Senator John Kerry has proposed a plan to radically reform the U.S. health care system. If he is successful, millions of middle-income families will be enrolled in Medicaid, the federal-state health program for the poor. Millions more will get their insurance through a system of managed competition modeled after the federal employee’s health system and similar to what Hillary Clinton proposed more than a decade ago. Most people would be forced from the private health plans they have today.
The ostensible purpose of Kerry’s proposal is to insure the uninsured. By some estimates as many as 44 million people lack health insurance at any one time. Sen. Kerry’s goal is to insure about two-thirds of them. The effort will be expensive, even by Kerry’s own estimate. We put the price of these reforms in excess of $1 trillion over ten years — an amount equal to almost $1,000 per year for every household in America.
Unlike the Clinton plan, Kerry’s program would not mandate employer-provided health insurance coverage. Instead, it would use economic incentives to induce people to voluntarily insure. But very little of those incentives will actually go to individuals. About 90 percent of the funds will go to state governments, employers and insurance companies. In a nutshell, the Kerry plan would use taxpayer dollars to encourage public and private institutions to persuade individuals to obtain insurance. Among the inducements:
- The federal government would pick up the additional cost of insuring Medicaid children if the states expand eligibility and increase enrollment.
- The federal government would pay the bulk of catastrophic health expenses if employers offer insurance to all employees and pay at least one-half of the cost.
- Additional subsidies would be offered to low-income people who insure through the managed competition system: small business employees, the unemployed, and people aged 55 to 64 years.
- And insurance costs would be limited to a percent of family income for everyone else who individually enrolls in the managed competition system.
President Bush has proposed tax relief for people who buy insurance on their own. In stark contrast, Kerry’s tax subsidies are trickle-down — people are supposed to get derivative benefits from checks written to others. Will this approach work?
More than half of the money in Kerry’s plan will be spent expanding Medicaid (for low-income families) and the SCHIP program (for low-income children). Prof. Kenneth Thorpe, Kerry’s health adviser, estimates that as many as 26 million new people will be enrolled. However, as the public sector expands the private sector will surely contract:
- Even Kerry assumes that for every 10 people who sign up, three people will lose employer-provided private insurance; and it could be much worse.
- Studies in the 1990s found that every additional dollar spent on Medicaid led to a reduction in spending for private insurance of 50 to 75 cents.
- More recent evidence suggests that private sector crowd-out is approaching one-to-one: Each new Medicaid enrollee is offset by one less person with private insurance.
Moreover, most of the private sector subsidies will go to people who are already insured; and employers will receive subsidies even if they fail to insure a single additional employee. Bottom line: It is entirely possible to spend $1 trillion and achieve no reduction in the uninsured.
Quality of care will suffer under the Kerry proposal. People who go from employer plans to Medicaid will have fewer choices of doctors, longer waits for care and some health care rationing. Those who join the system of managed competition will experience a different problem: Health plans will face perverse incentives to over-provide to the healthy and under-provide to the sick.
On the surface, managed competition sounds attractive. Each year, people could choose among competing health care plans — much like federal employees currently do. But the community-rated premiums charged bear no relation to actual health care costs. Healthy enrollees would overpay. Enrollees with high health costs would underpay. Thus health plans would have strong incentives to provide more services to profitable, healthy enrollees (in order to attract more of them) and fewer services to unprofitable, sick enrollees (in order to attract fewer of them).
Kerry explicitly rejects national health insurance, and wisely so. We have seen political pressures in other countries cause politicians to skimp on expensive, lifesaving technology even as they over-provide relatively trivial services to healthier people. And though Kerry avoids the political pressures of national health insurance, the end result may be the same because of the economic pressures of managed competition.
The plan will almost certainly lead to a new round of health care inflation. Federal spending alone will increase by more than $100 billion a year. But since there will be no increase in supply, the bulk of this new spending will buy higher prices rather than more health care. To make things worse, individuals will face perverse incentives to over-insure and over-consume.
For example, faced with virtually no out-of-pocket costs, the 26 million new enrollees in Medicaid will find no reason to show spending restraint. The bills all go to someone else. Premium caps mean that a poverty level individual will pay no more than $600 or $700 a year, with the excess premium subsidized by Uncle Sam. Given a decision to insure, the incentive will be to pick the most expensive plan available.
In an effort to hold down costs, Kerry’s advisers tout the benefits of “case management.” But in his acceptance speech at the Democratic convention, Kerry rejected all forms of managed care. He appears to have taken no position yet on Health Savings Accounts and other forms of consumer-directed health care.
Kerry’s original cost estimate was close to $900 billion over 10 years. Subsequently, he seems to have endorsed close to $300 billion dollars in savings, mainly by eliminating waste and inefficiency. Reading between the lines, it is tempting to conclude that Kerry really wants his plan to be paid for by the taxes he has promised to impose on taxpayers who earn more than $200,000 a year.
Beginning with the first full year of operation and ignoring phantom savings, we put the 10-year cost in excess of $1 trillion. But rescinding the Bush tax cuts for the “rich” will provide only one-third of that amount. For Kerry’s plan to succeed, new taxes for the middle class appear to be inevitable.
The Kerry plan would harm the economy. It would raise taxes on capital and lower workers’ take home pay. And because virtually all of Kerry’s subsidies are phased out as income rises, the plan would create new penalties for work. For example:
- The premium cap alone would add 15 percentage points to the marginal tax rates of low-income families — for every extra dollar they earn, they would lose 15 cents of premium subsidy.
- Assuming (as Kerry does) that employees reap the full benefits of employer subsidies and bear the full cost of their withdrawals, the small business tax subsidy would add 11 percentage points to the marginal tax rates of low-income workers, if they choose an average cost health plan.
- If they choose a high cost plan (because so little of the premium will come out of their own pockets), their marginal tax rate could climb 19 percentage points.
When these penalties are added to other marginal tax rates created by the income tax, the payroll tax and the withdrawal of other subsidies such as the Earned Income Tax Credit (EITC), overall tax rates for low-income families would soar to levels normally thought to apply only to the very wealthy.
A major problem with the current system is that tax subsidies for health insurance are arbitrary and unfair. But rather than move to a fairer system that treats equals equally, Kerry would create a slew of new subsidies that would make the current system even more arbitrary. Under the Kerry plan, people at the same income level would receive vastly different subsidies depending on their age, where they work and how they obtain insurance.
By design, the Kerry plan does not insure everyone. So who would be left out? The people most ignored are mainly middle-income families with incomes above 300 percent of the poverty level who buy their own insurance. Over the past decade, almost all the increase in the uninsured is accounted for by this group. Further, unlike people who get tax-subsidized insurance through an employer, these families must buy insurance with after-tax dollars. President Bush has proposed a tax deduction for this group, if they purchase insurance combined with health savings accounts. Kerry offers these families virtually no relief.
The structure of the Kerry health plans raises a number of intriguing questions:
- Why spend several hundred billion dollars on catastrophic insurance for millions of people (many with high incomes) who are already insured, while ignoring all of the non-poor uninsured who currently get no tax relief?
- Why spend billions to subsidize small businesses if they join an insurance system that doesn’t yet exist, while denying them those same subsidies if they buy insurance that is readily available in the marketplace?
- Similarly, why pay the cost of premium caps and other subsidies if individuals buy insurance that doesn’t yet exist, while denying them any relief if they buy insurance that is already available?
- And why spend billions enrolling middle-income families in Medicaid instead of using those same dollars to help them enroll in employer plans and individually-owned policies which they would probably much prefer?
There is only one explanation that sensibly answers all of these questions. The real purpose of this plan is not to insure the uninsured. The real purpose is to radically change our health care system.
[page]
Sen. John Kerry has proposed a plan to radically reform the U.S. health care system.1 If he is successful, millions of middle-income families will be enrolled in Medicaid, the federal-state health program for the poor. Millions more will get their insurance through a system of managed competition modeled after the federal employee’s health system and similar to what Hillary Clinton proposed more than a decade ago. Most people would be unable to remain in the private health plan they have today.
The Kerry plan would not mandate that employers provide health insurance coverage, unlike the Clinton plan of years ago. Instead, it would use economic incentives to induce people to voluntarily insure. Among the inducements:
- The federal government would pick up the additional cost of insuring Medicaid children if the states expand eligibility and meet their goals for increased enrollment, including enrolling 95 percent of children in families with less than 300 percent of poverty level income.
- The federal government would also pay 75 percent of the cost of catastrophic health expenses if employers offer insurance to all employees and pay one-half the premium costs.
There would be additional subsidies for many of those who insure through the system of managed competition, including:
- A refundable tax credit for small businesses that insure low-income employees;
- A 75 percent tax credit for workers between jobs and a 25 percent tax credit for workers age 55 to 64 years;
- And a limit to how much insurance could cost (6 percent of income at the poverty level, rising to 12 percent at 300 percent of poverty) for everyone else who individually enrolls.
"Sen. Kerry’s health plan will cost in excess of $1 trillion."
We put the price of these reforms in excess of $1 trillion over 10 years — an amount equal to almost $1,000 per year for every household in America (see Table I). This estimate differs in two ways from Kerry’s own estimate, calculated by Emory University Professor Kenneth Thorpe:2 First, Kerry's (i.e., Thorpe’s) most recent projection delays the introduction of the program by one year — making the first year’s cost zero. Second, Kerry is now projecting offsetting savings, most of which consist of the perennial promise to eliminate waste and inefficiency. Our projection includes 10 full years of operation and ignores phantom savings.3
[page]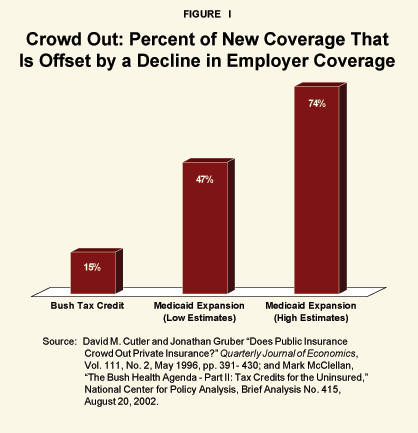
More than half of the cost of Sen. Kerry’s health plan will fund an expansion of Medicaid and SCHIP (State Children's Health Insurance Program).4 The goal is to insure almost 18 million additional people. The burden for taxpayers would be about $500 per year for every household in America. But what would the nation really get in return for assuming this extra burden?
A. Problem: Reduction in Private Insurance
“Expanding public insurance tends to crowd-out private insurance.”
Studies show that the expansion of “free” public insurance crowds out private insurance. This means that some people who are privately insured give up their private coverage because they have the opportunity to enroll in the public program. For example, people cease making contributions to an employer plan or they cease making premium payments for individually owned insurance. Or, employers of low-wage workers stop offering employer-provided insurance and instead pay higher wages because private insurance is a less valuable fringe benefit if there is a free care alternative.
The existence of such crowd-out means that the cost of expanding public insurance programs is much higher than people suppose, relative to the gain. For example, if for each new enrollee in a public program at least one person loses private insurance, there will be no net reduction in the number of uninsured, despite the higher taxpayer burden. If for every two new enrollees in the public program one person loses private insurance, the cost for each newly insured person will double.5
A study by Harvard University Professor David Cutler and Massachusetts Institute of Technology Professor Jonathan Gruber found that Medicaid expansions in the early 1990s were substantially offset by reductions in private coverage. They found that, for every additional dollar spent on Medicaid, private sector health care spending was reduced by 50 to 75 cents on the average.6 Thus taxpayers incurred a considerable financial burden, although little was accomplished. [See Figure I.]
Crowd-out apparently happened after SCHIP was implemented in 1997. Because of expansions of Medicaid and SCHIP, enrollment of low-income children in public programs increased from 29 percent to 33 percent. At the same time the percent of children from low-income families covered by private insurance fell sharply — from 47 percent to 42 percent.7 [See Figure II.] During this period, the percentage of children with private health coverage who were not from low-income households did not change. Thus, despite increased spending on public programs, the number of uninsured children was not reduced overall.8
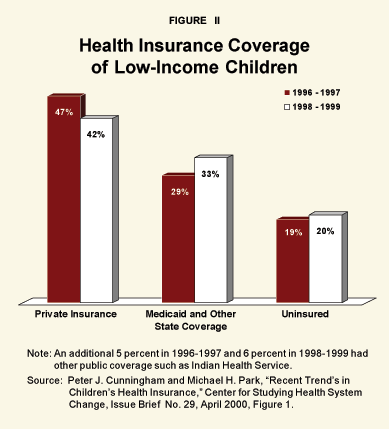
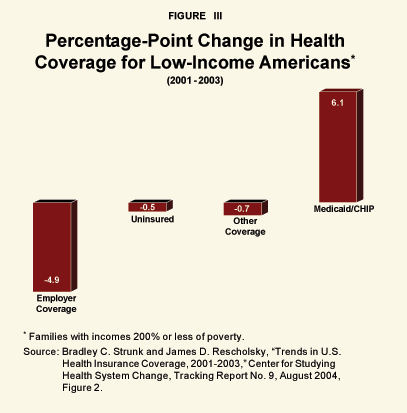
A casual look at Figure II suggests that in the latter 1990s the crowd-out of private insurance due to the expansion of public programs was close to one to one. More recent data suggests a similar conclusion for the current decade. From 2001 to 2003, the proportion of low-income Americans enrolled in public programs rose by 6.1 percentage points. However, this increase was offset by a 4.9 percentage point decline in coverage by employer-sponsored plans. Overall, the rate of uninsured fell only about one-half point.9 [See Figure III.] In this case, the data suggest that it takes a 13 percentage point increase in public coverage to reduce the uninsured rate by 1 percentage point.
“Despite a higher taxpayer burden, in the 1990s the percent of uninsured children did not go down.”
Kerry’s (i.e., Thorpe’s) estimates assume a 30 percent crowd-out.10 That is, for every 10 new Medicaid enrollees, three people lose private coverage. As a result, in order to insure 18 million new people (on net) through Medicaid expansion, Kerry would enroll about 26 million to make up for 8 million who lose private coverage. Kerry’s assumptions are much too optimistic, however. The evidence we have seen suggests the crowd-out rate will almost certainly be much higher, perhaps approaching 100 percent.
Bottom line: It is entirely possible that the Kerry plan could spend more than $500 billion and achieve no reduction whatsoever in the number of uninsured.
B. Problem: Failure to Enroll
Making people eligible for enrollment is not the same thing as actually enrolling them. Estimates vary, but anywhere from 10 to 14 million Americans who are eligible for free Medicaid and SCHIP health care are not enrolled.11 Kerry would extend this opportunity to enroll to millions more. To prod people into accepting coverage, he proposes automatically enrolling children in public schools or when they use community health centers. Past experience suggests this will not be easy. In fact, we can be fairly confident in predicting it will not succeed.
Why do 10 to 14 million Americans who are eligible for government funded health care not even bother to enroll? A possible answer is that they are getting free health care anyway.
A study by the Texas State Comptroller’s office found that Texas currently spends about $1,000 per year on free care for every uninsured person in the state, on the average.12 These estimates imply that the value of “free” care is about $4,000 per year for a family of four. Interestingly, $4,000 is a sum adequate to purchase private family coverage in many Texas cities. Granted, the two alternatives are not exactly comparable. But to many, the free care alternative appears more attractive than buying private insurance with aftertax dollars.
To our knowledge, no other state has duplicated the kind of intensive study done in Texas. However, an Urban Institute study estimated that uncompensated care to the uninsured nationwide totals about $800 per uninsured individual each year.13 If the value of uncompensated physician care were included, this total would probably rival the $1,000 Texas figure.
The existence of free care may make enrollment in Medicaid unnecessary. In fact an NCPA analysis of health regions in Texas found that where Medicaid spending was low, free care spending was high — and vice versa.14 Free care, in other words, appears to be a substitute for Medicaid.
How exactly does this substitution work? Despite a raft of studies claiming that being insured affects access to health care, there often is no difference in services rendered to those who seek care. Take Parkland Hospital in Dallas, for example. Both uninsured and Medicaid patients enter the same emergency room door, see the same doctors and receive the same care. The hospital rooms are the same, the beds are the same, and the care is the same. As a result, patients have no reason to fill out the lengthy forms and answer the intrusive questions that Medicaid enrollment requires. The doctors and nurses who treat these patients are paid the same, regardless of patients’ enrollment in an insurance plan. So they tend to be indifferent about who is insured by whom. In fact, the only people concerned about who is enrolled or not enrolled in what plan are hospital administrators, worried about who will pay the bills.
At Children’s Medical Center, next door to Parkland, a similar exercise takes place. Medicaid, SCHIP and uninsured children all enter the same emergency room door; they all see the same doctors and receive the same care.
“More recently, the net uninsured rate fell only onehalf percentage point.”
Interestingly, at both institutions, paid staffers make a heroic effort to enroll people in public programs — even as they wait for their medical care. Yet they apparently fail to enroll eligible patients more than half the time! After patients are admitted, staffers valiantly go from room to room to continue this bureaucratic exercise. But even among those in hospital beds, the failure to enroll rate is significant.
As an aside, we might ask why anyone should care whether people enroll or do not enroll in Medicaid or SCHIP. In Dallas County, thousands go to hospital emergency rooms to obtain free health care. But the same thing is true in Toronto and London. The difference is that in Toronto and London the patients are said to be “insured” and the fact that the care is “free” is a source of great national pride. In our country, the patients, who are probably getting better care than they would in Toronto or London,15 are said to be “uninsured” and the fact that they are getting free care is often a source of great national embarrassment.
Problem: Quality of Care. Although it may come as a surprise to many readers, Medicaid (for the poor) now spends more than Medicare (for the elderly and the disabled). The amount equals about $1,000 for every man, woman and child in the country every year. Sen. Kerry calls for a vast expansion of this program and he freely admits that the expansion will shift many from private to public insurance. But is this a good thing for patients?
Medicaid has always experienced problems finding physicians and providers willing to participate in the program.16 Compared to the privately insured, Medicaid patients have fewer choices of physicians, fewer choices of facilities, and are more likely to experience rationing by waiting. This may, in part, explain why pregnant women covered by Medicaid tend to enroll late, enter prenatal care late (often in their second or third trimester) and receive fewer prenatal visits than privately insured women.17
Part of the problem is the Medicaid patients’ relationship to Medicaid is very different from a privately insured’s relationship with a commercial insurer. Indeed, Medicaid is far more likely to respond to the pressures of special interests than to the needs of patients. For example:18
- In Dallas, Medicaid pays some hospitals 50 percent more than other hospitals for the same services; statewide, such practices lead to the waste of hundreds of millions of dollars.
- In Ohio, Medicaid’s method of cost-plus reimbursement pays for 13,000 empty nursing home beds.
- In El Paso, Medicaid over-compensates hospitals and under-compensates primary care, which is desperately needed by the city’s predominantly young, Hispanic population. As a result, clinics have to send patients to hospitals for x-rays and simple blood tests.
Moreover, when state government budgets get squeezed, politicians tend to cut enrollment (“optional” populations) and whole categories of treatment (“optional” services, such as drugs) rather than cut waste. These economy measures are virtually unheard of among employer-provided plans.
Precisely because the enrollees are not the real clients of Medicaid, the program is scandal-prone. Virtually every state has experienced exposés, but a Chicago Tribune investigation a decade ago was particularly revealing:19
- Over a nine month period, one woman saw 52 doctors — obtaining 2,000 Prozac antidepressant capsules.
- A man was diagnosed with 53 different medical problems from 79 different doctors; the 260 office visits he made cost Medicaid $51,764.
- In the course of 156 visits to 33 doctors, another woman obtained almost 6,000 doses of a codeine-based pain-killer, the tranquilizer Librium, and the sleeping aid Halcion.
- In one 12 month period, a 40-year-old patient saw 58 different physicians for a total of nearly 250 office visits.
- In one year, one patient obtained 9,218 Zantac pills.
Apparently, things have not much improved. A recent General Accounting Office report finds widespread fraud and abuse in every state.20
[page]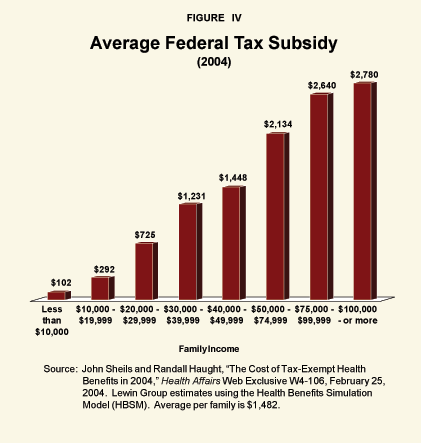
In the current system, government subsidies for private health insurance are already arbitrary and unfair. Rather than attempt to correct this problem, however, Sen. Kerry is proposing a raft of new subsidies that would be even more arbitrary and more unfair.
A. The Current System.
"Current system: Tax subsidies equal almost half the cost of employer-provided insurance for middle-income families."
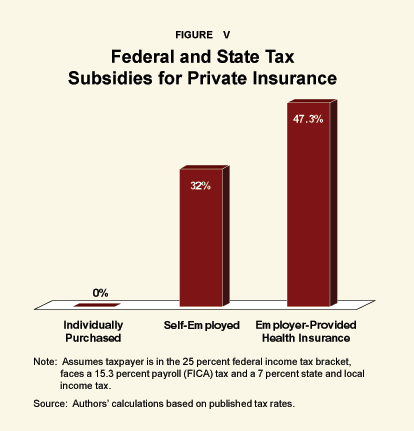
Federal and state government tax subsidies for health insurance – mainly employer-provided insurance — currently total about $190 billion per year. However, most of the assistance goes to those who need it least. Although the average tax subsidy is worth about $1,482 per family, households earning more than $100,000 per year receive $2,780 per year, on the average. By contrast, those earning between $20,000 and $30,000 receive only $725.21 [See Figure IV.] One reason is that those earning higher incomes are in higher tax brackets. For example, a family in the 40 percent tax bracket potentially gets a subsidy of 40 cents for every dollar spent on their health insurance. By contrast, a family in the 15 percent bracket potentially gets a subsidy of only 15 cents.
Another inequity arises because different people get different amounts of tax relief, depending on how they acquire health insurance. For example, when employers pay health insurance premiums rather than taxable wages, this fringe benefit escapes income and payroll taxes. Figure V shows what this means for a typical middle-income family. With employer provided coverage, the family gets a tax subsidy equal to almost half the cost of insurance. By contrast, middle-income families who purchase their own insurance get virtually no relief under the tax law.22 [See Figure V.]
B. Making the Current System More Arbitrary and Unfair.
Rather than create a fairer system that treats equals equally, Kerry would create dozens of new subsidies, making the system even more arbitrary. Among the artificial distinctions are the following
"Kerry plan: A worker in a 49-person firm could receive four times the subsidy as one in a 50-person firm."
Size of Business. Sen. Kerry proposes a generous subsidy for firms with fewer than 50 employees if they contribute at least 50 percent of premium costs, agree to cover all employees and purchase insurance through the managed competition system.23 The employer would receive a 50 percent refundable tax credit for the first 50 percent he contributes and a 25 percent credit against any additional contribution. The employer would receive the full credit for poverty level workers ($9,310 for an individual; $12,490 for a family of two). The credit then phases out gradually and is exhausted at 300 percent of the poverty level ($27,930 for an individual or $37,470 for a family of two). However, since the subsidy would be unavailable to employers of 50 or more, employees with identical incomes are treated very unequally. For example, consider an employee of a 50 person firm who pays no income tax, but whose wages are subject to a 15 percent (FICA) payroll tax:
- On the employer-paid share of premiums (assume 50 percent), this worker and his employer enjoy a 15 percent tax subsidy (because premiums are excluded from taxes) both under the Kerry plan and under the current system.
- However, if this same worker works for a 49 person firm, Kerry’s refundable tax credit (worth 50 percent) would bring the total tax subsidy up to 65 percent.
- The tax subsidy available at the latter firm is four times the size of the subsidy at the former one.
Age. Individuals aged 55 to 64 years who do not qualify for Medicaid and whose employers do not offer health insurance could buy coverage from the managed competition system. Those earning up to 300 percent of the federal poverty level would receive a 25 percent refundable tax credit to do so.24 However, this subsidy — available at age 55 — is not available to a 54-year-old with the same income.
Place of Work. The current system makes different tax subsidies available to different workers. Kerry’s plan would not only continue the practice, but make it much worse. For example:
- Individuals who buy into the managed competition system on their own would pay a subsidized premium — capped at 6 percent of their income at the poverty level and gradually increased to 12 percent of income at 300 percent of poverty; individuals with employer-provided insurance do not get to pay these rates.
- The self employed could deduct their premiums (as under the current system); other individuals, such as employees of firms that do not offer coverage, could not.
- Low-income unemployed workers would get a 75 percent subsidy, compared to 25 percent for those ages 55 to 64, 50 percent for employees of small firms and none for employees of larger firms.
No Horizontal Equity. As a result of the above, people at the same income level would receive vastly different subsidies, depending on their age, how they obtain insurance and where they work. This violates the well-known public finance principle of horizontal equity: People with the same incomes should be treated equally.
No Vertical Equity. Most of the subsidies in the Kerry plan are targeted toward lower-income workers and families. However, the catastrophic insurance subsidy — which is more than one third of the total — has the opposite distributional effect.25 Higher income workers tend to be enrolled in more lavish employer plans, which would receive more of this subsidy. More than two-thirds of the subsidy would go to firms with 500 or more employees. These large employers are more likely than small firms to have generous benefits and higher than average pay. They pay workers an average of $22.04 ($32.54 per hour with fringe benefits), and spend $2.34 per hour on health benefits. By contrast, only about 12 percent of the subsidy is targeted to small firms employing fewer than 100 workers. These firms pay lower wages ($14.46 per hour; $19.47 including fringe benefits), are less apt to offer health coverage, and spend less when they do ($1.13 per hour).26
These inequities extend to specific occupations. For example:
- Nonmilitary government employees earn an average of $20.13 per hour and under the Kerry plan their employers would receive $550.55 in health subsidies per worker per year.
- In the construction and mining industries, by contrast, the average hourly wage is somewhat less, at $17.60; but these employers would receive only $127.20 per worker per year.
- The average wage is much lower in farming, fishing and forestry, $9.71 per hour, but employers in those fields would receive only $68.45 per worker.27
“Each newly insured Medicaid enrollee could cost as much as $8,623 or more.”
One way to evaluate government subsidies is to ask: What do taxpayers get in return? The Kerry reforms claim to reduce the number of uninsured; and one can certainly argue that taxpayers have an interest in that goal, since they often pay the cost of health care for the uninsured. But what can the taxpayers expect in return for the extra burdens Kerry is asking them to bear?
A. Medicaid Expansion.
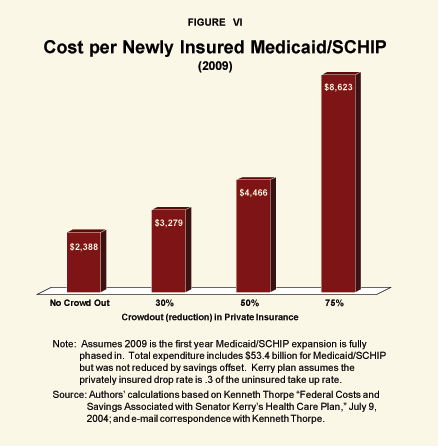
As noted above, the expansion of Medicaid and SCHIP in the 1990s significantly increased taxpayer burdens. But because private insurance contracted as public insurance expanded, little was accomplished. The conclusion: Medicaid expansion and SCHIP expansion are very inefficient ways of insuring the uninsured. Yet Kerry would extend that inefficient approach — in spades. As Figure VI shows:
- If Medicaid expansion induces a 30 percent contraction of private insurance (as Kerry assumes), the cost of insuring each new person, on net, will increase by more than one-third.
- At a more realistic 50 percent crowd-out rate, the cost almost doubles – reaching $4,466 per newly insured person or $17,864 for a family of four.
- At a 75 percent crowd-out rate, the cost of each newly insured person reaches $8,623, or $34,492 for a family of four.
- And at a plausible one-to-one crowd-out rate, there will be no reduction in the number of uninsured in return for a huge increase in government spending.
B. Private Insurance Subsidies.
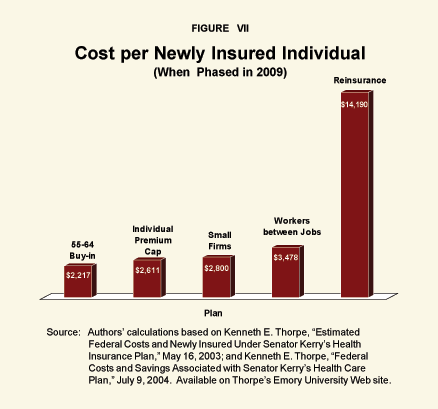
Most of the private insurance subsidies would go to employer plans rather than to individuals. Even Kerry estimates that most of the spending will be on people who are already insured. As Figure VII shows, by Kerry's own estimates:
- By 2009, when the plan is fully phased in, small business subsidies will cost $2,800 per newly insured person, or $11,200 for a family of four.
- Subsidies for workers between jobs will cost $3,478 per newly insured person, or $13,912 for a family of four.
- Catastrophic insurance subsidies will cost a whopping $14,190 for each newly insured person, or $56,760 for a family of four!
“Subsidizing employers’ high health care bills is a costly way to insure more people.”
Large as these numbers are, they likely err on the low side. Employers of workers who earn less than 300 percent of poverty will typically find it in their self-interest to drop employer-provided insurance once their employees have the opportunity to buy health insurance through the system of managed competition at artificially low premiums. Consider, for example, a family of four with an income equal to 200 percent of poverty, obtaining insurance from a small business:
- Kerry would offer this family a small business subsidy of $2,013 if they have insurance that costs about the average ($8,051) purchased by federal employers.
- Assume the employer drops the coverage and pays higher wages instead and that family is able to buy the same insurance individually, subject to a premium cap; the family's subsidy now rises to $3,770 — a good deal, even if the (FICA) payroll tax is applied to the higher wages.
Of course, many of the families who lose their employer coverage will pocket the extra income and forego the individual insurance, especially if no family member has a serious health problem. And those who do purchase individual insurance through the managed competition system will have an incentive to choose the highest-priced plans, rather than average-priced ones, because the premium cap will allow them to do so at no extra cost. (See the discussion on “Incentives to Spend More” below.)
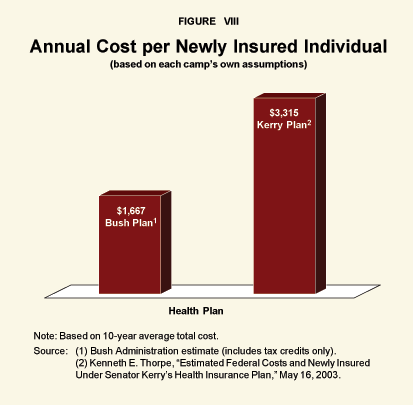
C. Kerry vs. Bush.
In an earlier publication, we compared the Kerry and Bush health plans based on assumptions made by each camp about its own plan. As Figure VIII shows, the Kerry plan costs more than twice as much as the Bush plan, per newly insured person.28 The reason why the Bush plan was so much more efficient (although insuring far fewer people) was that the Bush refundable tax credit was targeted to people who most need assistance.
“The Bush plan costs less per newly insured because its subsidies are targeted.”
In his State of the Union message, however, President Bush proposed a new tax relief plan: an above the line deduction for people who purchase Health Savings Account plans on their own. This subsidy is not as efficient because it will be claimed by many people who are already insured. Bush had three objectives in making this proposal, however: (1) increase the number of people who have insurance, (2) create tax fairness and (3) encourage efficient health insurance choices.
“The Bush plan would equalize tax subsidies between employer coverage and individually purchased plans.”
As noted above, under the current system people who purchase their own insurance get virtually no tax relief, even though people who obtain insurance through an employer are generously subsidized. An exception is a tax deduction that became available in 2004 for deposits to Health Savings Accounts. The Bush proposal would give the same tax relief to premium payments for HSA plans. This would create a level playing field on which people could choose between self-insurance (through HSA deposits) and third party insurance (HSA plan premium) without the distortions of tax law. In addition, the proposal offers comparable tax relief to people who purchase their own insurance and to those who receive employer-provided health insurance.
Professor Thorpe has produced estimates of the Bush package as a whole and concluded that the cost per newly insured person is the same for both Bush and Kerry. But that comparison is misleading, because it ignores the fact that Bush achieves two other goals – tax fairness and unbiased subsidies – whereas Kerry achieves neither of them.
D. Ignoring the Middle Class.
Strangely, the one group that Kerry completely ignores is the most discriminated against under the current system and would most likely respond to a tax subsidy: middle-income families who earn more than 300 percent of the poverty level. Indeed, once the Kerry plan is implemented, middle-class families who do not get insurance through an employer are the ones most likely to be uninsured!
It is widely thought that the uninsured are almost always low income families. Over the past decade, however, virtually all the growth in the uninsured has been among families who make more than $50,000 a year. By contrast, the uninsured rate among families who earn less than $25,000 actually declined.29
In general, families who earn $50,000 a year or more get up to a 50 percent tax subsidy if they obtain insurance through an employer. Yet they get virtually no tax relief if they purchase insurance on their own. Other than provide an opportunity to buy into the system of managed competition (with government subsidized catastrophic insurance), Kerry’s health care plan does little to assist this group – even though they are the ones most likely to bear a disproportionate tax burden to fund it.
[page]The costs of the Kerry plan will surely be greater than what Thorpe estimates. The reason: The plan would encourage people to over-consume health care. At the same time, Kerry seems to have rejected all forms of managed care and appears to be indifferent to cost controls through Health Savings Accounts and other consumer directed health care.
A. Perverse Incentives.
Numerous features of the Kerry plan would encourage people to overinsure and overspend on health insurance and health care.
“The Kerry plan would subsidize wasteful health care spending.”
Open-Ended Subsidies. Kerry’s plan would continue the current, deeply flawed system of open-ended tax subsidies. That is, the more employers and employees spend on health care, the greater subsidy they receive. People can always lower their taxes by spending more. This approach contrasts with the Bush administration's proposed fixed-sum tax credit, which subsidizes the core insurance we want people to have but leaves them free to purchase additional insurance with their own aftertax dollars. For example, the administration has proposed a $1,000 tax credit for individuals and a $3,000 credit for families. Once the $3,000 limit is reached, however, additional expenses would be paid with unsubsidized dollars.
Income Cap Subsidies. The theory behind managed competition is that people should be able to choose among a wide array of health plans – from somewhat Spartan to very rich.30 The government (or employer) subsidy, however, should be limited to an amount that covers the cost of basic insurance, with individuals paying for the bells and whistles out of their own pockets. Kerry’s income-based premium caps violate this principle. Once the cap is reached, the individual's incentive is to choose the richest, most expensive plan available, since someone else will be paying 100 percent of the extra cost.
For example, someone at the poverty level, buying into the managed competition system, would pay no more than $600 in premiums — even though the average cost of a family policy in the current Federal Employees Health Benefits Program (FEHBP) is $8,051. Once this individual decides to obtain insurance, there is no reason to settle for a moderately priced plan — especially when there are plans available in the $14,657 price range. Why choose a Hyundai, when you can have an Aston Martin at no extra cost?31
The irony is that the lowest income families under this system are likely to end up in the most lavish health plans – with much of the cost paid for by middle-income families who cannot afford to enroll in those very same plans!
Subsidies for Low-Income Individuals and Families. In addition to the premium caps, other subsidies for low-income families will change incentives and encourage perverse behavior. For example:
- The 75 percent subsidy for workers between jobs encourages people to purchase insurance until the value to them is only 25 cents on the dollar.
- The subsidy for low-income employees of small business will encourage people to obtain insurance until it is worth less than 50 cents on the dollar.32
- The 25 percent subsidy for people age 55 to 64 will encourage insurance that is worth 75 cents on the dollar.
Catastrophic Insurance Subsidies. The proposal to subsidize catastrophic insurance by paying for 75 percent of all medical expenses in excess of $50,000 also distorts incentives. Employees are likely to choose aggressive, unproven therapies, and mostly at taxpayers’ expense. As Helen Darling, president of the National Business Group on Health, said in a recent Wall Street Journal interview, such a scheme shows a “blank check mentality,” because once the $50,000 limit has been met, there will be weak incentives for anyone (employers, patients, insurers) to pay attention to costs.33 As a result, many more unnecessary procedures will be performed.
“Kerry appears to reject standard methods of controlling costs.”
For example, in the United States each year, doctors perform more than 500,000 heart bypass surgeries and another million angioplasties.34 Depending on the extent of the surgery, each procedure can cost well in excess of $50,000.35 Some experts believe that many of these operations provide no real benefit and may even put patients at unnecessary risk.36 Shifting most of their cost to taxpayers will not encourage employers and employees to make sure they are getting value for the money spent.
Though only a small percentage of insured workers use more than $50,000 worth of medical care in a given year, if government begins to pick up three-fourths of the tab, medical bills in this range will become more common.
B. Opposition to Cost Control.
Currently there are two broad ways of controlling health care costs: (1) managed care and (2) consumer directed care. Kerry appears to reject them both. In his ideal world, no one would choose between health care and other uses of money.
Opposition to Managed Care. Thorpe’s technical description implies that employers and insurers would have to engage in “case management” as a condition for receiving the new tax subsidies. However, in his acceptance speech at the Democratic Convention, Kerry said, “You’ll get to pick your own doctor — and patients and doctors, not insurance company bureaucrats, will make medical decisions.”37 This appears to be a blanket rejection of all forms of managed care.
Opposition to Consumer Directed Care. If employers and insurers cannot choose between health care and other uses of money, what about individuals? We assume Kerry opposes that, too; but we could be wrong. Kerry’s staff has indicated opposition to Health Savings Accounts, but we are not aware of any public statement by the Senator on this topic.
[page]Kerry’s plan to create an FEHBP-type system for individuals is supposed to reduce the number of uninsured by almost 6.7 million. Yet depending on how it is structured, it could cause the number of uninsured to increase. The reason: Many employers may simply drop coverage for their workers knowing that they can buy into the managed competition system. Workers facing premiums on their own without the tax exclusion granted to employer plans may opt to do nothing until they need care. In addition, if the system is structured like the federal program, people would be able to enroll annually at community-rated premiums. This means that people could avoid paying premiums while they are healthy and enroll only after they get sick. If healthy people respond to these incentives in predictable ways, the number of uninsured will rise, not fall.
[page]“The cost of government health care programs are consistently underestimated.”
Thorpe initially estimated Kerry’s plan’s cost at $895 billion over nine years.38 Subsequently, he revised his spending estimate upward to $951.8 billion, but came up with $298.8 billion in anticipated “savings,” leaving the nine-year cost at $653 billion39 — a figure less than the value of Bush tax cuts Kerry hopes to repeal for the highest income taxpayers. Are these numbers realistic? As noted in the Introduction, we believe Kerry has underestimated the spending and overestimated the savings.
A. Underestimating the Cost.
Since the introduction of Medicare and Medicaid almost 40 years ago, policy analysts have consistently underestimated the costs of new health care programs — usually by wide margins.40 Take Medicare, for example. In the first year, the program’s budget was 50 percent higher than predicted. By the sixth year, costs were running nearly 90 percent ahead of forecasts. Does Kerry’s plan suffer from the same tendency to underestimate?
The reason for these inaccurate projections has been the failure to appreciate the tendency of people to increase their use of health care when out-of-pocket costs are negligible. If price is no object, we could easily spend the entire gross domestic product on health care.41 Yet for 26 million enrollees in Medicaid and SCHIP (8 million of whom will come from private plans with such features as deductibles and copayments) price will suddenly become no object under the Kerry plan. Moreover, 10 million additional newly insured people will have new incentives to spend simply because they now have private health insurance. And we have seen how the many new subsidies under the Kerry plan will give people new incentives to overinsure and overconsume.
Another factor pushing up costs is a predicted new round of health care inflation. As discussed below, $100 billion a year in new government spending, coupled with additional private spending, will force up health care prices for everyone – causing more government spending through such programs as Medicare and Medicaid and lower tax revenues, as nontaxable health benefits crowd out taxable wages at the work place.
B. Expected Reduction in Uncompensated Care.
Sen. Kerry plans to save money by reducing federal Disproportionate Share Hospital (DSH) payments for treating indigent patients. Currently, the government makes payments through Medicaid to those hospitals that serve a disproportionate share of charity care patients. But if the number of the uninsured is reduced, one would expect the cost of uncompensated indigent care to fall as well, as should the federal government's share of the burden. Even if the number of uninsured low-income families diminishes, however, we expect fierce political resistance to a reduction in DSH payments.
“Kerry proposes illusory savings.”
Unfortunately, that is where any savings will likely end. Yet in addition to fewer DSH payments, Sen. Kerry also hopes to save through aggressive use of disease management, by investing in information technology, and by rolling back payments to Medicare+Choice private plans. Let’s briefly look at each of these proposals.
C. Disease Management and Information Technology.
Kerry hopes to save $116.5 billion over 10 years by employing disease management techniques and information technology. There is little doubt that, in principle, health care could be provided more efficiently, and that information technology seems promising. But Kerry’s approach lacks the appropriate incentives. The economic principle that applies here is: He who does the economizing must be the one who gains from the economization. The Kerry approach reverses that principle. It expects doctors, nurses, hospital personnel and insurers to realize economies so that taxpayers can save money. The question is: Why should they?
Appropriate disease management and increasing use of information technology are likely to be adopted, whether or not we implement the Kerry plan. It is doubtful that any additional savings to the federal government will be realized by putting more people in Medicaid and by encouraging managed competition. An additional problem, noted above, is that the projected savings from disease management seem to be negated by Sen. Kerry’s Democratic convention promise to avoid all forms of managed care.
D. Reduction of Payments to Private Medicare Plans.
The Kerry plan’s final cost-reduction proposal (an estimated $14.4 billion savings over nine years) would eliminate the recently legislated increase in payments to Medicare+Choice insurers, who provide seniors with health insurance coverage similar to what nonseniors have.
Of all Kerry’s cost savings schemes, this one is most unfair. And it may not save any money, since without the coverage for drugs and other services that private insurers provide, low income seniors may turn to more expensive Medicaid and Medicare services.
Studies show that seniors who enroll in Medicare+Choice plans tend to be those who have low incomes and who previously lacked Medicare supplemental (medigap) insurance. Thus, without a private plan, these seniors would be most vulnerable to the cost of expenses not paid by Medicare, including prescription drugs.
Kenneth Thorpe admits that seniors in private plans receive about $1,000 worth of benefits over and above those promised by Medicare, including coverage for drugs.42 Without the private plans, these seniors would likely turn to more expensive hospital and doctor therapies, ultimately paid for by taxpayers. As a result, making Medicare+Choice plans available to Medicare enrollees probably reduces overall government spending.
Precisely for these reasons, Congress increased payments to Medicare+Choice plans in the Medicare reform bill passed last year. Prior to passage, private plans were abandoning the market because the compensation was too low. Congress sought to reverse that trend and encourage more such plans to enter the market. This desirable reform, well worth the money it costs, is what Kerry wants to eliminate.
[page]“Kerry’s health care model is based on Hillary Clinton’s 1993 plan.”
43As we have seen, the Kerry plan calls for an enormous expansion of government-run health care programs. For those who remain in the private sector, most will participate in a nationwide system of managed competition, modeled after the Federal Employees Health Benefit Program (FEHBP). In fact, Ken Thorpe predicts that 75 percent of all employers will buy into the FEHBP-type system.
The idea of modeling the nation’s health care system on that available to federal employees is not new. Stanford University Professor Alain Enthoven made the proposal almost 25 years ago44 and Hillary Clinton adopted it as the basis for her health care reform plan a decade ago.45
Currently, federal employees choose among a dozen or more competing health plans each year.46 However, the competition among these insurers is not the same as one would find in a free market. It takes place under artificial rules that seriously distort the incentives of buyers and sellers in the health insurance marketplace.
A. Managed Competition
Health insurance plans in the FEHBP do compete. But the competition is artificially constrained. Each health plan is required to charge the same premium to every applicant (community rating) and to accept all applicants regardless of health conditions (guaranteed issue). An 80-year-old retiree pays the same premium to join a health plan as a 20-year-old employee.47 As a result, insurers do not compete on their ability to price and manage risk. Instead, they must compete on their ability to provide health care and manage its cost. This is not really competition among firms in the business of insurance. Rather, it is competition in the delivery of health care.
This artificial market changes the nature of the product both for buyers and sellers. Buyers are not purchasing protection against the loss of their assets when they select one of these health plans. The system as a whole provides protection against costs due to an expensive illness. Instead, when federal workers select a health plan they are choosing a set of particular health care services, such as access to one doctor network rather than another. This is comparable to requiring consumers to choose a specific auto insurer so they can have their cars repaired at particular auto repair shops; or to choose a specific homeowners’ insurer so they can get hail damage repair from a particular roofer.
“Managed competition creates perverse incentives to undertreat the sick and overtreat the healthy.”
The benefits of competition are easy to understand. These benefits flow principally from the fact that insurance companies find it in their self-interest to compete for the trade of potential customers. Thus, they make buyer-pleasing adjustments in their competitive strategies. However, none of the valuable benefits of competition will emerge if sellers find it in their self-interest not to sell to some buyers and if in fact, they compete with each other to avoid such customers. Yet managed competition creates these perverse incentives. People who know they need expensive medical treatment will use this knowledge to select a health plan. And since insurers understand this, they structure their products to discourage enrollment by the most expensive customers.
How Perverse Incentives Affect the Behavior of Buyers. Imagine a system in which health plans offer particular doctor and hospital networks in return for fixed premiums. People who are seriously ill and need specific, expensive medical treatment will select very differently from other people. Take a heart patient in need of cardiovascular surgery. This individual wants to find the best cardiologist and the best heart clinic. Therefore, this patient will look for the health plan that has a contract with that cardiologist and clinic. The premium matters little, since the value of receiving the best cardiovascular care far exceeds the patient’s premium payment.
The incentives facing healthy people are different. Because they are less likely to need any particular service in the near future, they are unlikely to spend much time investigating particular doctors and clinics. To the degree that they do investigate, they will probably inquire only about the primary care services they expect to receive. And if the need for heart surgery arises, odds are that patients will be able to switch insurers before the surgery is performed.
Thus the people who carefully compare the acute care services offered by competing health plans are likely to be the people who intend to use them. These are the very people health plans want to avoid. By contrast, those who choose a plan based on the quality and accessibility of nonacute services are more likely to be healthy.
How Perverse Incentives Affect the Behavior of Sellers. Imagine two competing HMOs. In the first, enrollees can see a primary care physician at any time, but there are cumbersome screening mechanisms and waiting periods for kidney dialysis, heart surgery and other expensive procedures. In the second, dialysis and heart surgery are available when needed, but primary care facilities are limited. Given a choice, most of us would enroll in the first HMO if we were healthy and switch to the second if afflicted with heart disease or kidney failure. But if everyone acted in this way, the second HMO would attract only expensive-to-treat patients. To cover its costs, it would have to charge a premium many times higher than the first HMO. The premium would need to approximate the cost of heart surgery or a kidney transplant. But most people can't afford that premium. Those who could afford it might be better off to simply buy their medical care directly. In any event, the HMO would face financial ruin.48
“Health plans will try to avoid the sick.”
It might seem that the second HMO could compete successfully by offering more primary care services. But to be truly competitive, it would have to change its strategy completely. The easiest way to keep costs down is to enroll only the healthy. And the easiest way to do that is not to have the doctors and facilities sick people want. As Alain Enthoven has noted (disapprovingly), “A good way to avoid enrolling diabetics is to have no endocrinologists on staff…. A good way to avoid cancer patients is to have a poor oncology department.”49
To attract healthy enrollees, a health plan might offer inexpensive vaccinations, cancer screening and a health club membership. The plan also might offer services at convenient times and locations, and provide free parking and other amenities. Of course, these services might be attractive to all potential applicants, but they are more likely to be decisive for healthy people. Health plans also can attract the healthy by targeting their advertising to desirable demographics.
A survey by the Kaiser Family Foundation discovered how HMOs competed for seniors on Medicare. The HMO print and television ads showed seniors snorkeling, biking and swimming, but did not feature the sick or disabled. In addition, nearly one-third of HMO marketing seminars were held at sites that were not wheelchair accessible.50 The following are just a few other examples of competition under managed competition uncovered by the Washington Post:51
- When a Minnesota network offered direct access to an obstetrician while rivals required referrals from a gatekeeper, it attracted disproportionate numbers of pregnant women, lost millions of dollars and soon ended the practice.
- When Aetna U.S. Healthcare offered unusually generous coverage for in vitro fertilization, people with fertility problems flocked to the HMO and Aetna had to end the practice.
- In another case, a California health plan severed its relationship with a university hospital known for practicing high-tech medicine and tackling complicated cases.
- Other HMOs avoid contracting with doctors’ groups known for expertise with high-risk patients.
The term “medlining” is sometimes used to describe the practice of avoiding the sick. It is health care’s version of redlining — the banking and insurance practice of avoiding deteriorating neighborhoods. The other side of the coin, of course, is attracting the healthy. In addition to health club memberships, some health plans have also offered dental benefits and vision care. The theory is that anyone who will switch health plans to get a free pair of eyeglasses cannot be very sick.52
B. The Results of Competition
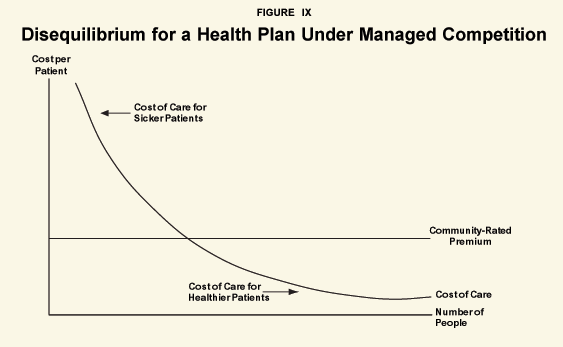
“Community-rated premiums don’t cover the cost of caring for the sickest patients.”
In Figure IX, patients are arrayed along the horizontal axis from most to least costly (left to right). The cost-of-care line shows what would be spent on each patient, given current standards of medical practice. This line is highly skewed, reflecting the fact that in a typical pool about 2 percent of the group spends more than 40 percent of the health care dollars, 10 percent spends almost three-quarters and the majority have very small expenses. The premium (selected by the health plan) is based on the average cost of care for all patients under community rating. This is the premium that must be charged all plan members if the plan is to cover its costs.53 The figure also illustrates how healthy people subsidize sick people, since most members have costs well below the premium they pay and a few have costs well above it. Clearly, this is what many proponents of managed competition believe the situation would look like for each health plan under their scheme. But a simple analysis shows that the diagram in Figure IX will give way to something else.
Roughly speaking, an equilibrium in a market exists if no health plan can adjust to become more profitable.54 However, the plan represented in Figure IX can easily become more profitable if it can lower the cost of caring for its sicker members. As long as these members stay in the plan, it will have the same premium income and lower costs. If sicker members shift to another plan, this is even better — since by definition, the sick are unprofitable. On the other hand, healthier customers are overcharged, since their cost of care is below the premium they are paying. This means that other health plans can lure away these customers by providing higher benefits for the same premium. Thus in order to retain profitable customers and attract even more, the health plan represented in Figure IX should increase the amount it spends on healthy members.
“Health plans will try to enroll healthy, low-cost enrollees.”
In free markets, competition causes prices to change until they equal average cost. The same tendencies exist under artificial competition. Yet because community rating requires the same premiums for all members, competition will cause cost to change until it equals price. If premiums could rise for “unprofitable” members, health plans would compete them up to the level of the cost of those people’s care. But if the premiums are artificially constrained, the plans will compete the cost of care down to the level of the artificial premium.55 The reverse pressures exist for “profitable” members. If the artificial premiums cannot be competed down to the level of average cost, the tendency will be to compete cost up to the level of the artificial premium. These conclusions follow from well-known principles of the economics of regulation. In the United States, we have had decades of experience with regulated markets. For most of the post-World War II period, the federal government has established minimum air fares higher than would have prevailed in a free market. Unable to compete on price, airlines have competed by offering more frequent flights, more convenient departures, more spacious seating and other inflight amenities. The reverse tendency emerges when prices are kept artificially low. For example, rent control laws prohibit landlords from raising their rents to the level of average cost. Since rents cannot rise, landlords tend to allow housing quality to deteriorate until housing costs equal the government-controlled rent.56
Consider this result in terms of a basic economic theory: When firms are maximizing profits, marginal revenue must equal marginal cost. Under artificial competition, marginal revenue (the amount of premium each additional enrollee pays) must be the same for every enrollee. Thus if health plans are maximizing profits, marginal cost (the amount the plan spends on each additional enrollee) must also be the same for every enrollee.
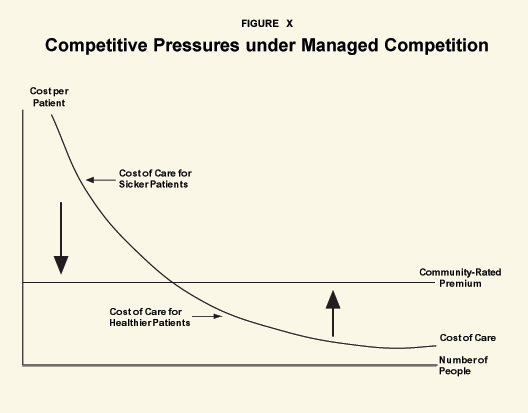
Health plans, therefore, face competitive pressures to adjust the delivery of health care until the cost-of-care line coincides with the (community-rated) premium line. [See Figure X.] This means that health plans have a strong financial self-interest in underproviding services to the sick and overproviding services to the healthy. Left unchecked, the end result of this process is a condition under which each person receives health services whose cost is exactly equal to the premium he or she pays.
C. The Effect of Limited Open Seasons
“The quality of care will fall for the sickest enrollees.”
The analysis presented here assumes that patients make choices among insurers based solely on the value of medical services they consume. This assumption would be justified to the degree that patients can easily shift back and forth among insurers as their health needs change. However, the federal employee program and most other managed competition programs allow plan changes only during “open season” once a year.
To the degree that people’s choices are constrained by limited open seasons, they must consider the insurance value of the plan they select as well as its direct consumption value. Consider an expectant mother choosing among competing health plans. She will need well-baby delivery services. However, she might experience complications in pregnancy or childbirth, or her child might be premature and require sophisticated medical treatment. In those cases, the woman would benefit from highly skilled medical personnel. Thus, she will be interested in purchasing real insurance as well as specific medical services.
For such potential problems as heart disease, cancer and AIDS, healthy people will be less likely to insure for expensive treatment — if they can switch insurers at least every 12 months. The tendency is to select a plan that is strong on preventive and diagnostic services, confident that one can eventually switch to a plan that is best at treating a particular disease should the need arise.
Therefore, periodic open seasons cause us to modify our prediction in recognition of an insurance component to people’s choices. Yet even with this modification we are left with the prediction that artificial competition will ultimately result in a radical deterioration in the quality of care sick people receive.
D. Barriers to Quality Deterioration
Just because health plans have an economic incentive to let treatment costs fall until they are no greater than the premium payments made on behalf of the sickest patients does not mean they will do so. Fear of tort liability lawsuits is one obstacle to quality deterioration. Doctors’ fear of censure or loss of a license to practice is another. But these obstacles are somewhat crude instruments for combating incentives that affect the decisions providers make.
E. Actual Experience of the FEHBP: Why Isn't It Worse?
Much of the behavior of the buyers and sellers within the FEHBP system is consistent with the theory of managed competition outlined here. But actual experience is nowhere near as bad as what theory would predict. Why not?
There are four apparent reasons.
“If the federal employees’ health system were extended to the whole population, the results would be much worse.”
Insurers and Providers Are a Small Part of a Large Private Market. In general, the doctors, hospital personnel and other providers who serve federal government employees are practicing in a very large private marketplace. Federal employees are a small fraction of their overall caseload. Similarly, the insurers for federal employees also compete in a much larger private marketplace. Undoubtedly, the practices and techniques that are the norm for the private market tend to shape and influence behavior within the FEHBP.
Put another way, managed competition within the FEHBP is a small subset of a much broader market where managed competition is absent. Behavior in the smaller market tends to reflect behavior in the larger one. But if it were the other way around — with managed competition being dominant and nonmanaged competition having a much smaller presence — we would expect the incentives of managed competition to exert a much greater impact on the practice of medicine.
There Is Very Little Movement of Enrollees among Plans. Despite the attractive idea that federal employees exercise choices among a dozen or so plans every year, the reality is that people tend to enroll in a plan and stay there. In fact, only about 5 percent of enrollees actually switch plans when they have the opportunity to do so.57 With so little movement among plans, the system is far less competitive in practice than it appears to be in theory. The absence of vigorous competition undoubtedly ameliorates the harmful effects of the perverse incentives we have examined. However, efforts to encourage competition and choice would almost certainly put more pressure on the health plans to respond to the perverse incentives they face.
The Office of Personnel Management Actively Discourages Perverse Competitive Behavior. To most advocates of managed competition, the office of Personnel Management (OPM) impassively sets the rules of the game and allows the competitors to compete at will. In fact, OPM is a much more aggressive regulator. All plans and changes in plan design have to be approved by OPM and the agency uses this power to make the market far less competitive than it otherwise would be. What OPM does for a limited number of federal employees, however, is unlikely to be duplicated by an overseer of an insurance market that includes most of the people in the country.
No Alternative Market Exists. Federal employees essentially get health insurance through their employer, the federal government. They have few opportunities to go outside the FEHBP and buy insurance in another market. As noted above, employer premium payments escape income and payroll taxes. But if federal employees purchased health insurance on their own, they would have to do so with their own, aftertax dollars. The fact that federal employees are a captive market with no alternative market to turn to is another factor ameliorating competitive pressures within the FEHBP. Those pressures would certainly be much stronger (and their perverse outcomes more evident) if people could move in and out of a FEHBP system in the manner envisioned under Sen. Kerry’s health plan.
F. Kerry vs. the FEHBP.
“Under Kerry’s managed competition, there will be fewer plans and higher costs.”
In campaign speeches and campaign literature, Sen. Kerry has implied that ordinary citizens will be able to join the health system used by federal employees. These statements have shocked and alarmed many federal workers, however. They envision hordes of expensive uninsurables swamping the federal system and pushing up costs.58 Anticipating this reaction, Kerry's team proposed a system that is essentially an FEHBP look-alike. The insurers who offer plans in the FEHBP will offer those same plans in the look-alike system. Same plans, same rules of competition, but formally separate systems.
Fewer Plans. How does Sen. Kerry know all the plans that participate in the FEHBP will choose to participate in the new look-alike? Many FEHBP plans are worker specific, such as the postal workers plan and the Panama Canal employees Plan.59 One could require FEHBP insurers to participate in the look-alike system. But since this might cause some plans to leave both systems, federal employees would surely resist this idea.
Higher Costs. Even if the same plans were available in both systems, the premiums charged could not be the same for two reasons. First, adverse selection guarantees the look-alike pool will be sicker and more costly to insure. As noted above, healthy people will be able to leave this pool for low cost alternatives (at least initially), an option not available (or practical) for federal workers. Second, the look-alike system will be far more vulnerable to cost-increasing special interest mandates. (See the discussion below). The look-alike FEHBP system therefore will be more costly than the real FEHBP and this cost difference will grow through time.
G. Kerry vs. National Health Insurance.
Unlike the left wing of the Democratic party, Kerry rejects the idea of National Health Insurance. Yet because the managed competition system he proposes includes so many perverse incentives, we could experience the same drawbacks prevalent in the government-run health care schemes of other countries.
“British National Health limits access to new technology.”
The most serious defect of national health insurance is the tendency to overprovide to the healthy and underprovide to the sick. This occurs because of the pressures inherent in allocating health care resources through the political system. Politicians cannot afford to spend most of the health care budget on the small number who need expensive care. Democratic politics forces them to take from the sick and give to the healthy instead. Take Britain, for example. Compared to health care in United States, the British National Health Service (NHS) is notorious for limiting access to modern medical technology:60
- The per capita use of renal dialysis for kidney failure in the United States is more than three times that of Britain.
- Britain has less than one-half as many CT scanners per capita as the United States and only one-half as many MRI scanners.
- According to the World Health Organization (WHO), as many as 25,000 people in Britain die of cancer each year because they cannot obtain the latest cancer drugs.
Yet while the NHS routinely skimps on services for the seriously ill, it overprovides to patients with minor ailments. For example:
- There are more than 18 million ambulance rides in Britain every year, or about one ride for every three people in the country; 80 percent of the rides are for such nonemergency purposes as outpatient care and pharmacy visits and amount to little more than free taxi service.
- The NHS provides free day care services to more than 260,000, home care or home help services to 578,000, home alterations for 375,000 and occupational therapy for 300,000.
“The Kerry plan would produce similar results, for different reasons.”
The British preference for “caring” over “curing” is a direct result of the political nature of national health insurance. In a typical U.S. private health care plan, 40 percent of health care dollars are spent on the sickest 2 percent of the population. In a government run system, politicians cannot afford to spend 40 percent of the budget on 2 percent of the voters, many of whom are probably too sick to vote anyway. The temptation is always to take from the few who are sick and spend instead on the many.
Managed competition, as we have seen, creates similar incentives. Whereas national health insurance overprovides to the healthy and underprovides to the sick for political reasons, managed competition encourages this same outcome because of perverse economic incentives.
[page]What are the likely effects of a huge expansion of Medicaid and the opportunity for employers and individuals to join a system of managed competition? We make four predictions.
A. Demise of the Small Group Market
One likely effect is that the market for small group insurance will vanish. The reason: The FEHBP-type market will enjoy an across-the-board subsidy for catastrophic costs and a subsidy for low-income employees that ranges from 25 percent to 37.5 percent of premiums (depending on the employer’s contribution) with lower, but still substantial, contributions for moderate-income employees. In addition, the FEHBP-type market will promise premium stability – small employers won’t face huge premium increases just because one employee has an expensive illness.
“The individual and small group markets would largely disappear.”
Since participation is voluntary, there may be an opportunity for small groups to stay in the commercial market (paying lower premiums) when all the employees are healthy and enter the FEHBP-type pool when health status takes a turn for the worse. It is this exodus of the healthy that undermines most health marts and other voluntary purchasing arrangements. In this case, however, employers will face a 10 percent penalty if they leave and reenter the FEHBP-type pool in addition to the tax subsidies that favor participation. Small group insurers should not count on a robust market for their products.
B. Demise of the Individual Market
Similar considerations apply to the market for individual and family policies. The self employed, people between jobs, older workers — all would be attracted to Medicaid or to the system of managed competition. For instance, according to eHealthInsurance.com, 46 percent of enrollees in HSA plans have family incomes of less than $50,000. The health insurance company Assurant has found that more than one-third (38 percent) of its HSA purchasers have only high school or technical school training. The same percentage lives in homes with market values less than $125,000. Twenty-seven percent have a net worth of less than $25,000.61 Under the Kerry plan, most of these families would qualify for free health care through Medicaid. Those whose income is too high would get special tax subsidies if they join the FEHBP-type system not available in the ordinary market.
C. Demise of Fee-For-Service Medicine
It is very difficult for fee-for-service insurers to compete under managed competition. The reason: People tend to prefer HMO coverage when they are healthy because they enjoy the low-out-of-pocket cost, and choice of doctors is not very important. However, once a serious health problem occurs, choice of physicians becomes more important — despite the higher out-of-pocket costs. Fee-for-service plans, therefore, tend to attract a disproportionate number of high cost enrollees. This is one reason so many fee-for-service insurers have left the FEHBP. Among those that remain, pure fee-for-service plans have been replaced by PPOs (Physician Provider Organizations) with some features of managed care.
D. Diminished Role for Employers
As noted above, employers of workers who earn less than 300 percent of a poverty-level income will generally find that both they and their employees will be better off if the employers drop employer-paid coverage and pay higher wages instead. The reason: The subsidies available to individuals who buy insurance through the managed competition system are more generous than the subsidies available through the workplace.
[page]The Kerry plan would harm the economy. Higher taxes on capital and labor will discourage savings, investment and work. High rates of health care inflation will strain government budgets, create pressures for higher taxes and lower the take home pay of workers. Inadequate revenues from Kerry’s tax plan, coupled with his promise to balance the budget, will force higher taxes on middle-income families.
A. Higher Marginal Tax Rates.
Kerry’s plan phases out most of his proposed subsides as individual incomes rise. This feature adds to the stiff work penalties that are already in the tax code.
Premium Caps. As discussed above, people who pay their own premiums to the FEHBP look-alike system will enjoy a limit on the amount of premiums they have to pay. For example, at a poverty level income, the premium will be no more than 6 percent of income. At 300 percent of poverty and above, the premium will be limited to 12 percent of income. This means that individual health costs go up as income rises. Specifically:
- An individual at the poverty level income ($9,310) will pay no more than $559 in premiums every year; but at 300 percent of poverty ($27,930) the maximum premium rises to $3,352.
- A family of four at the poverty level ($18,850) will pay only $1,131; but at 300 percent ($56,550) the maximum premium rises to $6,786.
“Phasing out subsidies as income rises raises marginal tax rates.”
The increase in the premium cap increases the penalty imposed on those who increase their earnings. For example, between a poverty level income and an income of 300 percent of poverty, the premium cap creates a 15 percent marginal tax rate, on top of other taxes and entitlement withdrawals. To put this in perspective, families in this income range already face effective marginal tax rates in excess of 50 percent due to income and payroll taxes and the withdrawal of the Earned Income Tax Credit (EITC) and other welfare entitlements!62 Once individuals reach 300 percent of income, their health costs rise by 12 cents for each $1 increase in income, assuming that the health plan they choose pushes them to the cap. This means that:
- An individual in the 25 percent tax bracket (say, due to a 15 percent FICA tax and a 10 percent income tax) will now face a 37 percent marginal tax rate.
- An individual in the 35 percent tax bracket (say, due to a 15 percent FICA tax, a 15 percent income tax and a 5 percent state income tax) will now face a marginal tax rate of 42 percent.
Ironically, Kerry’s attempt to help low-income families forces them to face marginal tax rates that are normally paid only by the very wealthy.
Withdrawal of Other Subsidies. The withdrawal of other Kerry subsidies also imposes marginal tax rates that are quite high. As Figure XI shows:
- The small employer tax credits can add nearly 11 percentage points to the marginal tax rates of low-income employees — assuming (as Kerry does) that employees reap all the benefits of these subsidies and bear all the cost of their withdrawal, even though an employer may be paying the entire premium.63
- However, if the employee chooses the highest-cost plan (a likely case if the premium is fully paid by the employer) the additional marginal tax rate will be 19 percent.64
- The withdrawal of the subsidy for workers between jobs creates an additional marginal tax rate between 16 percent and 29.2 percent, depending on the plan chosen.
- The subsidy for older workers increases marginal tax rates between 8.1 and 14.17 percent, depending on the plan chosen.
Medicaid Eligibility. Kerry would continue the current practice of making eligibility for Medicaid an all or nothing proposition. Due to arbitrary income cut offs in both the Kerry plan and the current system, individuals could face marginal tax rates far in excess of 100 percent. Consider an individual who earns 300 percent of poverty and is enrolled in Medicaid. If this person receives a salary increase of $1, he or she will lose family (Medicaid) health coverage worth from $5,000 to $10,000!
“Low income workers would face much higher marginal tax rates.”
Readers may wonder: What is the alternative? The alternative is to give people a subsidy that can be applied to Medicaid or to private insurance, with any shortfall being paid from the enrollee's own resources. The ideal subsidy is a lump sum, independent of income. Such a subsidy has no effect on marginal tax rates. If the subsidy must phase out as income rises, this can be done in a way that only modestly increases marginal tax rates. Bush's tax credit phase out, for example, raises marginal tax rates by only 5 percentage points.
B. Lower Take Home Pay.
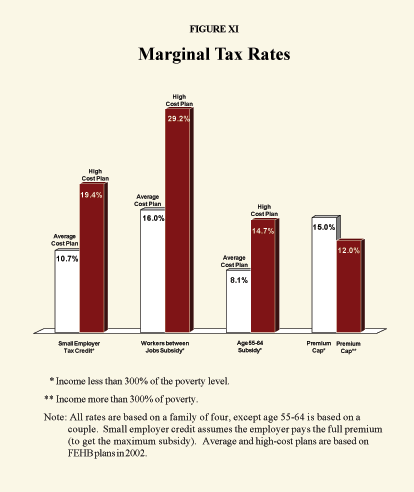
“To earn an extra dollar, workers would have to give up 15 cents of subsidy or more — on top of all other taxes.”
Employer-provided fringe benefits often substitute for wages. Other things being equal, an expansion of fringe benefits lowers after-tax wages more than they otherwise would be.
To a certain extent, we want people to substitute health insurance for wages, because there is a social interest in whether people are insured. The uninsured, as we have seen, are often able to get free care (paid by taxpayers). The current system's problem is not that government encourages people to have health insurance, but rather, that it distorts the choice between health insurance and other uses of money at the margin.65 By making the tax subsidies for health insurance open-ended, we have created a situation in which people can always lower their taxes by purchasing more health insurance. Kerry's proposal accepts this defect and makes it much worse.
A far better approach would be to give people a tax credit for the core insurance that we want everyone to enjoy and let them buy extra insurance with (unsubsidized) aftertax dollars.
C. Medical Inflation.
“Medical inflation will increase.”
Prior to the advent of Medicare and Medicaid in 1965, health care spending never exceeded 6 percent of gross domestic product. Today it exceeds 14 percent. These two government programs unleashed a torrent of new spending. But because demand increased without a corresponding increase in supply, the new spending led to higher prices rather than more health care. The federal government estimates that each additional $1 of health care spending yields only 43 cents worth of additional care, and the other 57 cents buys higher prices.66
Just as health care prices began to rise with the influx of new government spending in the 1970s, Kerry's addition of $100 billion per year in federal health care subsidies will almost certainly fuel even higher health care prices. Moreover, when the 27 million newly insured obtain insurance, they will add both their employer’s and their own money to the pot, making the total amount of new spending several times the magnitude of the government's largesse. To make things worse, these myriad subsidies will encourage people to overinsure and overconsume health care.
D. Higher Taxes on Capital.
“Capital formation will be discouraged.”
As noted earlier, Kerry hopes to pay for much of the cost of his health plan by rescinding President Bush’s tax cuts for people earning more than $200,000 a year. Although there has been much rhetoric about how the “rich” have benefited from the Bush tax cuts, they have received only a modest reduction in their tax bracket from 39.6 percent to 35 percent — a proportionately smaller reduction than the drop from 15 percent to 10 percent for those at the other end of the income spectrum. For those highly-paid rock stars and professional athletes who spend everything they make, that was the only tax cut they got. The more significant reductions in the capital gains tax rate and the dividends tax rate are only available to people who save, rather than consume. Moreover, these tax cuts are accomplishing three important goals.
First, they send a message to the rich, as well as everyone else, that saving will be rewarded. If a rock star saves and invests (instead of consuming), her tax rate on any subsequent income will be 15 percent instead of 35 percent. This gives all taxpayers an incentive to put money back into the economy — where the primary beneficiaries will be workers who will have more job options, higher productivity and more pay.
Second, lower rates on capital gains and dividends lower the cost of capital to all U.S. business concerns. Lower capital costs encourage further investment and job expansion. This also helps U.S. companies to compete in the international marketplace.
Third, the tax changes favored by the Bush administration place debt and equity financing on a more level playing field. Under the previous tax regime, interest payments made by companies were deductible, but dividend payments were not. Because of this, the tax law favored debt over equity. It also encouraged firms to retain and re-invest earnings — even if their investment prospects were not as good as their shareholders. Thanks to Bush’s tax changes, investment decisions can be made on the basis of economics, not tax law. Similarly, the choice between debt and equity finance is now more likely to be made on the basis of market considerations rather than tax considerations.
Kerry proposes to undo all of this. By repealing Bush’s tax cuts, he would raise the cost of capital for all U.S. companies, and return us to the days when corporate debt structure and investment decisions reflect the tax law, rather than economics.
E. Higher Taxes for the Middle Class.
“Repealing tax cuts on the rich won’t pay for Kerry’s plan.”
Kerry has pledged to pay for his health plan by repealing the Bush tax cuts for those who earn $200,000 a year or more. Reversing Bush’s intent to make these tax cuts permanent, Kerry anticipates an extra $800 billion in new revenue over 10 years. However, Bush’s intent is not the status quo. These tax cuts are scheduled to expire anyway. Against the budget that Kerry has promised to balance, immediate repeal of the tax cuts raises only $300 billion — less than one-third of what he really needs.67 Higher taxes on the middle-class seem to be inevitable consequence of the Kerry plan. Indeed, most of the financing would probably come from the middle-class.
[page]With respect to political considerations, there are two important questions to be asked:
- Is Kerry’s plan likely to be adopted?
- If it is adopted, how is it likely to evolve?
Let us consider both these questions in brief.
A. Political Resistance.
Congressional passage of Kerry’s plan, at least as currently proposed, would be very difficult – unless Kerry’s election were seen as a national mandate for the Kerry health plan. The easiest part to pass is the expansion of Medicaid and SCHIP, because this would give financial relief to state and local governments. But this idea may be opposed by some Democrats in Congress. A much harder reform will be the imposition of managed competition nationwide. Harder still will be the vast and expensive system of employer subsidies.
B. Hidden Subsidies.
One could argue that the business of politics is the activity of imposing costs on some for the benefit of others. But of all the transfers politicians are asked to make, the least popular idea is to impose taxes on one group in order to subsidize another group. The reason: The people who are going to experience pain will know its source precisely, whereas the people who are going to benefit may not even be aware of their benefits, let alone know the source.
Kerry’s proposal to cover three-fourths of the cost of catastrophic illness is very expensive. It accounts for more than a fourth of the cost of his entire health plan. When subsidies to small business are included, employer subsidies make up more than one-third of the cost of the plan. Note: These subsidies go directly to the employers and/or their insurers. There will be no line item on any worker’s pay stub. Indeed, employees are likely to be completely unaware of the subsidy.
Economic theory teaches that the benefits of such subsidies will eventually devolve to the employees. But if this plan were proposed by a Republican, the benefits would be characterized as “trickle down.” They are precisely the type of benefits that politicians don’t like.
“Politicians like to get credit for visible subsidies, not hidden ones.”
A similar principle applies to the politics of medicine in other countries. The biggest problem with government-run health care systems worldwide is the temptation to skimp on expensive technology. In principle, everyone benefits from an MRI scanner because everyone is a potential beneficiary. But if people do not understand the benefit (because it is subtle and not obvious) politicians do not get much credit for buying the equipment and maintaining it. That is why the temptation is to forego the scanner and spend the money on services that touch lots of people in obvious ways — even if it does little to improve their health.
Against these considerations is the hope of Kerry advisors to get support from a business community that is clearly concerned about rising health care costs. But this support may be tepid or nonexistent for reasons given below.
C. Managed vs. Nonmanaged Competition.
As noted above, a likely consequence of the Kerry health care plan is the virtual disappearance of the individual and small group markets. Commercial insurance for larger companies will also likely disappear. Obviously, most insurance companies and the agents who sell their products would oppose such changes. Also, all the insurers who have left the FEHBP or never participated in the first place will oppose the plan. There is a reason why they are not selling their products to government employees.
Against this opposition, who can be counted on to favor the change? Even insurers who currently participate in the FEHBP may not like the Kerry plan. The reason: uncertainty about how they will fare in a new, untried system.
D. Distributional Effects.
“The Kerry approach is trickle down — most of the checks will be written to someone other than the person expected to benefit.”
Roughly three-fourths of the cost of the entire Kerry plan is designed to benefit (either directly or by trickle down) lower income households. In this sense, it is consistent with traditional Democratic ideology. But Democratic politicians in recent years have been moving in a different direction — competing for middle class votes by promising middle-class benefits, often paid for by low-income families. For example, tobacco taxes, lotteries and other forms of gambling are popular with Democratic politicians almost everywhere. Yet these are among the most regressive ways to raise revenue. The proceeds from these taxes on the poor often fund middle-class benefits, such as education or tax cuts.
E. The Slippery Slope.
If the Kerry plan is adopted, a slippery slope will likely emerge. Problems at each stage will to lead to a new stage. Ultimately we will likely evolve the way the German system has: with mandated benefits, mandated participation, managed competition and a small “private” sector that will cater to the few who can afford it.
Mandated Benefits. Once the federal government gets involved, special interests will soon follow. Currently, health insurance is a state issue. As a result, the sea of special interest activity that surrounds health insurance regulation resides primarily at the state level. But if Kerry succeeds in making health insurance a federal concern, all the problems of state regulation will elevate to the federal level.
“Voluntary participation will likely evolve into employer mandates.”
For example, mandated health insurance benefits are laws requiring insurers to cover specific providers and procedures not usually included in basic health care plans. In 1965 there were only seven state-mandated benefits nationwide. Today there are close to 1,500.
Mandates cover services ranging from acupuncture to in vitro fertilization, and providers ranging from chiropractors to naturopathy. They cover bone marrow transplants in Georgia, hairpieces in Minnesota, marriage counseling in Connecticut and pastoral counseling in Maine. These laws mean that if people buy insurance at all, they must purchase a bloated and expensive package of benefits designed by politicians. They are forbidden to buy insurance that reflects their own preferences, tailored to individual and family needs.
Mandated benefits raise the cost of insurance and make it considerably more expensive than barebones insurance. As a result, mandates price otherwise healthy people out of the market. In fact, studies estimate that as many as one out of every four uninsured Americans has been priced out of the market for health insurance by mandates.68
Mandated Employer Participation. As special interest legislation (as well as adverse selection) forces up the cost of the FEHBP look-alike plans, employers with healthier work forces may leave the system — or choose not to join in the first place. As noted earlier, there have been numerous attempts to set up systems of managed competition for employers, including health marts and purchasing pools. These arrangements inevitably fail because firms leave the pools (for cheaper insurance) when their employees are healthy and join the pools when their employees are sick (because alternative insurance is more expensive). One way to prevent this instability, perhaps the only way, is to require employers to participate.
Mandated Employee Coverage. The problem of instability caused by employer behavior also applies to individuals. People who buy their own insurance, as well as people who obtain insurance through an employer, are tempted to remain uninsured (and save on premiums) while healthy and enroll only after a serious illness has occurred (when the expected health care is worth more than the premium). The more expensive insurance becomes (again, because of mandates and adverse selection), the more likely people will engage in such behavior and the more unstable the insurance pool will become. As in the case of employers, a solution – again, perhaps the only solution — is to require individual participation.
Mandated Employer Funding. In a Kerry administration, employers will likely be required to cover all employees and to pay almost all the cost of that coverage. This stage of evolution is almost unavoidable for two reasons. First, politicians around the world are very reluctant to try to force individual voters to buy anything. And they certainly never do so if mandating employer payments is an alternative. Second, for reasons discussed above, the Kerry plan will cost much more than he projects, and in the face of such budget pressures the inevitable temptation will be to shift costs to employers. Employers, therefore, will find that they are required to enroll their employees and pay for the cost of health insurance that they have absolutely no control over.
[page]Ultimately, full implementation of the Kerry plan will lead to massive changes in our health care system. At the end of the process we will find a four-tiered health care system.
Tier one will be the Medicaid/SCHIP tier. Families will have limited choice of doctors, lengthy waits and rationing of care, much as we see in Medicaid today. Over time, as health costs rise and budget pressures mount, they will see more rationing of care. Today’s enrollees are all poor; millions of middle-class families will be added.
Tier two will look increasingly like the German system, which has had mandated employer coverage for about 90 percent of the population for many years and has recently introduced American-style managed competition. Pressures to hold down costs will lead to increased waiting times and less access to expensive medical technology — but not as bad as for Medicaid patients. The government may engage in nationwide negotiations with providers and impose limits on high tech equipment, as is done in Germany.69 The pressures of managed competition will induce health plans to overprovide to the healthy and underprovide to the sick, which happens in Britain and Canada.
"As in Germany, the elite who can afford it will choose to opt out."
Tier three will consist of a small percent of the population (in Germany it’s about 10 percent) who can afford to opt out of the more general system of managed competition. They will pay more for their health insurance and they will pay higher doctors’ fees. They will experience less rationing by waiting and easier access to expensive technology, and they will probably receive better health care.
Tier four will consist of seniors who will remain in Medicare. The Bush presidency promised to give seniors access to the same full-service health plans as the rest of America. Under a Kerry presidency that hope would almost certainly evaporate. Cost pressures would induce the government to squeeze providers (as happens under the current system), leading to longer waits and more rationing – but not as bad as for Medicaid patients because seniors will continue to have more political power.
Overview. In the past, providers were able to shift some costs – from those who underpaid to those who overpaid. For example, inadequate payments from Medicaid and Medicare were made up by overcharging employers and private insurers. Regardless of who becomes the next president, competitive pressures in the provider community will intensify. Cost-shifting will become increasingly rare.
Under a Kerry presidency people will ultimately get the kind of care they and their insurers pay for. No more; no less.
NOTE: Nothing written here should be construed as necessarily reflecting the views of the National Center for Policy Analysis or as an attempt to aid or hinder the passage of any bill before Congress.
[page]- Kenneth E. Thorpe, “Estimated Federal Costs and Newly Insured Under Senator Kerry’s Health Insurance Plan, May 16, 2003; and Kenneth E. Thorpe, “Estimated Costs and Savings Associated with Senator Kerry’s Health Care Plan,” July 9, 2004. (Unpublished documents; available on Thorpe’s Emory University Web site.) Although Thorpe has no official relationship with the Kerry campaign, he is generally credited as the author of Sen. Kerry’s health plan.
- Thorpe, “Estimated Costs and Savings Associated with Senator Kerry’s Health Care Plan.”
- Thorpe’s projection is included in Appendix A. The assumptions behind the cost estimates as well as Kerry’s plan to pay for the program are discussed more fully below.
- Thorpe, “Estimated Federal Costs and Newly Insured Under Senator Kerry’s Health Insurance Plan” and Thorpe “Estimated Costs and Savings Associated with Senator Kerry’s Health Care Plan.”
- However, the loss of private insurance is likely to cause a small, offsetting increase in government revenues as employers substitute taxable wages for previously untaxed health benefits.
- David M. Cutler and Jonathan Gruber, “Does Public Insurance Crowd Out Private Insurance?” Quarterly Journal of Economics, Vol. 111, No. 2, May 1996, pp. 391-430.
- Private coverage (both employer and individual) fell a total of 5 percentage points; public coverage rose 5 percentage points; and the uninsured rose 1 percentage point. Coverage rates of the non-poor stayed the same. See Peter J. Cunningham and Michael H. Park, “Recent Trends in Children’s Health Insurance: No Gains for Low-Income Children,” Center for Studying Health System Change, Issue Brief No. 29, April 2000.
- Devon M. Herrick, “Five Myths about the Uninsured in America,” National Center for Policy Analysis, Brief Analysis No. 339, September 20, 2000.
- Bradley C. Strunk and James D. Rescholsky, “Trends in U.S. Health Insurance Coverage, 2001-2003,” Center for Studying Health System Change, Tracking Report No. 9, August 2004.
- E-mail correspondence from Kenneth Thorpe to Devon Herrick, July 28, 2004.
- Estimates of eligibility for public health care programs vary. The lower estimates are that around 10 million Americans are eligible but unenrolled, while the upper range of estimates is closer to 14 million. One study found that just over half (51.4 percent) of eligible, nonelderly adults were enrolled in Medicaid in 1997. Of the remaining adults who were Medicaid eligible, 21.6 percent had private coverage while 27 percent were uninsured. Another study found that about seven million uninsured children eligible for either SCHIP or Medicaid are not enrolled. See Amy Davidoff, Bowen Garrett and Alshadye Yemane, “Medicaid-Eligible Adults Who Are Not Enrolled: Who Are They and Do They Get the Care They Need?” Urban Institute, Series A, No. A-48, October 2001. Of those children eligible for Medicaid or SCHIP, one-third are eligible for SCHIP while two-thirds are eligible for Medicaid. Eight percent of uninsured, low-income children are illegal aliens and, as such, not eligible for either Medicaid or SCHIP. See Lisa Dubay, Jennifer Haley and Genevieve Kenney, “Children’s Eligibility for Medicaid and SCHIP: A View from 2000,” Urban Institute, Series B, No. B-41, March 2002. Also see “The Uninsured in America,” Blue Cross Blue Shield Association, February 27, 2003.
- Texas Comptroller of Public Accounts, “ Texas Estimated Health Care Spending on the Uninsured,” State of Texas, December 1999.
- Jack Hadley and John Holahan, “How Much Medical Care Do The Uninsured Use, And Who Pays For It?” Health Affairs, Web Exclusive W3-66, February 12, 2003.
- See John C. Goodman, “Minority Report of the Texas Blue Ribbon Task Force on the Uninsured,” in Sen. Chris Harris (Chairman) and the Members of the Texas Blue Ribbon Task Force on the Uninsured, “Texas Blue Ribbon Task Force on The Uninsured,” Report to the 77th Legislature, State of Texas, February 2001, p. 42.
- At Parkland Hospital, for example, a patient with a migraine might get an MRI scan, whereas this would almost never happen at public hospitals in Toronto or London. For more on the differences in health care systems, see John C. Goodman, Gerald L. Musgrave and Devon M Herrick, Lives at Risk: Single-Payer National Health Insurance Around the World (Lanham, Md.: Rowman & Littlefield, 2004), forthcoming.
- Sara Rosenbaum, “Medicaid,” New England Journal of Medicine, Vol. 346, No. 8, February 21, 2002, pp. 635-640.
- See E. Kathleen Adams, Norma I. Gavin, Arden Handler, Will Manning and Cheryl Raskind-Hood, “Transition in Insurance Coverage from before Pregnancy through Delivery in Nine States, 1996-1999,” Health Affairs, Vol. 20, No. 1, January/February 2003, pp. 219-229.
- Michael Bond, John C. Goodman, Ronald Lindsey and Richard Teske, “Reforming Medicaid,” National Center for Policy Analysis, NCPA Policy Report No. 257, February 2003.
- Bonita Brodt, Maurice Possley and Tim Jones, “How Hustlers Milk Medicaid,” part 4 of a series on “Medicaid: System in Chaos,” Chicago Tribune, November 3, 1993.
- Government Accountability Office, “Medicaid Program Integrity: State and Federal Efforts to Detect and Prevent Improper Payments,” July 9, 2004, GAO-04-707, p. 7.
- John Sheils and Randall Haught, “The Cost of Tax-Exempt Health Benefits in 2004,” Health Affairs, Web Exclusive W4-106, February 25, 2004.
- John C. Goodman, “Characteristics of an Ideal Health Care System,” National Center for Policy Analysis, NCPA Policy Report No. 242, April 2001.
- Thorpe, “Estimated Costs and Savings Associated with Senator Kerry’s Health Care Plan.”
- The federal poverty guidelines are available at “2004 HHS Poverty Guidelines,” Federal Register, Vol. 69, No. 30, February 13, 2004, pp. 7336-7338.
- Thorpe, “The Impact of Sen. John Kerry’s Health Care Proposal on Health Care Costs,” June 2004. Also see Sarah Lueck, “Businesses Are Wary of Kerry Health Plan,” Wall Street Journal, July 26, 2004.
- Authors’ analysis of Thorpe, “The Impact of Sen. John Kerry’s Health Care Proposal on Health Care Costs,” June 2004, Table 1; and Bureau of Labor Statistics, “Employer Costs for Employee Compensation-March 2004,” Bureau of Labor Statistics, U.S. Department of Commerce, USDL: 04-1105, June 24, 2004, Table 8.
- Authors’ analysis of Thorpe, “The Impact of Sen. John Kerry’s Health Care Proposal on Health Care Costs,” June 2004, Table 1; and Bureau of Labor Statistics, “Employer Costs for Employee Compensation-March 2004,” Bureau of Labor Statistics, U.S. Department of Commerce, USDL: 04-1105, June 24, 2004.
- Devon M. Herrick, “Bush versus Kerry on Health Care,” National Center for Policy Analysis, Brief Analysis No. 468, March 18, 2004.
- Devon M. Herrick, “Uninsured by Choice: Update,” National Center For Policy Analysis, Brief Analysis No. 460, October 7, 2003.
- See Alain C. Enthoven, “The History and Principles of Managed Competition,” Health Affairs, Vol. 12, (Supplement) 1993, pp. 24-48.
- In 2002, the average cost of family coverage in the FEHBP was $8,051.16. However, for some temporary employees, a FFS Plan with PBP (Health Plan-High) could cost as much as $14,656,98. See FEHB 2002, 2002 Plan Comparison, FFS Plan Profile: PBP Health Plan-High. Available Online at: http://www.opm.gov/insure/02/html/standard/plancomparison.html. Accessed August 10, 2004.
- If the employer pays 100 percent of the premium, the tax exclusion allows a poverty-level employee and his or her employer to avoid a 15 percent payroll (FICA) tax. On top of that, the government’s small-business subsidy for this worker would be 37.5 percent.
- Sarah Lueck, “Businesses are Wary of Kerry Health Plan,” Wall Street Journal, July 26, 2004.
- American Heart Association, “Heart Disease and Stroke Statistics – 2004 Update,” American Heart Association, Section 11.
- Mark A. Hlatky, et al., “Medical Care Costs and Quality of Life after Randomization to Coronary Angioplasty or Coronary Bypass Surgery,” New England Journal of Medicine, Vol. 336, No. 2, January 9, 1997, pp. 92-99.
- Howard H. Wayne, Living Longer With Heart Disease: The Noninvasive Approach That Will Save Your Life (Los Angeles, Calif.: Practice Mgt Information Corp, 1998).
- From John Kerry’s remarks as prepared for delivery to the Democratic National Convention. See Associated Press, “Text of Kerry’s Acceptance Speech,” MSNBC.com, July 29, 2004.
- Thorpe, “Estimated Federal Costs and Newly Insured Under Senator Kerry’s Health Insurance Plan.”
- Thorpe, “Estimated Costs and Savings Associated with Senator Kerry’s Health Plan.”
- John Merline, “Medicare’s Blown Projections,” Investor’s Business Daily, February 4, 1998.
- For a discussion of how medical spending could increase when medical care is free at the point of service or highly subsidized, see John C. Goodman, Gerald L. Musgrave and Devon M. Herrick, Lives at Risk: Single-Payer National Health Insurance Around the World (Rowman & Littlefield, 2004),Chapter 24, forthcoming.
- Kenneth E. Thorpe and Adam Atherly, “Reforming Medicare: Impacts on Federal Spending And Choice of Health Plans,” Spending & Plan Choice: Medicare Reform, Health Affairs Web Exclusive, October 10, 2001.
- This section is largely based on John C. Goodman and Gerald L. Musgrave, “A Primer on Managed Competition,” National Center for Policy Analysis, NCPA Policy Report No. 183, April 1994.
- The case for managed competition was forcefully argued in Alain Enthoven, Health Plan: The Only Practical Solution to the Soaring Cost of Medical Care (Reading, Mass.: AddisonWesley, 1980). For an update on Enthoven’s views on the advantages and disadvantages of the FEHBP, see Enthoven, “Effective Management of Competition in the FEHBP,” Health Affairs, Vol. 8, No. 3, Fall 1989, pp. 33-50.
- See Walter A. Zelman, “The Rationale behind the Clinton Health Care Reform Plan,” Health Affairs, Vol. 13, No. 1, Spring 1994, pp. 9-29.
- The Federal Employees Health Benefits Program (FEHBP) has four main features: 1) federal employees in most places can choose among 8 to 12 competing health insurance plans, including Blue Cross and a number of HMOs; 2) the government contributes a fixed amount that can be as much as 75 percent of each employee’s premium; 3) the extra cost of more expensive plans must be paid by the employee with aftertax dollars; and 4) the plans are forced to community rate, charging the same premium for every enrollee. A similar choice system is in place for employees of many state and local governments. Public employee health benefit options in the state of Minnesota are similarly organized, as is the California Public Employees’ Retirement System (CalPERS). See Bryan Dowd and Roger D. Feldman, “Employer Premium Contributions and Health Insurance Costs,” in Michael Morrisey, ed., Managed Care and Changing Health Care Markets (Washington, D.C.: American Enterprise Institute, 1998), pp. 24-54. Many private employers also give employees a choice of health plans, and where these plans are independent organizations they effectively compete against each other to enroll members. See James Maxwell et al., “Managed Competition in Practice: ‘Value Purchasing’ by Fourteen Employers,” Health Affairs, Vol. 17, No. 3, May/June 1998, pp. 216-27.
- Congress initially exempted itself and other government employees from Medicare coverage. The policy was changed for new employees in the early 1980s so that today 80 to 85 percent of federal employees have Medicare coverage — and Medicare is the payer of first resort.
- The HMO would receive premiums only from people who were about to undergo expensive medical procedures. Thus the average premium would have to equal the average cost of the procedures. It is precisely because most people cannot easily bear such a financial burden that health insurance is desirable in the first place.
- Alain Enthoven, “The History and Principles of Managed Competition,” Health Affairs, 1993 Supplement, p. 35. On the practice of encouraging high-cost patients to “disenroll,” see Jonathan E. Fielding and Thomas Rice, “Can Managed Competition Solve the Problems of Market Failure?” Health Affairs, 1993 Supplement, p. 222; and Joseph Newhouse, “Is Competition the Answer?” Journal of Health Economics, Vol. 1, No. 1, January 1982, pp. 109-16.
- Reported in Natalie Hopkinson, “Study Finds Medicare HMOs Target Active Seniors but Not Disabled in Ads,” Wall Street Journal, July 14, 1998.
- David Hilzenrath, “Showing the Sickest Patients the Door,” Washington Post, National Weekly Edition, February 2, 1998.
- Ibid.
- Note that the premium does not have to be the same for all plans, but it must be the same for all members of a given plan.
- More formally, an equilibrium is said to exist when no participant in the market — including all buyers and sellers — can improve his or her position by any unilateral move.
- Other analysts have recognized this problem, noting that the tendency is one of “the free market pitfalls of managed competition” (p. 118), that “one of managed competition’s greatest challenges is to safeguard quality of care without robbing the system of free-market efficiencies” (p. 110) and that “managed competition carries an inherent risk of discrimination against enrollees who incur high health care costs” (p. 120). See Alan L. Hillman, William R. Greer and Neil Goldfarb, “Safeguarding Quality in Managed Competition,” Health Affairs, 1993 Supplement, pp. 110-22.
- See William Tucker, The Excluded Americans: Homelessness and Housing Policies (Washington, D.C.: Regnery Gateway, 1990).
- Robert D. Reischauer (Brookings Institution), Testimony before the Senate Committee on Finance, May 21, 1997. Also see FedWeek.com, March 31, 2004, Section 9.
- Mike Causey, “Be Wary of Expanding Health Plan to Uninsured,” Washington Times, August 3, 2004 and Mike Causey, “Strangers in Your Health Plan?” Mike Causey’s Federal Report, FederalNewsRadio.com, July 28, 2004.
- “Guide to Federal Employees Health Benefits Plans For Federal Civilian Employees,” FEHB 2004 Guide, publication RI 70-1, Center for Retirement and Insurance Services, U.S. Office of Personnel Management, November 2003.
- Goodman, et al, Lives at Risk.
- Laura Trueman, “Health Savings Accounts: Myth vs. Fact,” National Center for Policy Analysis, Brief Analysis No. 479, July 19, 2004.
- Jagadeesh Gokhale, Laurence J. Kotlikoff and Alexi Sluchynsky, “Does It Pay to Work?” National Center For Policy Analysis, NCPA Policy Report No. 258, March 2003, and Jagadeesh Gokhale and Laurence J. Kotlikoff, “Does It Pay Both Spouses to Work?” National Center For Policy Analysis, NCPA Policy Report No. 260, May 14, 2003.
- This tax rate assumes that the employer pays 100 percent of health plan costs. Employer receives a 50 percent tax credit for first half of expenditure and a 25 percent credit for spending above half the cost for employee coverage. In 2002, the average cost of family coverage in the FEHBP was $8,051.16. Under the Kerry plan, using the 2004 poverty level, a family of four moving from 150 percent of poverty ($28,275) to 300 percent ($56,550) would lose approximately $3,020 in subsidies on an average policy.
- In 2002, the average cost of family coverage in the FEHBP was $8,051.16. However, some FFS family plans cost as much as $14,656.98 per year. See FEHB 2002, Plan Comparison, FFS Plan Profile: PBP Health Plan-High. Available Online at: http://www.opm.gov/insure/02/html/standard/plancomparison.html. Accessed August 10, 2004.
- John C. Goodman and Merrill Matthews, “Reforming the U.S. Health Care System,” National Center for Policy Analysis, Policy Backgrounder No. 149, April 26, 1999.
- The Health Care Financing Administration (now the Center for Medicare and Medicaid Services) estimated that between 1960 and 1988, 57 percent of the growth in personal health expenditures was due to price, 10 percent to population and 34 percent to the use of medical services and supplies. See National Center for Health Statistics, Health, United States,1990 (Hyattsville, Md.: Public Health Services, 1991), Table 106.
- See John D. McKinnon, “Kerry’s Deficit Cutting Math May Not Add Up,” Wall Street Journal, July 30, 2004.
- Gail A. Jensen and Michael A. Morrisey, “Mandated Benefit Laws and Employer-Sponsored Health Insurance,” Health Insurance Association of America, January 1999. This estimate is consistent with early estimates by John C. Goodman and Gerald L. Musgrave, “Freedom of Choice in Health Insurance,” National Center for Policy Analysis, NCPA Policy Report No. 134, November 1988.
- See Victor G. Rodwin, “Physician Payment Reform: Lessons from Abroad,” Health Affairs, Vol. 8, No. 4, winter 1989, pp. 76-83.
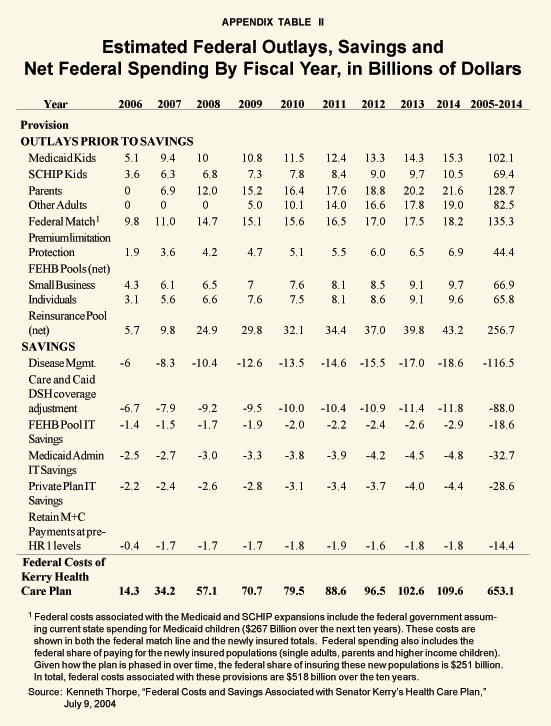
John C. Goodman, Ph.D., is the founder and president of the National Center for Policy Analysis. National Journal recently dubbed him the “Father of Health Savings Accounts,” and he has pioneered research in consumer-driven health care.
Dr. Goodman is the author of eight books, and is author/co-author of more than 50 published studies on health care policy and other topics. He received a Ph.D. in economics from Columbia University. He has taught and done research at several colleges and universities including Columbia University, Stanford University, Dartmouth University, Southern Methodist University and the University of Dallas.
Devon Herrick, Ph. D., a senior fellow with the National Center for Policy Analysis. He concentrates on such health care issues as Internet-based medicine, health insurance and the uninsured, and pharmaceutical drug issues. His research interests also include managed care, patient empowerment, medical privacy and technology-related issues.
Dr. Herrick received a Ph.D. in Political Economy and a Master of Public Affairs degree from the University of Texas at Dallas with a concentration in economic development. He also holds an MBA with a concentration in finance from Oklahoma City University and an MBA from Amber University, as well as a BS in accounting from the University of Central Oklahoma.