. Every year from 1965 through 1982, the nation endured increases in health care spending in excess of 10%, reaching 14.5% in 1975 and 1976, 14.9% in 1980 and 15.9% in 1981 [see Figure IV].
In the early 1980s, many large employers switched to self-insurance under ERISA to better control their health care spending. At that time of high inflation and high interest rates, many employers did not believe insurance companies were doing enough to restrain spending. One executive told Congress, "When we were insured, the insurer got a percentage of the claims paid. They had no interest in holding down costs."11
Employers instituted a number of cost-containing efforts, including benefit redesign emphasizing outpatient care over inpatient treatment and programs such as second surgical opinions and preadmission certification. They also increased benefits for substance abuse treatment, hospice and home health services. These programs had remarkable, if temporary, success. One author wrote, "Inpatient days dropped from 278 million in 1981 to 220 million by the end of the decade… outpatient visits increased from 203 million in 1981 to 300 million by 1990."12 Former Secretary of HEW (Health, Education and Welfare, now Health and Human Services) Joseph Califano had gone to work at the Chrysler Corporation and concluded the private sector could do cost containment far better than the government. He wrote:
My conviction that the key to health care cost containment rests in an aroused private sector in no small measure relates to the contrast between the frustration of trying to get government to deal with this problem and my recent experience with Chrysler Corporation. In 1984, Chrysler cut its health care bill to $402 million, down by $58 million from the $460 million projected in our budget."13
"Managed care has had success in holding down cost increases, but at a high price in employee morale and community relations."
Mr. Califano had a lot to crow about when he was writing in 1986. For five years in a row (1982-86) the rate of increase in total national health care spending had dropped. He wasn't alone. Margaret Heckler, Secretary of HHS under President Reagan, famously said in 1985 that we had "broken the back of the health care inflation monster."14
But soon enough, health care inflation was back, growing every year for four years until it reached 15% in 1990. Employers had succeeded in holding down costs for a time, but now they needed another strategy. They switched to managed care in massive numbers. From 1984 to 1990, HMOs and PPOs increased their share of the private benefits market from 7% to 34%, and they continued to grow through the 1990s, capturing 65% of the market in 1995.15 More recent estimates place managed care's market share at 85%.16
The hope for managed care was that it would provide first-rate health care while restraining utilization and cost. Managed care was supposed to provide incentives to keep people healthy so they would consume fewer health care services. It was supposed to help patients bond with their primary care provider who would direct them to the most cost-effective services. It was supposed to educate patients to take better care of themselves and avoid expensive professional care for ordinary ailments. It was supposed to bring a new businesslike attitude to health care services.
In fact, managed care organizations (MCOs) have had success in holding down cost increases, but at a high price in employee morale and community relations. Cost increases may have flattened, but the reasons aren't clear. It may be that MCOs have reduced waste and increased efficiency. Or it may be because that MCOs have denied needed services; or have selected healthier customers; or have underpriced their premium to gain market share; or have provided lower-quality care and service; or have cajoled doctors into providing cheaper – not better – care. Academic research on these issues has been mixed.17
Most likely, the causes for the reduction in cost increases are a complex mix of many factors, but there is little evidence that managed care has lowered costs by improving patient health or by preventing disease. There is little evidence that MCO patients are better educated or better able to avoid needless care. There is little evidence that MCOs are more efficient at delivering care.18
But there is plenty of evidence that patients and doctors are disgruntled. They resent externally imposed controls, and fear that needed services are being denied.19 More importantly, employees object to being placed in a plan without their consent. Research indicates that people who choose managed care are usually happy with their choice. It is the people who have no choice who are the least happy.20 Eighty-three percent of employers offer no choice of health plan at all and the remainder usually provide a choice of only two or three plans.21
[page]"Employers are sick of being caught in the middle of an essentially political argument between doctors and health plans."
Employers currently see premiums rising again. They are nervous about the prospect of being held liable for bad outcomes. They worry that even a choice of several plans is no longer suitable for a diverse workforce. They are tired of the unpredictability of health care expenses and of the administrative costs associated with managing a benefits plan. And they are sick of being caught in the middle of an essentially political argument between doctors and health plans. They get few kudos for spending $4,000 to $6,000 per employee on health care, but they get a ton of grief if Viagra or in vitro fertilization isn't covered.
They are also concerned about increasing regulation, as the federal government follows the states in placing social policy on the backs of employers through mandated benefits and other regulations.22 This year's sensation is the "Patients' Bill of Rights." Before that came COBRA, HIPAA, mental health parity, mandates passed by Congress on hospital stays for childbirth and mastectomies and a slew of other proposed mandates. Every year there seems to be something new for corporate human resource administrators to comply with.
Employers want to stop being "the monkey in the middle." They want to get out of managing health benefits. At the same time, they want their workforce covered and productive. They know that having a good health plan reduces expenses for sick leave and can boost worker morale. The question is how to balance these two competing interests.
Increasingly, employers are looking at their pension benefits as a model. They have successfully moved their retirement programs from defined benefits to Defined Contribution programs like 401(k)s.23 Employees are happy to control their investments and shape their own futures. Employers are happy to have a fixed, budgetable obligation administered by professional money managers. They wonder whether they can apply the same approach to their health care obligations.
[page]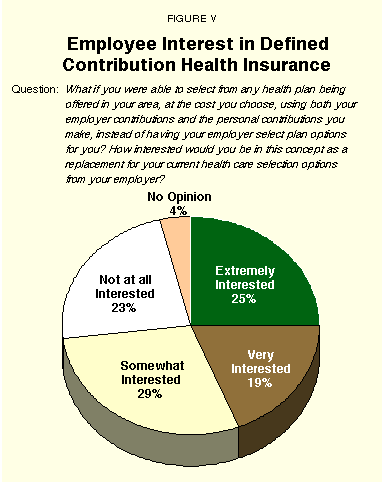
To date, there has been little implementation of a Defined Contribution approach to health care. Employers are still working through the implications of such a move for their workforce and for their companies. But recent surveys show a significant level of interest among both employers and employees.
"Recent surveys show a significant level of interest by both employers and employees in a Defined Contribution approach."
Cigna/Benefits Access. One of the first surveys was conducted by Benefits Access, Inc. (owned by Cigna), published in October 1998.24 The firm surveyed human resource executives at 900 mid-sized companies and found that "60% of HR executives wish they could provide employees with enough information to make their individual benefits decisions and 'leave the rest to them.'" It also found a great deal of frustration among HR executives who felt underfunded and overworked.
PricewaterhouseCoopers. About a year later, PWC released its "Healthcast 2010"25 report, which included a survey of "U.S. Healthcare Leaders." The report stated flatly that "Defined Contribution programs will emerge in healthcare." It explained:
Moving to a Defined Contribution program may allow employers to better control their cost obligations of providing healthcare benefits. "Health benefits are becoming more of a dissatisfaction of employees," says one employer who spoke of the hassles of negotiating coverage denials with insurers on behalf of workers.
PWC reported that some 62% of "healthcare leaders" expect that employers will move to Defined Contribution by 2010, 58% expect Medicare to do the same and 60% think that most employers will offer Medical Savings Accounts by then.
KPMG. KPMG surveyed 103 senior executives and over 14,000 employees of Fortune 1000 companies to test their interest in the Defined Contribution concept.26 The results were first presented at the "Consumer-Driven Health Care Conference" organized by Prof. Regina Herzlinger at the Harvard Business School in November, 1999. KPMG asked employees:
What if you were able to select from any health plan being offered in your area, at the cost you choose, using both your employer contributions and the personal contributions you make, instead of having your employer select plan options for you? How interested would you be in this concept as a replacement for your current health care selection options from your employer?
"The vast majority of those interested in a Defined Contribution approach were satisfied with their current choice of health plan."
As Figure V shows, 25% were "extremely interested," 19% "very interested" and 29% "somewhat interested." It is worth noting that of the 73% of employees who were interested, the vast majority (84%) were either "highly" or "somewhat" satisfied with their current choice of health plan.
A similar question was asked of the employers, and 46% were found to be "receptive" while 31% were "unreceptive." Of those who were receptive, 80% said they would be likely to switch if there were no negative tax consequences for their companies or their employees. Employers underestimated how interested their workers would be in the new approach – 45% thought their workers would be unreceptive, while only 40% thought they would be receptive.

"The Commonwealth Fund put its own spin on its survey results."
Commonwealth Fund. The Commonwealth Fund released a survey in January 2000 called "Listening to Workers."27 It surveyed some 5,000 adults from January to May of 1999 to ask about their experience and preferences in acquiring health insurance. The key question and breakdown of responses are shown in Table I:
This survey provides an interesting example of political spin in the way it reports its results. In the narrative, the authors take dead aim at the KPMG study and say:
The vote for employers, rather than direct purchase, appears at least in part to be a vote for group coverage and the value of having a group sponsor when selecting health plans. These findings speak against a move by some employers to convert plan sponsorship to a defined "contribution" in which employees would be on their own when arranging coverage. A significant majority – 67% – wanted some form of group coverage, either through employers or government.
That's one way to spin the results, but quite a stretch for several reasons:
- The question doesn't really test the interest in Defined Contribution. Unlike the KPMG survey, it says nothing about employers paying most of the premium but implies that employees would have to pay out of their own resources.
- The question omits any possibility of non-employment groups being formed to help find coverage and retain marketing efficiencies.
- Combining support of government programs and employer-sponsored care as forms "of group coverage" is peculiar. It is doubtful that people on Medicaid consider themselves enrolled in "group coverage." It would be more logical to combine employer-based and individual coverage as forms of private insurance, supported over public programs by 72% of the respondents. Certainly private individual coverage and private employer coverage have more in common than either does with Medicaid.
- It is far more interesting that only 56% of people who currently have employer-based coverage think that is the best way to get coverage in the future. Over one-third (35%) would prefer something different.
- A plurality (31%) of people currently in public programs would prefer direct purchase, and only 22% would choose to continue in a public program.
"The small to mid-sized companies are the ones most eager to find a new way to deal with health coverage."
Booz-Allen & Hamilton. More recently, the consulting firm of Booz-Allen surveyed Fortune magazine's "100 Best Companies to Work For" and found "all but a few were anticipating a shift to defined-contribution systems, which would save them millions of dollars in administrative costs by taking them out of the selection and retailing process." One of the authors, Vice President David Knott, said, "We believe the move to defined-contribution health plans is no more than three to five years away. Within 10 years, the defined-contribution system will be as common in health care as it is in retirement planning."28
Notably, these surveys focus on larger employers. Yet they are the very ones that currently have sophisticated human resource departments and can do a relatively good job of administering a health benefits program.29 The small to mid-sized employers are the ones that are especially hard-pressed. The car dealers and plumbers and print shops with 100-500 employees can't afford professional benefits management and are the most eager to find a new way.
[page]One big question in evaluating a Defined Contribution approach is the tax code. Few if any companies would choose the Defined Contribution approach if it meant that employees would have to pay taxes on the employer's contribution. According to Lewin and Associates,30 the current tax exclusion for employer-provided benefits equals about 40% of total outlay – total spending for employer-sponsored coverage in the year 2000 is estimated at $356 billion, and the federal and state revenue loss is $141 billion. Making these contributions suddenly taxable would eliminate an enormous benefit for workers and would effectively prohibit a change.
"One big question in evaluating a Defined Contribution approach is the tax code."
Until recently, most observers thought that current tax law would need to be changed to allow for Defined Contributions. Much of the discussion, both for and against, assumed that workers would receive the funds, pay taxes on the money, and be free to spend it on things other than health insurance. Those opposed to the idea warned of a substantial increase in the numbers of uninsured under such a scenario. Those who supported Defined Contributions were prepared to seek a change in the tax code to treat employee-chosen health plans the same way employer-chosen plans are treated.
Now it is apparent that these concerns were misplaced. Defined Contributions can take place under current tax law. Section 106 of the Internal Revenue Code says simply, "Gross income of an employee does not include employer-provided coverage under an accident or health plan."31
The IRS issued a ruling in 1961,32 clarifying Section 106. It said in part:
The employer may contribute to an accident or health plan either by paying the premium…or by contributing to a separate trust or fund…which provides accident or health benefits directly or through insurance to one or more of his employees. For those employees who are covered by a group policy through their employment, the employer pays his share of the premium directly to the insurance company. For those employees who are not covered by the employer's group policy but have other types of hospital and medical insurance for which they pay the premiums directly to the insurers, the employer pays a part of such premiums upon proof that the insurance is in force and is being paid for by the employees.
1961 was a long time ago; does RR 61-106 still apply? In a 1988 decision in Adkins v. United States, the U.S. District Court for Northern Ohio33 confirmed that ruling in deciding that a lump sum payment from an employer that was not restricted to health coverage was taxable income, even if the money was intended to help employees pay for coverage. The government argued that the employees had "unfettered discretion to do what they please with the monies," so the payment did not fall within the Section 106 exclusion. The Court agreed saying:
Section 106 clearly applies to contributions made by the employer to hospital, medical and accident benefit insurance programs, trusts or funds. Section 106 does not contemplate, nor infer, direct payments to the employee.
This decision was later upheld on appeal.
[page]While the tax code seems favorable to a Defined Contribution approach, other sections of federal law create severe obstacles. The essential concept of Defined Contribution is not only that employers will have better control over their health care costs, but also that employees will be able to control the resources available to them.
Employee resources may include an employer contribution, of course, but may also include their own funds, federal and state tax advantages, funds from a spouse or a spouse's employer, in some cases direct payments from government programs or charitable organizations and refundable tax credits.
Defined Contribution assumes that the worker can merge all those resources into a single package and purchase coverage in keeping with his or her values and priorities. Some workers are more comfortable with risk than others. Some have greater family responsibilities. Some have different health care needs.
"Two federal laws – ERISA and HIPAA – present problems in switching to Defined Contributions."
Defined Contribution also is intended to solve the problems of portability and accountability. As with pension programs, Defined Contribution in health care means that workers "own" their own policies. They no longer "borrow" the coverage from their employer or lose it once the employment stops. The worker, not the employer, controls how funds are invested – in this case, in a health program rather than a retirement fund. As with 401(k) retirement accounts, workers and health insurers may want to enter into a long-term contract for coverage. The insurer would be able to reduce its marketing costs, and the worker would have continuity of coverage without fear of annual renewal decisions. Defined Contribution implies health coverage that is "personal and portable."
A Defined Contribution environment would be initiated and partly supported by the employer, but the coverage would be individualized to the needs and resources of each worker. Unfortunately, federal and state law chops the insurance market into discrete markets, with very different rules for each. Substantially different rules apply to individual (also referred to as "nongroup" coverage), small group, and large group insurance. Some laws cut across even these categories. Some apply only to groups with at least 20 or 25 employees, while others apply only to groups with fewer than 50 employees.
Two federal laws present particular problems in switching to Defined Contribution: the Employee Retirement Income Security Act of 1974 (ERISA) and the Health Insurance Portability and Accountability Act of 1996 (HIPAA).
ERISA. ERISA – the Employee Retirement Income Security Act of 1974 – may be one of the most widely misunderstood laws on the books.34 ERISA governs "employee welfare benefit plans," which are defined as: "(A)ny plan, fund or program…established or maintained by an employer or by an employee organization…for the purpose of providing for its participants or their beneficiaries, through the purchase of insurance or otherwise, medical, surgical, or hospital care or benefits, or benefits in the event of sickness, accident, disability, death, or unemployment."35 This definition applies to all employers, regardless of size, whether they acquire benefits through an insurance company or provide them directly. The only exceptions are church and government plans.36
While nothing is ever certain until the Supreme Court says it is so, a Defined Contribution system clearly would be a "program…established… by an employer…for the purpose of providing…medical, surgical, or hospital care or benefits." It is, therefore, an "employee welfare benefits plan," subject to ERISA.
HIPAA. ERISA regulations are minimal, mostly involving plan disclosure and reporting and fiduciary responsibilities. HIPAA – the Health Insurance Portability and Accountability Act of 1996 – is another story. HIPAA was written as an amendment to ERISA, and so takes ERISA's definitions as its starting place. For example, a "group health plan" is defined in HIPAA as "an employee welfare benefit plan to the extent that the plan provides medical care…to employees…directly, or through insurance, reimbursement, or otherwise."37
"Despite having 'Portability' in its title, HIPAA does not deal with portability at all."
Briefly, HIPAA requires that insurers "guarantee issue" all products available in the small group market, limit the waiting period for preexisting condition coverage, and credit prior coverage towards the waiting period.38 An insurer may set premiums according to a group's experience, but may not vary premiums for individuals within the group based on health status. Presumably, premiums may be varied for "similarly situated" individuals, based on demographic factors other than "health status" such as age, sex, geography and participation in health promotion programs.39
HIPAA also requires states to enable certain eligible individuals leaving group coverage to join an individual plan without new underwriting. States may do so in a variety of ways, including mandatory guaranteed issue of individual coverage, requirements that insurers offer some limited guaranteed issue plans, enrollment in a state high-risk pool, or states can default to federal regulation if they fail to act. To be eligible, an individual must have had 18 months of prior group coverage with no gaps longer than 62 days and must have exhausted any COBRA continuation opportunities.
Despite its name, HIPAA does not deal with "portability" at all. It does not provide for individual plan ownership, or allow workers to keep their coverage when they change jobs. HIPAA in fact locks in the employer as the locus of coverage. It is solely the employer who decides what kind of coverage to purchase and what sort of benefits will be covered. All HIPAA does is limit the ability of employers and insurers to medically underwrite new enrollees.
"True Defined Contribution appears to be impossible under current law."
HIPAA's guaranteed issue provisions may have increased instability in the market by providing a perverse incentive for the smallest employers to enter and exit the market as the needs of their employees change. Since every carrier must offer all their products to all employers, it is easy for an employer to purchase rich benefits during times of special need and drop coverage or go to a cheaper plan when the need passes.
HIPAA also makes Defined Contribution difficult by reinforcing the wall of separation between "group" and "individual" insurance. This is a meaningless distinction at best. When a worker purchases health insurance coverage, the money must come from somewhere, presumably from his job – the same source as if the employer purchased the coverage on his behalf. There is only one difference: when the employer buys it, there is a huge tax advantage amounting, on average, to 40% of the cost of the coverage. Other state and federal regulations controlling individual, small group and large group health insurance are substantially different as well.
Thus, to own their own policies and take the coverage with them from job to job, individual workers must have "nongroup" coverage. But if an employer contributes to the cost of the premium, and the employee wants to enjoy the exclusion from taxes, the coverage is defined as "group." So, true Defined Contribution appears to be impossible under current law.
Two caveats should be noted here:
- A few companies are exploring other sections of the tax and benefits laws for creative ways of making Defined Contribution possible. One firm is looking at using a "dual purpose profit-sharing program," possibly in combination with a voluntary employees benefit association (VEBA or 501(c)9). This may enable employees to withdraw profit-sharing funds on a tax-free basis to purchase health insurance or health care services. Another company believes it can use a combination of Section 125 and Section 105 to create tax-advantaged "personal care accounts" in which unused funds may roll over to pay for future health care expenses. These or other approaches may be perfectly legal and achievable, but most employers will probably not rush to embrace them until it is well established that the product falls comfortably within existing laws and regulations. As with 401(k)s, the first firms to package and market such a new approach may be very successful indeed.
- There is a widespread and growing consensus in Congress that refundable tax credits are one way to level the playing field between employer and individual insurance, and to encourage more people whose employers do not offer coverage to purchase insurance. If a tax credit were substantial enough – equaling at least 40% of premium cost – some employers might decide to stop offering coverage and let their employees purchase insurance on the individual market. Such a credit would be identical to the existing tax advantage provided to employer-based coverage, except it would be more fair to lower-income employees. The main problem would be that some workers might ignore the 40% subsidy and still prefer to spend the money elsewhere. To address this concern, Congress could include a provision that enables employers to set aside a sum of money that could be used solely for health care costs. Doing this would create an almost perfect Defined Contribution scenario.
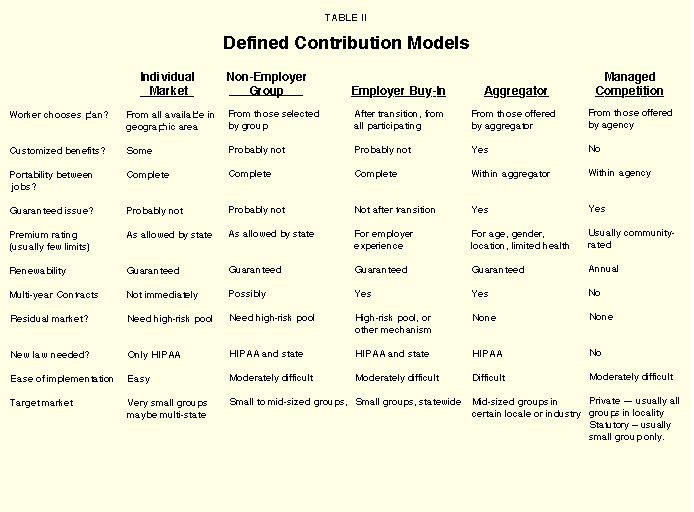
Despite the regulatory problems, much work and money are being invested in developing models and products to make Defined Contribution possible. In some cases, the models go as far as they can under current law. In other cases, the models show what the market could look like if the laws were reformed. In broad strokes, these models fall onto a continuum between the pure individual, nongroup market at one end, and a "managed competition" model at the other. The important variables between the two ends of the spectrum include: (a) the degree of individual ownership and portability; (b) the level of employer involvement in plan design and carrier selection; (c) the barriers to entry for competing carriers; and (d) the need for regulatory changes. Table II summarizes the characteristics of five models.
"Despite the regulatory problems, much work and money are being invested in developing models and products to make Defined Contributions possible."
The Individual Market Model. Today's individual market is much maligned by policy makers and employers. In truth it is far better than most observers realize, but not as good as it needs to be. Because of the extraordinary tax advantage provided exclusively to employer-based coverage, anyone who can possibly access group coverage will do so. Those remaining to purchase individual health insurance are generally people too ill to work, those with uncertain incomes, those with poor employment records, the semi-retired or fully retired, seasonal workers and those employed in high-risk jobs that group carriers don't want to cover.
The people in the individual market are older, sicker and poorer than those in the group market.40 They are also unsubsidized by either their employers or by the government, and collecting their premiums is a major challenge. Lapse rates are high as people acquire coverage when they have the money, and drop it when they run out of funds or lose the extra income from seasonal overtime. Underwriting and marketing expenses are very high, as carriers use the services of insurance agents to screen for egregious risks.
Despite all of these problems, individually underwritten coverage is fast becoming more affordable than group coverage, especially small group coverage. HIPAA has made it possible for groups to remain uninsured while the workers are healthy and purchase coverage only after someone gets sick or pregnant. Other cost-increasing regulations also are more prevalent in the small group market. For example, states often apply more mandated benefits, such as those requiring coverage for substance abuse or infertility treatment, to the small group than to the individual market, and states are more likely to apply rating restrictions to the small group market. Few of these costly requirements apply to the large group market, which is often defined as employers with 50 or more workers.
In its purest form, Defined Contribution would allow employers to make funds available to employees, who would use that money to purchase coverage in the individual market. The money would remain tax-advantaged because it would be available solely for the purchase of health insurance. Employers might reimburse their workers for paid premiums, or they might use payroll withholding and send payments directly to the employee's chosen carrier.
The employee would choose from any insurance plan available on the market and would be the policy holder. If the worker changed jobs, he or she would continue the exact same insurance plan, paying premiums directly from his or her own resources. When the worker got a new job, the new employer would make the contribution it could afford to the same plan.
"In its purest form, Defined Contributions would allow employers to make funds available to employees, who would use the money to purchase individual coverage."
In such a system, both the worker and the health plan would have an interest in providing long-term contracts for coverage to reduce the costs of underwriting,41 marketing, retention, and re-enrollment. The insurance plans would use underwriting to set an appropriate premium at enrollment, and the employer would adjust its contribution accordingly. But once in the plan, the worker would no longer have to worry about rate spikes due to changes in health status. Premiums would increase based only on overall trend and possibly increasing age of the insured.
Advantages for Employers: This model takes the employer out of the business of choosing and managing health care plans, lowers administrative costs and probably increases employee morale. The firm's contribution can be determined by business resources and labor market demands. The responsibility of the firm would be limited to using payroll withholding for the employee contribution and forwarding that along with the firm's contribution to the health plan chosen by the worker.
Advantages for Employees: Workers have access to the full range of health plans available on the individual market and can customize their benefits according to their needs and resources. They are the policy holders, so the plan is accountable directly to them, and the coverage is guaranteed renewable, so it should be permanent as long as premiums are paid. Portability is absolute, unless a new employer isn't offering its own group plan.
Advantages for Carriers: Carriers gain access to a very attractive new population made up of active workers who are generously subsidized by employers and by government. Many of the costs associated with the current individual market, such as retention and premium collection, are solved. Plus, carriers should be able to relax their underwriting restrictions for this population.
Disadvantages: The intersection between employer payment and worker ownership creates severe regulatory problems. Employer payment may mean the coverage is regulated as "group," even though individual ownership means it is "individual." There would likely have to be new legislation to resolve this conflict.
While carriers might relax their underwriting, they would still want to charge premiums based on age, sex, geography and possibly health status. Having risk-based premiums would make higher-risk people more attractive to cover, but employers would need to adjust their contribution accordingly. There would also need to be a high-risk pool or some other "residual market" for very high-risk employees who are priced out of coverage.
Some workers will not want to shop for coverage on the open market, so employers would need to provide a default plan for people unwilling or unable to find their own health plan. Plus, individual enrollment will add marketing costs over what employers currently incur.
Non-Employer Group Coverage Model. In this model, the employer's role is exactly the same as above, but to enjoy the marketing efficiencies of group coverage, workers would band together for joint purchasing arrangements. Typical sponsors might include fraternal organizations, church groups, homeowners' associations, credit unions and labor organizations.
"To enjoy the marketing efficiencies, workers could band together for joint purchasing agreements."
The members of these groups would collectively shop and negotiate for coverage, seeking discounts or added services from carriers in exchange for bringing a large number of customers to the table. The individual would still be the policy holder, and coverage would remain constant despite employment changes. The employer would still send its premium contribution plus any payroll withholding to the plan of the worker's choosing.
Advantages: Non-employment groups might actually be better than employer groups for marketing purposes. Other forms of group enrollment involve relationships that last longer, or may be larger than all but a few employers. People often belong to a church or fraternal organization for their adult lifetimes, and the numbers of people involved in a credit union or labor organization can dwarf most employers.
The coverage would be fully portable and independent of employment. Very likely, long term contracts would evolve.
Disadvantages: The group shops for and selects coverage, much as employers do today. This removes the worker/consumer from the most powerful of tools: the ability to choose the plan most in keeping with personal needs and resources.
The arrangement runs into many of the same regulatory problems as the Individual Market model. Plus, some states ban such arrangements for not being "true groups," a problem that is magnified if most of the premium is coming from the employer.
Employer Buy-in Model. This model attempts to combine the best elements of the group and individual markets. It starts out with the employer choosing a health plan for the entire group. But after a transition period, the coverage converts to individual and employees may choose to stay with the existing carrier or switch to another.
The coverage is then "owned" by the individual, and the usual renewal and underwriting rules for new enrollees apply. Only carriers who are willing to convert a block of group business into nongroup policies would be eligible to participate.
Advantages: Both employers and insurance companies must be comfortable with the initial enrollment and rating procedures. Carriers know that they will enroll the whole group, which may include a mix of risks, and that initial premiums will be set on a group basis. Employers will not have to do anything differently than before, other than communicate to their employees that after some period of time (three years is most commonly suggested), they will convert to nongroup coverage.
The comfort level for employees should also be high. At first they don't have to do anything, but they will convert to nongroup coverage after three years. If they want to stay with the same plan at that time, they are free to do so. If they prefer a different plan, they will be free to shop for something else.
"The Employer Buy-in Model attempts to combine the best elements of the group and individual markets."
Disadvantages: As with most of these models, regulatory obstacles must be overcome. Beyond that, potential selection problems arise with this and most of the models. In this case, the highest-risk employees may stay with the employer's original carrier, while lower-risk employees shop around for a better deal. To address that problem, employers may want to risk-adjust their contributions, so that higher-risk workers get a larger contribution than do low-risk workers and each group receives a contribution appropriate to the premium they will be charged. Such adjustments may be difficult to perfect in an open market in which different insurers use differing methodologies for setting individual premiums. Another way to address the issue and discourage annual plan-hopping could be with longer-term contracts in which the insured makes a commitment of three years or so – enough time to smooth out most acute care episodes and ensure enrollment stability.
The Aggregator Model: The aggregator model may be one way of resolving some of the enrollment and rating problems mentioned above. The aggregator acts as a third-party trust to facilitate the collection of monies and choice of plans. Aggregator firms will offer a variety of health plans, hold both employer and employee premium contributions and provide a marketplace in which employees can decide how to spend their health care dollars.
These firms42 typically use an e-commerce approach to plan selection, so plan information is displayed and enrollment completed online. They may select the carriers that participate, using criteria such as ability to process applications and claims electronically, 24/7 customer service information and minimal underwriting. They also may negotiate discounted premiums to enable the carriers to access this new market. Aggregator firms might also risk-adjust the employer contribution to accommodate age, sex, geographic and even health status variations among employees.
An aggregator firm would hold a contract with the employer, very much as employers choose a 401(k) administrator, and might even be partially paid by the employer for the value of the health plan administration services provided. These firms would most likely serve a large number of employers and target their services at specific geographic areas or industries. It is possible that business coalitions or industry associations would form such a firm to service their membership.
"An aggregator firm acts as a third-party trust to facilitate the collection of monies and choice of plans."
But while the employer makes a contract with the trust to provide these services, the employee is the policy holder. There is no direct relationship between the employer and the health plan. If a worker leaves his or her job, the coverage continues as is, with the trust now collecting the premium either directly from the employee or from the employee's new employer. Alternatively, the employee might deal directly with the carrier and discontinue the relationship with the trust.
Advantages: The aggregator serves as a marketplace for plan selection, risk adjustment and resource consolidation and allocation. It may screen the carriers that participate, according to certain underwriting and customer service criteria. Much of this should be backroom accounting and invisible to the worker/consumer, who knows simply that he or she has certain resources and may use them to choose among several plan and benefit options.
Employees will be able to select among the same plans, whether they are working or unemployed. There should be complete portability, provided the old and new employer both use the same aggregator.
The employer simply chooses an aggregator and pays out a sum for each employee. Even the usual employee questions and complaints, normally fielded by company HR staff, are addressed to the aggregator. Use of the Internet should lower marketing and enrollment costs.
Carriers should be attracted by the minimal marketing effort required and access to an extremely desirable population.
Disadvantages: Again, the blending of group and nongroup coverage is a large regulatory problem, as is the possibility that the aggregator will be treated as a Multiple Employer Welfare Arrangement (MEWA). Portability could be lost if two employers use different aggregators, or use none at all. Assuming the regulatory problems are solved, a new employer should be able to make payments to the aggregator, even if the company has no other relationship with the aggregator.
Private and Statutory Managed Competition. Managed competition may take two forms. It may be enabled through legislation, or it may be set up by employers as a cooperative program. In either case, it is based on the belief that there are efficiencies to be gained through the concerted effort of a large number of employers, and an agency selects the participating carriers and negotiates conditions of participation on behalf of the employers. There will usually be an annual open enrollment period, at which time every worker can change plans. In some cases, the open enrollment provision is continuous, so that workers can change plans at any time during the year.
"It is not clear that there are savings under managed care."
Statutory managed competition programs are usually aimed at the small group market in a specific geographic area. They often have a social mission beyond merely helping employers access coverage. They may be created in the hope of reducing global health care costs or increasing the numbers of uninsured individuals. They may also include waivers of certain regulatory restrictions, such as mandated benefits, premium taxes or enrollment criteria. On the other hand, the agency may actually add restrictions beyond those of existing state law, such as standardizing benefit plans or restricting price discrimination.
Private managed competition programs are similar except they are organized without the benefit (or burden) of enabling legislation. Like their statutory brethren, they typically feature an agency that "manages" the participating health plans.43 Unfortunately, this management process often results in standardized benefit programs, which misses the point of individual choice.
In both cases, the agency is the representative of the employer and acts in place of the employer in negotiating with the health plan. The individual worker is not the policy holder, and coverage will terminate along with the worker's employment.
It is not clear that there are savings under these models. Managed competition may simply add a layer of administrative and regulatory complexity between the employer and the state insurance department. The agency overseeing managed competition might add its own mandates and regulatory obstacles and actually diminish the ability of individuals to choose how to spend their resources. The track record of states that have tried this approach locally, notably Florida, is not encouraging, and employers are rightly concerned that a managed competition approach could easily lead to mandatory participation.44
Advantages: Employees of smaller firms get a far broader choice of health plans. Employers get the services of an agency with more managerial expertise than most small employers possess. There may be some cost savings as a result of joint purchasing, though the cost of running the agency may offset this. In theory, the competition between health plans should lead to greater efficiency, lower costs and higher quality.
Disadvantages: The potential savings and efficiencies are often overstated, and the worker still has only a one-year (or less) contract with the carrier, with no continuity or portability. To the extent that managed competition uses community rating, it provides carriers with a strong incentive to avoid higher-risk individuals. It also enables workers to choose a comprehensive plan when their health care needs are greatest and a less comprehensive plan when their need is less.
[page]Even if the group/nongroup issues are resolved and employers are allowed to contribute to a worker's individual premium, a number of market and regulatory issues will remain. We cannot anticipate the best resolution of these issues. To a large extent, the market will have to evolve through trial and error, and the regulatory environment will respond to market conditions. But addressing the issues requires a clear understanding of the dynamics of health insurance pricing and administration.
1. Should Employers Vary Their Contributions by Risk Factors?
"The issue of adjusting employer contributions to reflect the relative cost of the employee is complex."
It is often argued that employer plans are community-rated within the group. That is, the entire group may be experience-rated, but to the extent employees pay for some portion of their premium, they are all charged the same. But that is only partly true. Employers currently provide much greater nominal benefits to workers with families than they do to single employees, even though it may be less as a percentage of the cost of coverage. For example, an employer may pay 90 % of the cost of coverage for a worker, but only 75% of the cost of dependent coverage. If the per capita cost is $1,000 per year, Employee A with a spouse and two kids may get an employer contribution of $3,100, but Employee B, who is single, gets a contribution of only $900. Employee A is getting a much higher nominal benefit than Employee B, but the employer is paying 90% of Employee B's coverage and only 77.5% of Employee A's coverage.
Beyond the issue of family vs. single coverage, there is evidence that employers account for health differences between workers by adjusting wages. Federal Reserve economist Louise Sheiner has concluded that the extra cost of covering higher-risk workers is often reflected in lower wages for those workers.45
So the issue of adjusting employer contributions to reflect the relative cost of the employee is complex. Even defining the meaning of "equity" isn't easy. Is it "discriminatory" to adjust the contribution based on known actuarial risk factors, or is it discriminatory not to do so? One solution would be for employers to base the contribution on a percentage of the worker's cost, thereby accounting for the extra premium paid by higher-risk, older workers. But that would sacrifice one of the attractions of Defined Contribution: predictability. It would also encourage waste and inefficiency as the employer absorbs much of the excess cost of an inefficient plan.
"Carriers' risk-adjustment methods cannot be as complicated or intrusive as those in use today."
Another solution that will surely be discussed is requiring carriers to "community rate" premiums, thereby eliminating the need for employer adjustments. While this approach is appealing in its simplicity, its very simplicity makes it unworkable. As long as insurers are receiving the same premium from all customers, they will always have a strong incentive to attract healthy customers and to repel high-risk customers. There are an infinite number of ways to structure a program so that it is attractive to the young and healthy but less attractive to others. This is especially true in a multiple choice environment. The point of risk-based rating is to make high-risk individuals more attractive by giving them the resources to pay higher premiums.
The more likely solution is to use simplified rating adjustments, based on age, sex, geography and perhaps a short list of health conditions that both employers and insurers can use to synchronize contributions and premiums. Such adjustments will need to be transparent and easy to calculate to enable electronic enrollment and instantaneous premium quotes.
2. How will the insurance industry respond? Will it insist on applying individual-market underwriting standards? Will it continue using minimum participation rules?
As mentioned above, the kinds of extraordinary underwriting currently in use in the individual market would be inappropriate for this attractive new market. While carriers may want to use some form of simplified risk-assessment for setting premiums, it cannot be as complicated or intrusive as those in use today, and due to HIPAA it cannot be used to deny coverage.
On the group side, carriers often have minimum participation and contribution requirements to qualify employers for coverage. A carrier might require that 75% of a group's employees participate and that the employer contribute at least 50% of the premium. These participation rules would not make sense in an individual choice environment, though the minimum contribution rules might still be applied.
Employers or third party trusts might insist that concessions on underwriting and participation standards be a condition for health plans that want to access their business.
3. How can a Defined Contribution plan retain the marketing and administrative efficiencies of the current employer-based system?
Two oft-cited advantages of employer-based coverage are the administrative and marketing efficiencies of dealing with a large group and the ability to pool risks. These advantages are overstated. For example:
Risk Pooling. Most employers are not especially good risk pools, if risk pooling implies bringing together a large number of people of varying risks and backgrounds to share the cost of an occasional large claim. This is what an insurance company is designed to do, not what an employer is for. For one thing, workers all share one characteristic: they are able to work and so they are all in reasonably good health. For another, employees of a single employer are likely to be more like one another than the general population. Workers in a bicycle shop are more likely to be young bicycle riders, workers in a Chinese restaurant are more likely to be Chinese, workers in an auto repair shop are more likely to be male and teachers in an elementary school are more likely to be female – certainly more likely than would be true for the general population. Finally, a "risk pool" of 25 or 100 or even 1,000 workers is small compared to an insurance company that covers possibly a million or more people. A bout of influenza can easily sweep through a 100-person "pool" leaving very few unaffected people to pay the claims of the ill. It is better to have insurance companies pool risk than to rely on employers.
"It is better to have insurance companies pool risk than to rely on employers."
Administrative efficiencies. Larger employers are often thought to be more efficient than smaller ones, and certainly more efficient than the nongroup market. This idea is based on the notion that loss ratios (that is, the percentage of premium that is paid out in claims) are higher for larger groups. Very large groups may have loss-ratios of 93%-95%, mid-sized groups 85%-90%, small groups 75%-85% and individuals 60%-75%. Once again, there is some truth here, but it is often overstated. One of the reasons employer groups appear to be more efficient is that the employer performs many of the administrative functions an insurer must do for small groups and individuals. With the exception of marketing and underwriting, all of the same tasks (keeping enrollment records, distributing plan information, answering employees' questions, collecting premiums, processing claims, responding to appeals, etc.) need to be performed regardless of the size of the group. But larger employers are more likely to have human resource departments that absorb many of these responsibilities. The tasks are still performed and paid for, but they never become part of the insurer's administrative overhead. They are paid directly by the employer instead. Certainly it is more efficient to print 1,000 plan brochures than 50, but these kinds of bulk savings are trivial compared to the cost of answering worker questions, which a large employer does in-house and the insurer does for a smaller employer.
Marketing Efficiencies. Here there is a substantial difference. Engaging a broker to talk to one decision maker who can enroll 1,000 people is clearly more efficient than having the same broker talk to each of the 1,000 people. Commissions are much higher as a percentage of premium for smaller employers and nongroup insurance. There are two ways a Defined Contribution plan might solve this problem. One is through Internet marketing, combined with a strong customer service operation. The other is through long-term contracts which spread the cost of individual marketing over five, 10 or even 20 years.
It is doubtful Defined Contribution could succeed without the Internet. There is simply too much information to be successfully managed with paper, and the cost of moving all the paper back and forth would be prohibitive. The Internet is an ideal medium for this kind of decision making. Not only can it organize and present large amounts of information coherently, but it also can customize benefits and instantly calculate and compare the costs for each worker's unique situation. Internet enrollment is another major reason for keeping underwriting questions simple. But an effective service will never be able to answer all questions online, so it must be supplemented with a dial-in customer service operation staffed by knowledgeable, personable representatives.
4. How will employers communicate the change to their workers, especially in a tight labor market? What must employers do to ease the transition?
"Employers need to be sensitive to the fact that workers often view any change in benefits as a 'take away'."
Surveys repeatedly illustrate a high level of unhappiness with the current health benefits arrangement. A recent Watson Wyatt survey of very large (average size 16,000 workers) employers found that 88% of them believe their employees rate their health plans "average to poor," while only 10% consider them "excellent."46 So the potential to communicate these changes effectively should be very high. Still, it is a big change, and workers often view any change in benefits as a "take-away" rather than an improvement.
Employers need to be sensitive to that view, and avoid forcing workers into something they don't understand. That means there should be a transition period during which the conversion is voluntary, with a fallback plan available for those who are nervous about change or are unwilling or incapable of making effective choices.
Workers also may be anxious about being at the mercy of the market. Employers should make sure that the insurance companies are willing to accept all comers, or that a viable high-risk pool is available for those few workers who may be priced out of enrollment.
With these assurances, the process could be an exciting one, as workers take control of their own resources. The conversion can be upbeat, and can include a health fair or a benefits bazaar in which workers can comparison shop for plan options and think about how they might best spend their money. This should be a festive occasion that opens up a whole new world for empowered workers.
Admittedly, Defined Contribution plans introduce a host of new issues for employers. Different companies will try out different models, and some will work better than others. Over time, the questions will be answered and a new market will develop, one in which patients are empowered to choose their own health plans and to change plans if the first isn't satisfactory. Health plans will focus on pleasing the individual customer, rather than the employer. They will enter a new era of customer service and information or risk losing business. Employers will concentrate on what they do best and leave health care to those who are good at it.
[page]Over the past 50 years, employers have done a good job of voluntarily providing coverage to the American people. The vast majority of Americans get their health insurance through the employer-based system, leaving the government responsible for covering those not associated with an employer – the poor and the elderly.
"Our system of third- and fourthe party payment has distorted the economics of health care."
Unfortunately, this system of third- and fourth-party payment has distorted the economics of health care. Consumers are so far removed from the financial consequences of their decisions that costs have risen dramatically. And working people whose employers do not provide coverage are doubly disadvantaged – once because they pay prices inflated by employer and government subsidies, and again because they get no similar subsidy. The two groups of people who receive the least support in our system are the uninsured and those who purchase individual coverage. Yet the latter group is older, poorer and sicker than people with employer-based coverage, and the former is younger, sicker and poorer. In either case, the very people who most need help get it least.
For the past 25 years, employers have wrestled with the consequences of this inflationary system. They have tried almost everything – self-funding their benefits to control reserves and lower administrative costs, redesigning benefits structures to emphasize outpatient treatment, requiring second surgical opinions and utilization reviews, increasing employee cost-sharing and switching to HMOs and other managed care programs. These changes have had some success in holding down costs, but usually the effects are short-lived. And they have created resentment on the part of employees who feel that needed services are being withheld.
Partly in response to the growing resentment among employees and providers, the federal government has enacted what it views as remedial legislation: COBRA, HIPAA, mandates for maternity coverage, mental health care, mastectomy hospital stays and currently the prospect of liability for bad outcomes through the Patients' Bill of Rights proposals. To employers, it seems that every year brings new regulations. Even if the Patients' Bill of Rights is defeated, it will be small consolation to many employers who expect the next Congress to add yet more requirements.
Employers spend a lot of money on health care, often $4,000 to $6,000 per employee per year, but they get little benefit for it in terms of employee morale. Employees have little sense of what these benefits cost, but they have great expectations that all services should be covered at little cost to themselves.
There was a time when employers were happy to divert some portion of the total compensation package out of wages and into health benefits. There was little difference in administrative burden, and providing health insurance meant a more productive workforce and less sick leave expense. Further, the fact that health benefits were excluded from income was a major advantage to workers.
Now employers are concluding that the regulatory and administrative burdens of managing benefits programs are too great. It is far easier to simply pay out the cash than it is to divert the funds into benefits. If they can find a way to do so while retaining the productivity advantages of health benefits, they will have a win/win situation.
This is what Defined Contribution is aimed at. Ultimately, employers will be able to simply write the checks for coverage – much as they write the checks for payroll. But the money will be available solely for the purchase of health insurance, so the productivity issues are addressed.
"The impact of Defined Contributions on employees should be profound."
The impact on employees should be profound. They will be able to choose the health plan that is most suited to their own needs, and "vote with their feet" if a plan doesn't perform as promised. They will make their own trade-offs in benefit design and cost-sharing, allowing them to take risk at the level with which they are comfortable. They will be able to keep the same plan as they change jobs, and even enter into long-term contracts with their health plan. They will be able to amend their benefit design as they go through life's changes – beefing up on maternity and pediatric coverage when they are young, switching to vision, dental and even long-term care coverage as they age. They will be able to save money when their expenses are low, and have it available when expenses get higher.
This is a rational health care system that can meet the needs of each family. It is not a one-tiered, or two-tiered or even five- or six-tiered health care system. It is a 270 million-tiered health care system that delivers exactly those services each individual demands. Now, that is a market-based system.
Greg Scandlen is a Senior Fellow with the National Center for Policy Analysis
[page]Greg Scandlen is a Senior Fellow in Health Policy. In this role, Mr. Scandlen writes studies and analyses on health policy issues, as well as opinion columns for such publications as the Wall Street Journal, Investors Business Daily, and the Washington Times among others. He also publishes a weekly health policy newsletter called Washington Weekly, which summarizes and critiques the important movements in national health policy.
[page]- Source Book of Health Insurance Data, 1980-1981, HIAA (Health Insurance Association of America), Washington, D.C., p. 12.
- Ibid.
- Health Care Financing Administration, Office of the Actuary, National Health Statistics Group.
- Ibid.
- Ibid.
- Social Security Bulletin, February 1976, p.13.
- Paul Starr, The Social Transformation of American Medicine (New York: Basic Books, 1982), p. 394.
- Terree P. Wasley, What Has Government Done to Our Health Care? (Washington, D.C.: Cato Institute, 1992), pp. 55-56.
- Aspen Systems Corporation, A Report to the Governor on State Regulation of Health Maintenance Organizations, for the Office of Prepaid Health Care, DHHS, Twelth Edition, 1990.
- Wasley, What Has Government Done to Our Health Care? pp. 71-72.
- Ricard J. Stefan, Acme Steel Company, Testimony before the Subcommittee on Commerce, Consumer Protection, and Competitiveness of the House Committee on Commerce, 102nd Congress, 2nd Session, February 5, 1992.
- Dean Coddington et al., The Crisis in Health Care: Costs, Choices and Strategies (San Francisco: Jossey-Bass Publishers, 1990), p. 85.
- Joseph A. Califano, "A Corporate Rx for America: Managing Runaway Health Costs," Issues in Science and Technology, Spring 1986.
- Quoted in William B. Schwartz, M.D., "Business Forum: Health Care Inflation; Cutting Costs Means Painful Choices," New York Times, May 8, 1988.
- HIAA, Source Book of Health Insurance Data, 1997-1998, p. 59.
- William M. Mercer/A. Foster Higgins & Co., Inc., cited in "EBRI Fact Sheet," Employee Benefit Research Institute, September 1998.
- Research on these issues is pouring out of academia. Some examples: Daniel Altman et al. examined public employee experience in Massachusetts and concluded that the 40% cost differential between HMOs and indemnity coverage can be attributed equally to risk selection and lower prices (NBER Working paper No. W7832, August 2000); on the other hand, David Cutler et al. looked at the treatment of heart disease in two data sets also from Massachusetts and concluded that "virtually all" of the cost differential is due to lower unit prices (RAND Journal of Economics, Vol. 31, No. 3, Autumn 2000).
- Even on a service as fundamental to managed care as encouraging the use of preventive care, the research is mixed. One study synthesized the research published between 1990 and 1998 (18 studies) and concluded that 37 % of the studies found higher use of preventive services under managed care, but 60 % found no difference. Kathryn Philips et al., "Use of Preventive Services by Managed Care Enrollees: An Updated Perspective," Health Affairs, Vol. 19, No. 1, Jan/Feb 2000, pp. 102ff.
- This is particularly true for high utilizers. See Benjamin Druss et al., "Chronic Illness and Plan Satisfaction under Managed Care," Health Affairs, Vol. 19, No. 1, Jan/Feb 2000, pp. 203ff.
- Atul Gawande et al., "Does Dissatisfaction with Health Plans Stem from Having No Choices?" Heath Affairs, Vol. 17, No. 5, September/October 1998. This is not a new phenomenon. Even the RAND Health Insurance Experiment in the late 1970s found that patients who were randomly assigned to HMOs were less satisfied than people who chose HMO coverage. Joseph Newhouse, Free for All? (Cambridge, Mass.: Harvard University Press, 1993), p. 347.
- Susan Marquis and Stephen Long, "Trends in Managed Care and Managed Competition, 1993-1997," Health Affairs, Vol. 18, No. 6, Nov/Dec 1999 pp. 75ff.
- Greg Scandlen, "New Study Shows 992 Mandated Benefits in the States," Health Benefits Letter #15, August 29, 1991. Susan S. Laudicina and Katherine Pardo, State Legislative Health Care and Insurance Issues: 1999 Survey of Plans, BlueCross BlueShield Association, December 1999, lists 1,391 state mandates. Also see John C. Goodman and Merrill Matthews, "The Cost of Health Insurance Mandates," National Center for Policy Analysis, Brief Analysis 237, August 13, 1997.
- As of 1994-95, 42% of all full-time employees were in defined benefits retirement programs, while 39% were in Defined Contribution programs, according to the Bureau of Labor Statistics. The Defined Contribution numbers are pulled down by the public sector, in which 86% of workers are in defined benefits programs and only 9% are in Defined Contribution programs. See Monthly Labor Review, "Defined Contribution retirement plans becoming more prevalent," Bureau of Labor Statistics, January 1999. Available at www.bls.gov/opub/ted/1999/jan/wk1/art03.htm
- "HR Execs Want to Empower Employees to Make Own Benefits Decisions," press release on survey from Benefits Access, Inc., Hartford, Conn., October 14, 1998.
- Sandra Lutz, "Healthcast 2010," PricewaterhouseCoopers, Fall 1999.
- "A New Direction for Employer-Based Health Benefits," KPMG, LLP, publication 99-12-05, November 1999.
- Lisa Duchon et al., "Listening to Workers: Findings from the Commonwealth Fund 1999 National Survey of Workers' Health Insurance," Commonwealth Fund, January 2000. See also www.cmwf.org.
- Philip Lathrop, Gary Ahlquist and David Knott, "When Consumers Rule: The Next Revolution in U.S. Health Care," Strategy+Business, reprint from Booz-Allen & Hamilton, March 2, 2000. See also article on the Booz-Allen & Hamilton Web site at www.bah.com/viewpoints/insights/health_rev_2.html.
- One little-noticed result from the Commonwealth Fund survey is the correlation between income and group size and support for continuing an employer-based system. When looking at firm size, only 48% of workers employed by firms with fewer than 25 employees think employers are the best source, while 62% of those in firms with at least 500 workers think so. Similarly with income, only 40% of people making under $20,000 think employers are the best source, while 58% of those making $50,000 or more do.
- John Sheils, Paul Hogan and Randall Haught, "Health Insurance and Taxes: Impact of Proposed Changes in Current Federal Policy," National Coalition on Health Care, October 19, 1999.
- 26 USCS Sec. 106 (a).
- Revenue Ruling 61-146, 1961-2 C.B. 25.
- Adkins v. United States (1988 ND Ohio) 693 F Supp., 88-2 USTC, 9437.
- Greg Scandlen, "Legislative Malpractice: Misdiagnosing Patients Rights," Cato Institute, Briefing Paper No. 57, April 7, 2000.
- 29 U.S.C. Section 3(1).
- 29 U.S.C. Section 4(b)1-2.
- P.L. 104-191, Section 706 (a)(1).
- For a good review of these provisions, and how they relate to state-based small group reform efforts, see Len Nichols and Linda Blumberg, "A Different Kind of 'New Federalism?' The Health Insurance Portability and Accountability Act of 1996," Health Affairs, Vol. 17 No. 3, May/June 1998.
- P.L. 104-191, Section 2701(b)(1,2).
- The individual market includes 29.6 % who are below 200 % of the poverty level and 18.8 % who are between the ages of 55 and 64, while the percentages for the employer-based market are 16 and 9.2, respectively. Deborah Chollet, "The Individual Market: Consumers, Insurers and Market Behavior." KFF, January 20, 1999.
- The term "underwriting" is often misunderstood, in part because it is used to mean many different things. It goes back to the early days of insurance, especially shipping insurance, when a few investors would evaluate the risk of each journey and decide whether to insure it by "writing" their names "under" the manifest and description of the voyage. For a readable description of the early days of the insurance industry, see Andrew Tobias, The Invisible Bankers (New York:The Linden Press, 1982). As used in this paper, underwriting means the evaluation of individual risk. Carriers may then decide what to do with that evaluation – charge less or more than average, add an exclusionary rider, or deny coverage altogether, depending on the controlling laws and regulations.
- There are at least eight companies working on developing this model, often with the support or involvement of major benefits consulting firms. These companies include Lumenos, Vivius, HealtheCare, MyHealthBank, Sageo, HealthSync and some others that are not yet named.
- One recent example is "HealthPass" in New York. HealthPass was organized by the New York Business Group on Health with the aid of a $1 million grant from the City of New York. HealthPass offers the employees of small companies a choice of four different carriers and 20 different benefit programs. More information is available at www.healthpass.com.
- Elliot Wicks, Mark Hall and Jack Meyer, "Barriers to Small-Group Purchasing Cooperatives," Economic and Social Research Institute, March 2000.
- Louise Sheiner, "How Do Wages Reflect Employer-Based Health Insurance Costs?" American Enterprise Institute, December 1999.
- Barbara Martinez, "Most Companies See Rising Cost of Health Care as Pressing Issue," Wall Street Journal, July 5, 2000.