Medicaid, the joint federal-state health care program for the poor and near poor, is the largest single expenditure by state governments today. At the rate the program is growing, it is on a course to consume the entire budgets of state governments in just a few decades.
The Growth of Medicaid. Although Medicaid is commonly assumed to be a health program for welfare recipients, there are 10 times as many people on Medicaid as there are receiving welfare checks. Medicaid costs American taxpayers more than $1,000 per year for every man, woman and child in the country, or $4,000 a year for a family of four. Including Medicare and other public health care spending, the average family of four is spending more than $11,000 on other people’s health care – more than the cost of health insurance for such a family in almost all states.
The program has grown far beyond the scope originally envisioned. Nationally, Medicaid covers:
- One in every six people.
- One in every three children.
- One in every two births.
- More than one of every two nursing home residents.
What Difference Does Medicaid Make? It is commonly assumed that Medicaid enrollment is preferable to being uninsured, but little thought has been given to the actual effects of Medicaid on the people it serves.
- One study found that Medicaid’s strict eligibility requirements induce enrollees to consume more and save less, reducing their average household wealth by $1,600 to $2,000.
- Another study found that Medicaid expansions have been substantially offset by reductions in the number of people with private coverage, as people drop private health insurance to take advantage of “free” health insurance.
- A recent RAND Corporation study found that there was very little difference in the quality of health care received by Medicaid enrollees and uninsured individuals, once they saw a doctor.
Unequal State Spending. Medicaid programs consume more than one-fifth of the average state budget, more than the average state spends on public schools. However, spending per Medicaid enrollee varies widely. For example:
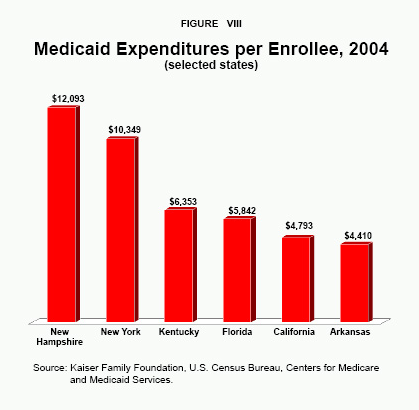
- New Hampshire spends about $12,093 per Medicaid enrollee, the most of any other state, compared to the nationwide average annual cost of about $6,834.
- In contrast, Arkansas spends only $4,410 per enrollee.
Higher living costs or health care costs do not explain this wide disparity in state spending.
Waste, Fraud and Abuse. Both high- and low-spending states waste funds in some obvious ways. For example:
- New York pays for millions of trips by ambulatory patients in specially-equipped vans when low-cost public transportation is available.
- Ohio pays for 12,000 empty nursing home beds each year.
- In Colorado, Michigan and many other states Medicaid has paid for services to beneficiaries who are no longer living, due to a lack of controls on provider reimbursements.
Some Medicaid abuse is fraud, but it is difficult to determine the extent in states that do not make aggressive efforts to discover it. Fraud and abuse may consume as much as $1 of every $10 nationwide, according to the Government Accountability Office, and more than $1 of every $5 in New York Medicaid, according to one estimate. A New York Times investigation found massive provider fraud in New York City, including a dentist who claimed to have performed nearly 1,000 procedures in a single day and 9,500 procedures in one month.
Costly State Policies. There are widespread practices that raise state Medicaid costs:
- Many states cover far more of the population than the poor and provide more generous benefits than the private sector, encouraging individuals to drop private health insurance.
- Many states underpay physicians and overpay hospitals, encouraging hospital-based treatment instead of less expensive care in doctors’ offices.
- Many states pay premium prices for brand-name drugs even though lower-cost generic and over-the-counter medications may be just as effective.
- Many states encourage nursing home care over lower-cost community-based care or home care.
- Many states also pay the long-term care expenses of middle- and upper-income seniors – but make little effort to recover costs from their estates or their children.
Common-Sense Reforms. There are a number of reforms states can implement without bureaucratic federal hassles. These include such common-sense changes as:
- Substituting less-expensive for more-expensive therapies and providers wherever possible;
- Selective contracting with hospitals and other health care facilities;
- Instituting pay-for-performance programs where possible, reimbursing providers based on outcomes, not services rendered.
- Expanding efforts to detect fraud and abuse to recapture inappropriate provider payments.
- Exploiting less expensive alternatives to nursing home care and recapturing the assets of deceased nursing home residents to defray the cost of their care.
Fundamental Reform: Consumer-Driven Health Care. America is on the leading-edge of a consumer-driven health care (CDHC) revolution that will transform private health insurance and care delivery. A number of states are undertaking initiatives that inject CDHC principles of competition, choice and control into Medicaid. Among the ways this can be done:
- Give patients control of some of the Medicaid dollars spent on their health care by establishing Health Opportunity Accounts that enrollees can use to pay for some health services, providing them financial incentives to consume health care wisely.
- Allow enrollees to enroll in employer-sponsored plans where they work using Medicaid funds to pay the employee’s share of premiums and/or allow them to purchase private health insurance directly.
- Create financial incentives for people to purchase long-term care insurance instead of relying on Medicaid.
The new Deficit Reduction Act gives states a wide range of options to reform their Medicaid programs, although in some cases states must still apply for waivers from the federal government.
More Radical Reform: Block Grants to the States. More fundamental reform will require federal legislative changes. One might assume that the federal contribution to state Medicaid programs is based on each state’s poverty population. Yet, this is not the case. For example:
- New York has 8 percent of the nation’s poverty population, but gets 12.9 percent of all federal Medicaid dollars.
- By contrast, Texas has 10.3 percent of the nation’s poor, but receives only 6 percent of federal Medicaid dollars.
Ideally, Congress should distribute federal funds in block grants based on each state’s poverty distribution and allow the states full discretion over their use, provided they are spent on indigent health care. The block grant could include federal Medicaid funds and State Children’s Health Insurance Programs (SCHIP), along with other federal health dollars.
States would have the flexibility to design their own systems, and would realize the full benefit of every dollar saved through more efficiently-delivered care and pay the full cost of every dollar of unwise spending.
[page]Medicaid is the largest single expenditure by state governments today. Health care costs have risen rapidly over the past decade, and the states as a whole now spend more on Medicaid than they spend on primary and secondary education.1 Medicaid and other health expenses account for one in every five dollars of state spending.2 At the rate the program is growing, it is on a course to consume the entire budgets of state governments in just a few decades.3
“Medicaid is the largest single expenditure by state governments.”
It is sobering to realize that Medicaid alone costs more than $1,000 per year for every man, woman and child in the country – or $4,000 for a family of four. Since Medicare costs a comparable amount, the average family of four is spending more than $11,000 on other people’s health care – more than many spend on health care and health insurance for their own family.4
Restraining the growth of Medicaid spending is a fiscal imperative for the states. However, squeezing payments to providers or limiting coverage is not the best approach. The best alternative is fundamental reform that introduces competition, encourages private-sector coverage, and allows beneficiaries to make their own choices between health care and other uses of their money. Incremental steps toward these objectives would benefit Medicaid patients as well as taxpayers.
This study addresses problems in state Medicaid programs, surveys promising reforms currently underway in a number of states and recommends a number of changes. Because Medicaid is a joint federal-state program, some fundamental reforms require Congress to address the program’s future in a comprehensive way. But state policymakers can make dramatic changes in program design and cost without new federal legislation.
[page]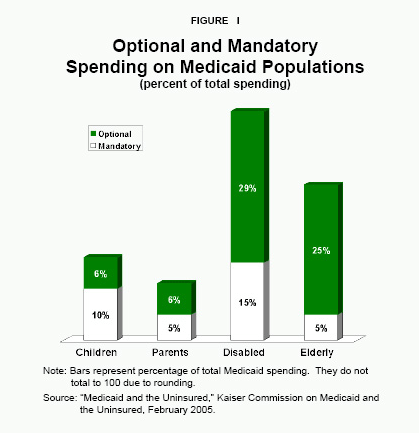
Medicare and Medicaid were created in 1965 as part of President Johnson’s Great Society and War on Poverty. Medicare is a federally-funded health care program for seniors and the disabled. Medicaid is a joint federal-state program for the poor and near poor. Although each state operates its own Medicaid program, the federal government sets the parameters and matches state spending. Medicaid has grown far beyond the program originally envisioned and the scope of the current program is staggering. Nationally, Medicaid covers:
- One in every six people.
- One in every three children
- One in every two births.
- More than one of every two nursing home residents.
The number of Medicaid enrollees nationwide rose by nearly one-third between 2000 and 2004.5 The current enrollment of 53 million is likely to go much higher. An estimated 14 million additional people are potentially eligible but have not enrolled.6 Furthermore, the number of seniors who qualify for Medicaid long-term care benefits is projected to grow rapidly as the baby boomers begin to retire. The population over age 65 will grow nearly two-thirds (64 percent) by 2020, and the number of seniors over age 85 will grow four-fifths by 2025.7
“There are 10 times as many people on Medicaid as on welfare.”
Although Medicaid is commonly assumed to be a health program for welfare recipients, only a small portion of enrollees receive Temporary Assistance for Needy Families (TANF), the main cash assistance program. Furthermore, the number of individuals receiving TANF has fallen from almost 13 million in 1996 to about 5 million in 2003.8 As a result, there are 10 times as many people on Medicaid as there are receiving welfare checks.
Who Qualifies for Medicaid? Federal law requires states to cover certain populations, including low-income seniors and pregnant women, the blind and disabled, and all children living in poverty. In addition to the federal income test, states also impose their own asset tests to determine eligibility. In most states, a Medicaid-eligible individual can own a home, a car and personal property.
States can choose to cover children and families above the poverty level. Every state covers some optional Medicaid populations, and overall they comprise about 29 percent of enrollees.9 Optional populations are typically above the poverty level and include pregnant women, infants and young children. Some states extend eligibility to families at 200 percent to 300 percent of the poverty level, though many of these higher-income groups are enrolled in the State Children’s Health Insurance Program (SCHIP), which provides insurance for children whose parents are not eligible for Medicaid.
- New York, for instance, extends eligibility to include young children (ages one to five) in households with incomes up to 133 percent of the federal poverty level, and infants to age one and pregnant women with incomes up to 200 percent of the federal poverty level.
- Tennessee’s TennCare program covers all infants in families up to 185 percent of the federal poverty level.
In theory, most seniors and most of the disabled are covered by Medicare. However, there is a class of Medicare recipients called dual eligibles. Although they qualify for Medicare, they can also receive Medicaid because of their low incomes and few assets. Medicare is the primary payer, but states must pay for any benefits Medicare doesn’t pay for if Medicaid covers them. More than one-third of all Medicaid costs are for dual eligibles.10
How Do Enrollees Get Medical Care? On paper, Medicaid coverage appears more generous than the benefits the vast majority of Americans receive through private health plans and insurance. Potentially, enrollees can see any doctor or enter any facility and have government pay virtually all costs. In practice, things are different.
“Two-thirds of Medicaid spending is for optional benefi ts; one-third is for mandatory benefi ts.”
Access to Primary Care. Physicians and other health care providers choose whether or not to participate in Medicaid. About 30 percent of doctors do not accept any Medicaid patients, and among those who do, many limit the number they will treat. Access to care at ambulatory (outpatient) clinics is also limited. A recent survey found two-thirds of Medicaid patients were unable to obtain an appointment for urgent ambulatory care. In three-fourths of the cases, the reason was the provider did not accept Medicaid.11
Access to Specialists. The number of specialists who accept Medicaid is particularly limited.12 According to a recent New York Times investigation:
- In New York City, a child on Medicaid with an irregular heartbeat was not able to see cardiac specialist for nearly four months.
- The parents of a boy needing corrective ear surgery were told the wait could be as long as five years.
- At specialty clinics run by teaching hospitals in the city, Medicaid patients often have to wait one to three hours for a 5 to 10 minute appointment with a less-experienced medical resident or intern.13
The problem is not limited to New York City. In 2003, the Denver Post reported that physicians were claiming the University of Colorado Hospital was refusing Medicaid patients, and Medicaid enrollees faced six- to eight-month waits for appointments at specialty clinics.14 In Washington, a 45-year-old Seattle woman admitted to the hospital with a triple fracture of her ankle waited nine days for a doctor to agree to take her case because none of the orthopedic surgeons on staff would accept Medicaid.15
“Nationwide, one-fourth of Medicaid enrollees account for two-thirds of costs.”
Access through Managed Care Plans. Medicaid managed care plans are one way states have attempted to expand access to care, control costs and improve quality. The plans receive a set annual fee per enrollee to provide whatever health services the state covers, and the plans can negotiate higher provider fees than normal Medicaid rates.16 In most states, managed care plans limit the choice of physicians and facilities (as in private insurance plans), but contractual arrangements between physicians and the plans ensure a degree of access Medicaid patients typically do not have. Enrollees who are not in managed care are treated under the old fee-for-service model, but are limited to those doctors and hospitals who participate in Medicaid. Nationally, 61 percent of Medicaid enrollees, about 27 million people, are in managed care.17 The percentage of managed care enrollees ranges from none in a few states to 100 percent in Tennessee.18
In some states, Medicaid managed care plans are operated by public hospitals, and outpatient care is provided by clinics and community health centers. Some provider networks only serve special populations such as pregnant women, and once the women give birth they must transfer to another network.19 Other states contract with networks created by the same private insurers who administer employer-sponsored health plans.20
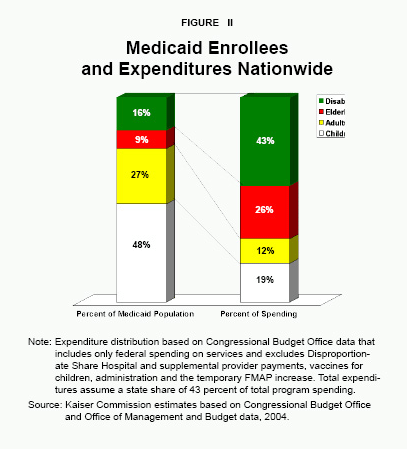
Where Do the Dollars Go? Although less than one-third of enrollees are optional populations, roughly two-thirds of Medicaid spending nationwide is on optional populations and services. [See Figure I.] Poor women and children, most of whom the states are required to cover, make up three-quarters of all enrollees but account for less than one-third of the funds spent.21 By contrast, the elderly and disabled account for about one-fourth of enrollees but more than two-thirds of all costs. [See Figure II.]
States have considerable flexibility to determine the types of services covered by Medicaid. They are required to offer 14 mandatory benefits – such as hospitalization, physician visits and so forth – but they are allowed to choose which of 34 optional benefits to cover, including prescription drugs and long-term care. [See Appendix Table IIa-c.]
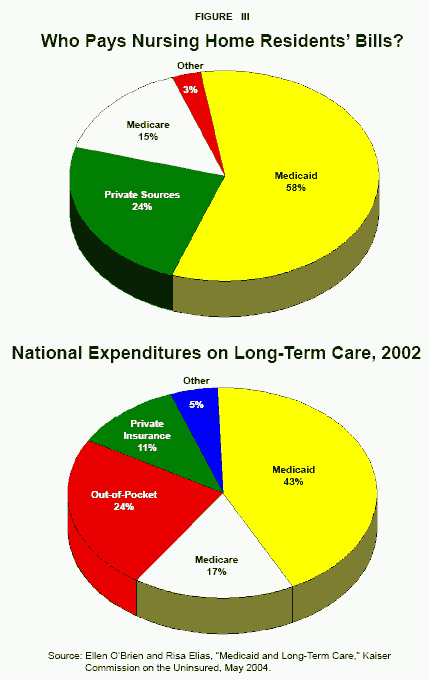
Nursing home care is an optional benefit every state provides. Medicaid pays for 58 percent of all nursing home residents and 43 percent of all long-term care costs nationally. [See Figure III.] Long-term care is used by only 9 percent of all enrollees.22
“Many states receive far more Medicaid dollars than they need, while others get far less.”
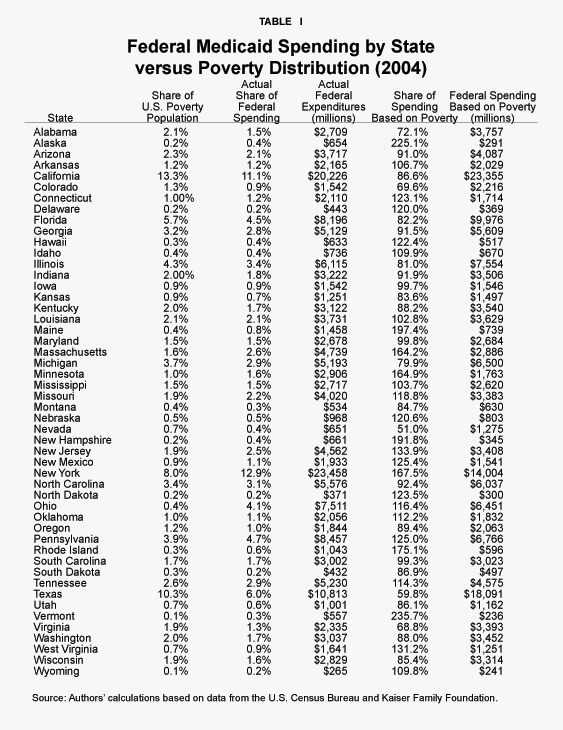
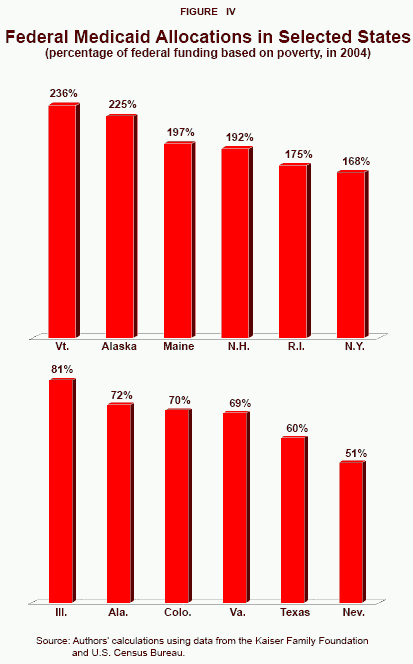
How Is the Federal Contribution Determined?23 One might assume that the federal government’s contribution is based on each state’s poverty population. This is not the case. Using the percentage of the nation’s poor that live in each state as an indication of need, many states receive far more Medicaid dollars than they need while others get far less. [See Table I.] New York, for example, has 8 percent of the nation’s poverty population, but gets 12.9 percent of all federal Medicaid dollars. By contrast, Texas has 10.3 percent of the nation’s poor, but receives only 6 percent of federal Medicaid dollars. As Figure IV shows:
- New York received 68 percent more than it would have if the distribution of funds were based on poverty alone.
- Vermont received more than twice as much as it would if based solely on its poverty population.
- Maine received almost 97 percent more.
Among states that received far less than they would have by this criterion [see Figure IV]:
- Virginia received only 69 percent of what it would have based on its share of the poverty population.
- Texas got about 57 percent of the funds it would have based on poverty.
- Nevada received only 51 percent.
“The distribution of federal funds isn’t based on poverty.”
Poverty versus Other Factors. Arguably, federal Medicaid spending should be based on more than the distribution of poverty.24 It should also consider states’ ability to pay as well as regional differences in the cost of health care. Using state data on poverty, personal income per capita (as a proxy for ability to pay) and personal health expenditures per capita (as a proxy for health care costs), a regression analysis of federal Medicaid dollars spent in each state shows:25
- A 10 percent increase in the state’s poverty rate increases federal Medicaid spending in that state by 8.2 percent.
- A 10 percent increase in the proportion of personal income spent on health increases federal Medicaid spending in a state by 12.6 percent.
- However, a 10 percent increase in a state’s personal income per capita has no effect on federal Medicaid spending.
This implies that per capita health expenditures have a substantially greater effect on the amount of federal funds a state receives than its poverty distribution and that a state’s ability to pay has virtually no effect. Thus, even taking all three factors into account, the current distribution of federal funds is still very unequal:
- Instead of its current 6 percent of federal Medicaid dollars, Texas would receive almost 9 percent if ability to pay and other factors were considered.
- By contrast, instead of its current 12.9 percent, New York would receive only about 7 percent of total federal Medicaid dollars.
These disparities in the distribution of funds are due to the Federal Medicaid Assistance Percentage formula (FMAP), or the “federal match,” used to determine the percentage the federal government contributes to each state’s program. If federal funds were distributed based solely on poverty, some $44 billion – about one-fourth of federal Medicaid spending – would have been distributed to different states in 2004. [See the sidebar “The Federal Matching Formula.”]
Medicaid was intended to improve access to medical care and thereby the health of the indigent. Arguably, it has done neither. And as the program has expanded to cover additional populations, including the near poor and even middle-class individuals, the evidence suggests that it is displacing, or crowding out, private health insurance coverage.
Impact on Access to Care and Quality. It is commonly assumed that Medicaid enrollees have greater access to health care than if they were uninsured; however, the evidence is mixed.
“Medicaid spending substitutes for free care by doctors and hospitals.”
Most enrollees rely on the same public and not-for-profit hospitals and clinics that have always provided a health care safety net for the poor.26 Medicaid is the primary social safety net for indigent health care – but not the only one. For example, community health clinics and hospital emergency rooms are often providers of last resort. The existence of this free care (charity care) often makes people eligible for Medicaid feel that enrollment is unnecessary. Free care, in other words, appears to be a substitute for Medicaid.
“Where Medicaid spending is low, spending on free care is high — and vice versa.”
In fact, where Medicaid spending is low, spending on free care is high – and vice versa. For example, an NCPA analysis of health regions in Texas found that the area with the highest average Medicaid cost per enrollee spent more than twice as much as the area with the lowest average cost.27 But it found that adding spending on free care to Medicaid spending cuts the variation in regional health care expenditures in half. In other words, free care substitutes for Medicaid spending. [See the sidebar “Free Care: The Health Care Safety Net.”]
A recent RAND Corporation study found that among Medicaid enrollees and uninsured individuals who sought care, Medicaid patients received the same quality of health care as the uninsured. Furthermore, the quality of health care received by the poor was only slightly less than for higher income groups.28
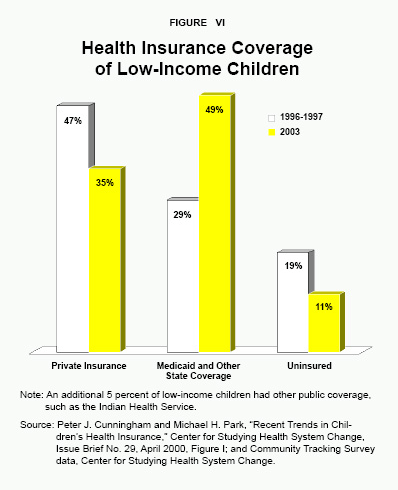
“Medicaid crowds out private insurance coverage.”
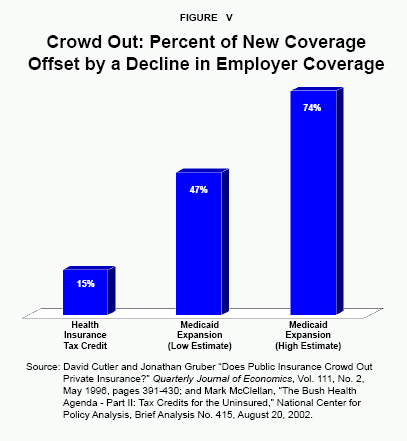
Impact on Private Insurance. Many assume Medicaid insures people who otherwise would not have access to private insurance.29 However, Medicaid also induces some people to drop their private coverage in order to take advantage of free health insurance offered by the state. As a result of such crowding out, the cost of expanding public insurance programs has been high relative to the gain. For example, if for each new enrollee in a public program at least one person forgoes private insurance, there will be no net reduction in the number of uninsured, despite the higher taxpayer burden. If for every two new enrollees in the public program one person loses private insurance, the net cost to the taxpayers for each newly insured person doubles.30
Economists David Cutler and Jonathan Gruber found that Medicaid expansions in the early 1990s were substantially offset by reductions in private coverage.31 For every additional dollar spent on Medicaid, private-sector health care spending was reduced by 50 cents to 75 cents on the average.32 Thus taxpayers incurred a considerable burden, but at least half, and perhaps as much as three-fourths, of the expenditures replaced private-sector spending, rather than buying more or better medical services. [See Figure V.]
In 1997 Congress expanded access to public health insurance with the State Children’s Health Insurance Program (SCHIP). This program provides additional federal matching funds to cover children in families whose incomes are too high to qualify for traditional Medicaid. SCHIP also crowds out private coverage. For example, take a low-income working family covered by an employer-sponsored health plan. The employer might have covered some or all of the cost of insurance premiums for the employee and family with pretax dollars. But paying wages is more attractive to actual and potential employees if coverage is provided by the state. Thus, SCHIP offers some employees the opportunity to increase wages and reduce their health insurance costs.
“Increased Medicaid enrollment was offset by a drop in private insurance coverage.”
As a result of Medicaid and SCHIP expansions, the number of poor children without health insurance fell from 19 percent in 1997 to 11 percent in 2003. During this period, enrollment of low-income children in public programs increased from 29 percent to 49 percent.33 Meanwhile, the percentage of children from low-income families covered by private insurance fell from 47 percent to 35 percent, although there was little change in the percentage of privately insured children in households at higher income levels. [See Figure VI.] A back-of-the-envelope calculation suggests that the crowd out of private insurance due to the expansion of public programs was 0.6, meaning that every percentage point increase in public coverage resulted in a reduction of about 0.6 percentage points in private coverage among low-income children.34
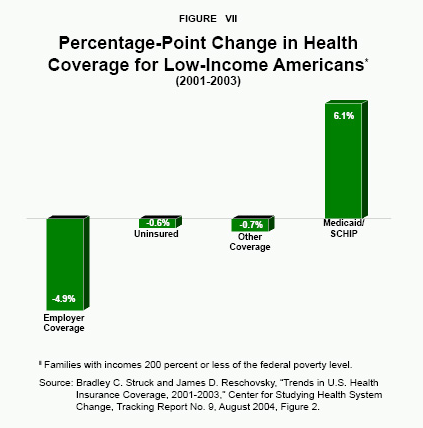
More recently, from 2001 to 2003, the proportion of low-income Americans enrolled in public programs rose 6.1 percentage points. However, this increase was offset by a 4.9 percentage point decline in coverage by employer-sponsored plans. Overall, the rate of uninsured fell only about one-half point.35 [See Figure VII.] Casual empiricism suggests during this period it took a 13 percentage point increase in public coverage to reduce the uninsured rate by 1 percentage point.
Impact on Health. An oft-cited argument for Medicaid is that making health care virtually free at the point of consumption encourages preventive care and improves health outcomes. This could potentially reduce overall, long-term health care costs. Unfortunately, there is little evidence this occurs. Studies suggest explicit attempts to encourage the use of preventive care by Medicaid beneficiaries are generally unsuccessful. For example, one study found that outreach programs in North Carolina had a very small impact on utilization.36 Another study found that receiving Medicaid benefits for a year increased the probability children would receive checkups by only 17 percent. The researchers concluded that “factors other than insurance and income, such as the low educational attainment of low-income mothers, explain approximately 80 percent of the gap between low-income and other children in their well-child visits.”37 Additionally, there is no evidence that becoming eligible for Medicaid significantly improves child immunization rates.38
“Medicaid creates disincentives to work and save.”
However, analyzing the use of Medicaid services tells us only about inputs, not outcomes such as health improvement. The evidence of Medicaid’s effect on health is conflicting. For example, Medicaid eligibility is somewhat associated with a lower risk of infant mortality.39 And University of Washington researchers found some evidence that Medicaid enrollment decreases low-weight births for medically high-risk women.40 Studies in other states, however, have found Medicaid expansion had little effect on prenatal care and outcomes.41
Impact on Income and Wealth. Like other means-tested government benefits, Medicaid creates disincentives to work and save. Income tests discourage work by withdrawing benefits as income rises. Asset tests encourage people to transfer or spend down their assets or avoid saving to become or remain eligible. Knowing their medical needs will be covered by Medicaid, eligible families may boost consumption and save less for emergencies. Economists Aaron Yelowitz and Jonathan Gruber found that Medicaid recipients consumed more and saved less, reducing their average household wealth in 1993 by $1,600 to $2,000 (in today’s dollars).42 Substituting consumption for asset accumulation decreases the likelihood of escaping poverty.43
“Medicaid expansion has been offset by private insurance contraction.”
An increasing number of seniors appear to be arranging their financial affairs in order to qualify for Medicaid long-term care coverage, although the poverty rate among seniors is the lowest of any age group. Furthermore, as a group, seniors have more assets than any other age cohort. According to the U.S. Census Bureau, at all income levels individuals reach age 65 with more household wealth than at any other time in their lives. Senior households aged 65 and older have assets worth an average of $108,885, including home equity.44 Thus, most seniors have enough assets to cover the cost of all but the longest nursing home stay.45 Despite this wealth, a growing number of seniors are spending down or transferring assets to avoid the high costs of long-term care.
[page]Medicaid spending by state varies widely. In 2004, the average state spent 22.3 percent of its budget on Medicaid, ranging from 4.6 percent in Wyoming to 35.2 percent in Tennessee.46 Expenditures per enrollee also vary substantially. New Hampshire spends about $12,093 per enrollee, the most of any state, compared to the nationwide average annual cost of about $6,834. Arkansas, by contrast, spends only $4,410 per enrollee. [See Figure VIII.]
Why Do Some States Spend More Than Others? Some might assume that Medicaid costs are higher in states such as New York because the local cost of living is much higher. However, a comparison of New York City to Columbus, Ohio, where the local cost of living is at the national average, shows:
- In fiscal year 2003-2004, Medicaid spending in New York City averaged $9,842 per enrollee, almost twice as much as the $5,082 spent in Franklin County (Columbus).
- Adjusted for the cost of living in each area, New York City spending per enrollee was still twice as high as in Columbus, Ohio.47
The most important contributing factors to greater spending are policies that encourage more spending and discourage cost control:
- Some states offer coverage to virtually all optional populations, and cover almost all optional services.
- Many state Medicaid programs underpay physicians (69 percent of what Medicare pays, on average) and overpay hospitals, although treatment in doctors’ offices is less expensive than inpatient care or hospital-based clinics.
- Some states pay premium prices for drugs though lower-cost alternatives are often just as effective.
- In all states, the lack of cost-sharing and direct control by patients over some benefits encourages waste and unwise health care choices.
- Many states do not aggressively pursue fraud – even failing to spend a substantial portion of the federal funds available for antifraud efforts.
Many states have imposed regulations on private health insurance that drive up the cost of private coverage, increasing demand for Medicaid services. The following sections examine how these features of the system raise costs.
“Some states spend much more per Medicaid enrollee than other states.”
Costly Policy: Offering More Benefits to More People. One reason Medicaid is so costly is that some states cover virtually all optional populations and provide virtually all optional benefits.48 In Tennessee and New Mexico, Medicaid covers more than one out of every five residents – considerably higher than the national average (14.3 percent).49
“Some states cover virtually all optional populations and benefi ts.”
Upon expanding coverage to parents of Medicaid-eligible children 150 percent to 200 percent above the poverty level, Maine’s Dirigo program now enrolls the largest percentage of the population under the age of 65 of any state -18 percent.50 Additionally, Maine’s Dirigo Health Board of Directors recently approved a new tax on insurers that is projected to raise $44 million to cover costs. Of course, the tax will be passed on to insurance policyholders.51
There are 35 optional Medicaid services for which the federal government will provide matching funds if a state chooses to cover them. [For a list of optional benefits, see Appendix Table IIa-c.] For instance, rehabilitative therapy (covered in 31 states) and podiatry (covered in 27 states). New York tops the list, providing 31 different optional services.52
Optional Benefit: Long-Term Care. One example of an optional benefit that all states provide is long-term care, which either takes place in a nursing home or in a patient’s home. In 2004, 35 percent of national Medicaid spending was allocated to long-term care. But state expenditures vary:
- North Dakota proportionally spent the most – almost 60 percent of its Medicaid budget (or $293 million) – on long-term care.53
- By comparison, Tennessee spent the lowest percentage – 22 percent of its Medicaid budget (or $1.5 billion) – on long-term care.54
What accounts for the variation in spending on long-term care? Some states have a higher proportion of blind, aged and disabled beneficiaries than the U.S. average. In Alabama, Maine, Mississippi and Pennsylvania, more than one-third of enrollees fall into these categories, compared to the national average of 24 percent.55
Also, some states spend more on long-term care per beneficiary. In Connecticut, more than half of the state’s Medicaid expenditures went for long-term care. The state’s nursing home costs rank third highest in the nation, at about $97,000 per patient annually.56
“Ohio taxpayers subsidize 12,000 empty nursing home beds.”
The method used to reimburse nursing homes affects the cost of nursing home care in a state. For example, Ohio and many other states reimburse nursing homes based on the number of beds, not patients. Hence, Ohio taxpayers subsidize about 12,000 empty nursing home beds annually.57 Furthermore, Medicaid reimbursements are based on “cost plus” – the cost of services provided by a nursing home plus a small profit. This discourages nursing homes from reducing costs and improving quality.
Optional Benefit: Personal Care and Home Care. Another widely utilized benefit is personal care and home care. Personal care, sometimes referred to as “custodial care,” generally involves assistance with activities related to daily living (bathing, toilet assistance, eating, grocery shopping, taking medication and housekeeping, although housekeeping cannot be the sole purpose for the personal care). Waivers allow extended services such as transportation and adult day care.58 Home care provides assistance with daily living activities, but also includes skilled nursing.59
Enrollees often begin receiving personal care after discharge from a hospital when a Medicaid official assesses their level of disability and calculates the number of hours of assistance they need for daily living activities. Though home care can be beneficial since it often replaces more expensive nursing home care, it can also be abused. In New York, which provides much more home care than any other state, beneficiaries receive an average of 30 hours of home care per week, compared to the national average of 11 hours per week.60
Once recuperated, most recipients come to expect the higher level of service they received while incapacitated and resist cuts in their personal care. If patients complain, the system generally favors clients over administrators. In New York, for example, Medicaid enrollees have been found to use home care attendants for nonmedical tasks such as shopping. Furthermore, in some cases, assistants are chosen by the recipients themselves, and can include other members of the household, relatives or neighbors. Thus, Medicaid often pays family members to do what they would have done anyway. Many individuals receiving home care could perform more of the tasks themselves and are receiving more assistance than is needed to keep them out of institutionalized care. In these cases, home care often amounts to free maid service.
About half of states that offer personal care services impose hourly per day limits, while about one-third impose cost limits.61 Annual personal care expenditures per enrollee from 1997 to 1998 ranged from $37,596 in Massachusetts to $144 in Arizona (the national average was $6,870).62
“In some places, Medicaid transportation is a free taxi service.”
Optional Benefit: Transportation. States also provide such nonmedical services as transportation.63 For example, New York Medicaid pays for wheelchair-accessible vans to transport enrollees with mobility problems to and from medical treatments. The service is intended to provide transportation only to those who use wheelchairs or who cannot walk without assistance. But many individuals taking ambulette rides have no mobility problems; for them, the service is actually a free taxi service. In 2005, the New York Times reported:64
- Two doctors each ordered more than 90 trips per day for patients.
- At another clinic, one patient used the service 153 times in a single year while another patient used the service 152 times – about one ride every 2.5 days.
- Other patients used the service more than 130 times each.
For patients who qualify for the service, cheaper alternatives exist. A typical bus ride in New York City costs $2 and a taxi ride costs $10, according to the New York Times. But Medicaid typically pays ambulette contractors $25 to $31 each way. Overall, New York Medicaid spent $316 million to transport patients to doctors’ offices and hospitals in 2003. This works out to 10.5 million to 12.5 million rides per year.65
Costly Policy: Underpaying Physicians and Overpaying Hospitals. Routine examinations and treatments – including minor surgical procedures – often can be provided more efficiently and at less cost in a doctor’s office than in a hospital emergency room. Health care providers are reimbursed for routine Medicaid services according to fee schedules set by state administrators. But many doctors do not participate in Medicaid because reimbursement is so low. As a result, the patients turn to much costlier settings, such as hospital clinics and emergency rooms.
The Effects of Underpaying Physicians. In every state, Medicaid reimbursement rates for physicians are typically lower than what physicians receive from the private sector. One way to think about Medicaid physician payments is to compare them to what Medicare pays:
- Medicare pays physicians only 83 percent as much as private insurers, on the average, nationwide.66
- Nationwide, Medicaid fees for physician services average 69 percent of what Medicare pays, according to the American Academy of Pediatrics,67 and perhaps as little as 62 percent, according to an Urban Institute estimate.68

Furthermore, reimbursement fees among states vary widely. For example:69
- Alaska reimburses physicians about 137 percent of what Medicare pays.
- In contrast, Rhode Island’s reimbursement rate for physicians is only 42 percent of what Medicare pays.
“Medicaid usually pays physicians less than Medicare.”
These rates represent an overall average of primary care, obstetric care and other services. There are also stark differences in reimbursement rates for specific services. For instance:70
- A New York doctor receives $30 for a highly complex examination of an established patient, whereas Mississippi pays a physician about $100 for the same exam. [See Table II.]
- l An eye doctor in New York receives $30 for a comprehensive exam of a new patient, whereas Texas and Florida pay more than twice as much for the same service.
These reimbursement rates affect access to care. Laurence C. Baker and Anne Beeson Royalty found that a 10 percent increase in Medicaid fees raised the number of poor patients visiting office-based (private) physicians by 3.4 percent and correspondingly reduced the number visiting public physicians (such as in public health clinics) by 3 percent.71 When private physicians are rewarded for taking complex cases, they have an incentive to accept them. When fees are not adjusted for the complexity of the case, they have an incentive to avoid them.
“Reimbursement rates affect access to care.”
The Effects of Overpaying Hospitals. When access to private physicians is limited, patients rely more on inpatient hospital treatment. In New York, for example, 18 percent of Medicaid patients receive inpatient care compared to just 11 percent nationally.72 Furthermore, in contrast to its reimbursements for physicians, New York pays hospitals generously. When New York deregulated the hospital industry in 1997, the Medicaid fee-for-service system was left largely intact, allowing Medicaid enrollees to go to any public or nonprofit hospital, regardless of its efficiency. Consequently, Medicaid began to pay the highest fees of any payers – including private insurers.73 In most states, Medicaid pays the lowest fees of any payer.
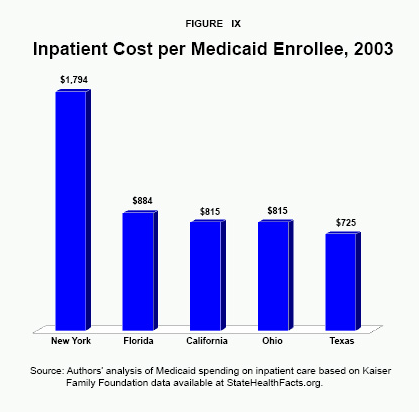
This generous payment policy does not give hospitals any incentive to increase productivity or reduce costs. In 2003, New York Medicaid paid about $10 billion to hospitals for inpatient care, subsidies for graduate medical education and hospital-based clinics – more than any other state Medicaid program. Furthermore, among large states, the inpatient cost per enrollee is greatest in New York at $1,794 in 2003, compared to $725 in Texas, $815 in California and Ohio, and $884 in Florida.74 [See Figure IX.]
Costly Policy: Paying Premium Prices for Drugs. Prescription drug expenditures are one of the fastest growing components of the Medicaid program. From 1990 to 2003, Medicaid’s outpatient prescription drug expenditures rose eight-fold to $33.8 billion nationally.75 There are a number of reasons for this increase.
Many private health plans and most state Medicaid programs have some type of preferred-drug list with increased cost-sharing for drugs that have significantly cheaper alternatives. The drugs are selected through a competitive bidding process, and drug companies usually agree to reimbursement rates that are steeply discounted from the retail price. Many states will only include one drug from a class in the formulary.
Some states have taken steps to reduce drug spending but not all efforts are successful. For example, New York recently began encouraging the use of generic drugs, but doctors can easily substitute higher-priced brand-name drugs.76
As with other types of managed care there is a danger that drug formularies can become bureaucratic obstacles that prevent patients from getting the drugs they need. Also, administrators may be tempted to sacrifice quality care in order to reduce costs. Ideal drug policies minimize costs without harming patient welfare. Poor drug policies harm patients and may (because of adverse health effects) not even reduce costs.77
Frank Lichtenberg of Columbia University has found that newer, more-expensive drugs may offer more effective treatment and reduce total health care costs. Lichtenberg found that lowering the average age of drugs used by roughly a decade (that is, from 15 years to 5.5 years) results in an increase of $18 in drug spending but a net reduction in total health care spending by $111. Most of the net reduction was due to decreased hospitalizations and fewer office visits.78
Prescription drugs can also reduce Medicaid program costs by substituting for expensive emergency treatments. For example:79
- Spending just $4,500 a year for pricey atypical anti-psychotic drugs could save $73,000 a year in institutional costs for the mentally ill.
- “Clot buster” drugs for strokes could save about four times the drug price by reducing the cost of treating patients in hospitals.
“New York spending per patient is higher than in other large states.”
Furthermore, as Linda Gorman of the Independence Institute notes, Medicaid populations tend to have a disproportionate number of people who need newer, more-expensive drugs with fewer side effects.80
Costly Policy: Ineffective Managed Care. As noted, managed care was introduced into Medicaid in order to increase access to care and to provide services efficiently. Managed care organizations usually contract with area hospitals and doctors to provide services at negotiated discounts. In 2004, enrollment rates for the Medicaid population were as high as 88 percent in Arizona.81 In fact, all but seven states have at least half of their Medicaid beneficiaries enrolled in managed care plans.82
However, most states exempt substantial patient populations from their mandatory managed care enrollment: the elderly and disabled, who are the most intensive users of Medicaid. In New York, for example, 70 percent of Medicaid costs are for the elderly and disabled. For many of them, managed care is not even available on a voluntary basis. The average yearly cost per person to care for them is 10 times higher than for nondisabled children and five times the cost of caring for the parents of nondisabled children. Exempting the most intensive users of Medicaid services from cost-control efforts is an expensive missed opportunity. These patient groups have problems accessing care and could benefit from the continuum of care and case management that managed care networks offer.
An alternative to managed care is to allow patients to manage their own health care dollars and shop for care as empowered consumers in the medical marketplace. This option will be considered below.
Costly Policy: Little or No Cost-Sharing. Economic theory predicts that individuals will consume more of a good if it is free. Health care is no exception. Therefore, Medicaid recipients who pay no copays or deductibles are not aware of the cost of health care services and have no incentive to economize.
“Medicaid recipients have no incentive to economize.”
Many states recognize the necessity of cost-sharing and have imposed small copays of 50 cents to $3.00 on prescription drugs or office visits for Medicaid recipients. But critics argue that even small copays – while leading to a reduction in the use of Medicaid services – hurt the poor by discouraging them from purchasing necessary drugs or services. Some studies show this leads to an increase in costly adverse medical events and emergency room visits, which defeat the purpose of cost-sharing.83 Furthermore, some cost-sharing programs – in Michigan and Minnesota, for example – have been found to violate the federal Medicaid Act, which prohibits withholding care or services to recipients based on their ability to pay.84 However, there are forms of personal health accounts, discussed later in this paper – such as reverse HSAs – that would give patients incentives to reduce unnecessary utilization of health care, while encouraging them to seek needed care.
Costly Policy: Treatment Errors and Adverse Medical Events. Eliminating errors in diagnosis can lead to better treatment at lower cost.85 Some of the most dangerous and costly problems in our health system include drug misuse, antibiotic overuse, preventable hospital-acquired infections, and the under-diagnosis and mistreatment of chronic conditions.86 The Institute of Medicine found that between 44,000 and 98,000 people die each year from preventable medical errors. Further, medical errors cost the health care system an estimated $37.6 billion a year, of which $17 billion is due to preventable errors.87
Researchers found no one particular cause of medical errors; instead, they found multiple causes that result in a larger systemic failure of hospital protocols. They classified these errors into two categories:88 1) active errors by health care providers (that is, doctor, nurse or other worker), which are usually detected quickly, and 2) latent errors, such as poor system maintenance or equipment design or poorly organized health care systems, which are more difficult to detect because they are beyond the control of individual caregivers.
A 2000 study by the Agency for Healthcare Research and Quality found that children in the Medicaid program were more likely to experience treatment errors than children on private insurance.89 They were also more likely to be victims of post-care infections, postoperative respiratory failure and postoperative sepsis.90
Another quality problem is adverse drug events, which are common among the elderly. A Massachusetts study found that the elderly population in nursing homes was especially vulnerable:91
- Adverse drugs events occurred at a rate of 1.89 for every 100 resident months; hence, the risk of occurrence is almost 25 percent annually.
- Of the 546 adverse drug events examined, 38 percent were considered serious, 6 percent were life-threatening and one was fatal.
- However, about 51 percent were considered preventable.
Since Medicaid covers 58 percent of nursing home patients, this implies that Medicaid patients are particularly at risk.
“Hospital-acquired infections are the fourth-largest killer in America.”
Costly Policy: Failure to Control Infections. Hospital-acquired infections are the fourth-largest killer in America. A recent report found that nearly 100,000 people may die annually of hospital-acquired infections alone.92 Even more frightening, a new and deadly infection known as MRSA (methicillin-resistant Staphylococcus auerus) does not respond to commonly used antibiotics. Many Medicaid hospital patients are infected with this dangerous disease. In 2003, 57 percent of staph infections were a result of MRSA, and the percentage is rising. Infections of all kinds are common in nursing homes, but MRSA infections are on the rise and the prognosis is worse for the elderly than for the young. Infections in long-term care facilities result in one-quarter to one-half of transfers to hospitals.93
Costly Policy: Failure to Control Fraud and Abuse. Fraud and abuse have plagued Medicaid since its inception. In 1997, the Government Accountability Office estimated that fraud and abuse may be as high as 10 percent of Medicaid spending.94 For example, a 1993 investigative report of the Illinois Medicaid system by the Chicago Tribune found:95
- In one year, 71,064 Medicaid patients visited a doctor’s office more than 11 times (compared to a national average of six visits per year), while four patients made more than 300 visits in one year.
- In one day, one patient saw five doctors, visited a pharmacy seven times and had 22 prescriptions filled with 663 pills.
- Attempts by government to rein in these abuses have resulted in some improvements, but fraud involving the use of Medicaid transportation still abounds. Recently, for example:
- In Illinois, a woman operating transportation services from her home for Medicaid recipients was found guilty of $150,104 worth of false billings for mileage, attendants and a wheelchair-accessible van.96
- A New Jersey transportation operator was sentenced to state prison for billing Medicaid for unauthorized uses of transportation (to nonmedical destinations) and kickbacks worth $214,840.97
“Fraud and abuse may be as high as 10 percent of Medicaid spending.”
The Tribune also uncovered “Medicaid mills” that freely prescribed drugs, syringes and other medical products that were then sold by patients on the street. More recently, a year-long investigation of New York Medicaid by the New York Times found massive provider fraud. For example:98
- Dr. Rosen, a dentist in New York’s Medicaid program, claimed to have performed nearly 1,000 procedures in a single day.
- In September alone she claimed to have performed 9,500 procedures.
- All told, she and a colleague billed New York Medicaid $5.4 million in 2003.
Most fraud is committed by physicians and other providers, rather than patients, but providers often turn a blind eye to unscrupulous patients abusing or defrauding the system. For instance, the Times reports that a Brooklyn doctor prescribed more than $11 million worth of a synthetic growth hormone used to treat AIDS patients over a three year period. Investigators say these patients were part of an elaborate scheme to obtain a drug popular with bodybuilders buying on the black market. New York Medicaid’s yearly cost for this growth hormone grew from $7 million to $50 million within a year of the scheme becoming prevalent.
Another source of fraud and abuse is the federal Supplemental Security Income (SSI) program. Many people with disabilities access Medicaid benefits by qualifying for SSI. Since coverage is often related to medical conditions that are fairly easy to fabricate or exaggerate, individuals and parents have incentives to misrepresent medical conditions. For example, according to the Government Accountability Office (GAO), “middlemen” provide translation services to beneficiaries who do not speak English and coach them on feigning and exaggerating mental disabilities in order to receive SSI benefits. Middlemen also work with dishonest health care providers to supply faulty medical information. Additionally, a number of SSI recipients have admitted to transferring ownership of assets in order to quality for SSI benefits: 99
- Between 1990 and 1994, an estimated $74 million in assets were transferred, including cars, cash, houses and land.
- Between 1996 and 1997, the Inspector General’s Office received 12,680 complaints of SSI fraud, constituting about 37 percent of all fraud allegations received from the public.
Thus, these recipients “game” the system to obtain coverage.
“State regulations raise the cost of private health insurance.”
Costly Policy: Regulations That Raise the Cost of Private Insurance. As noted, Medicaid crowds out private insurance coverage by offering a free alternative. Contributing to that rise are regulations that raise the cost of health insurance. Nationwide, state insurance mandates require private carriers to cover more than 1,800 specific benefits and service providers (such as acupuncturists and chiropractors).100 These mandates raise the cost of health insurance. Economists estimate that up to one-fourth of the uninsured are priced out of the market for health insurance due to cost-increasing regulations.101
Two regulations are particularly notable. Community rating charges enrollees the same premium regardless of health status. In doing so, it essentially overcharges young, healthy individuals to cross-subsidize older, less-healthy individuals. Enrollees who are overcharged are prone to drop their coverage. Guaranteed issue, which requires insurance companies to provide health insurance regardless of an individual’s health status, makes it easy for people to wait to obtain insurance until after they become sick. With fewer and fewer healthy individuals to offset the sick, the risk pool becomes increasingly unhealthy. Over time, this cycle causes premiums to sky-rocket and insurance becomes unaffordable.
[page]If state Medicaid programs were as efficient as most private-sector health plans, they could spend billions of dollars less to achieve the same health outcomes and would have billions of dollars each year to fund tax cuts or other spending programs.
Section 1115 waivers, granted by the Centers for Medicare and Medicaid Services (CMS), have traditionally been used to test innovative, comprehensive Medicaid reform. In 2001, the Bush administration announced a streamlined waiver process called the Health Insurance Flexibility and Accountability (HIFA) initiative. Through HIFA waivers, states have the opportunity to reduce some benefits in order to increase other benefits, reduce benefits in return for increases in the number of people eligible, and/or reduce benefits for some people in order to create a new set of benefits for others.102
“Waivers allow states to implement reforms.”
There are certain restrictions on the waivers.103 They are usually valid for only three years (although they can be renewed). They must be budget neutral (that is, require no additional federal spending). The state must be trying to “research an idea” (rather than just trying to cut costs). Certain populations must be “held harmless” (usually pregnant women and children). Certain benefits must be protected. However, states can adjust almost all benefit, eligibility and reimbursement standards. If the waiver proves unsuccessful at any time, the state can unilaterally cancel it after closing the pro-gram to new enrollees for six months.
In addition, the Deficit Reduction Act of 2005 gives states new authority to adopt many common-sense reforms that formerly required federal waivers. [See the sidebar “The Deficit Reduction Act of 2005.”]
[page]To reduce Medicaid costs, states should begin by employing measures that are common in the private sector and that achieve results. Some states are already implementing these reforms, and the following are some examples.
“There are many opportunities to improve quality and control costs.”
Substituting Less-Expensive for More-Expensive Therapies. Treatment in outpatient settings, such as doctors’ offices, is generally less expensive than treatment in a hospital. However, Medicaid patients have limited access to physicians other than in public health clinics or hospital emergency rooms. Paying higher physician fees for examinations, tests and procedures that can be performed in a doctor’s office would increase patients’ access to health care and reduce expensive emergency room visits.
Performing more procedures in outpatient settings that were once only performed in hospitals (such as minor surgeries that don’t require an overnight stay) is a common way of reducing costs.104 A Pennsylvania study found that about 10 percent of all hospitalizations for patients under age 65 are potentially avoidable. Caring for these patients in lower-cost, more-appropriate settings could have saved the state about $2.8 billion in 2003. In some cases, procedures performed in hospitals could have been done in outpatient clinics. In other cases, inpatient care could have been avoided by timely physician care.105
West Virginia, for example, recently changed its Medicaid program to give recipients the option to sign a “personal responsibility contract,” stipulating certain requirements such as using emergency room services only for emergencies and not being late for doctor’s appointments. In return, beneficiaries will receive credits they can use for other health benefits, such as fees for exercise classes. The contract is optional, but will apply to about 160,000 beneficiaries. Those who choose not to sign a contract will have more limited benefits than those who do.106
Substituting Less-Expensive for More-Expensive Providers. Why pay more when the same quality of care is available for less? Private-sector health plans routinely contract selectively, choosing to direct enrollees to providers who charge less for the same level of quality. These plans typically require enrollees to use facilities and physicians that are “in-network,” or to pay a larger share of the cost if they use providers that are “out-of-network.”
Medicaid could selectively contract specific high-cost procedures to “Centers of Excellence,” which are hospitals that perform a high volume of particular procedures for which there is a demonstrated relationship between volume and quality. Hospitals that do not receive contracts would not be reimbursed unless the services were preauthorized or the patient was admitted due to an emergency. This is a modest reform that is long overdue.107
Through specialization, hospitals can perform a large volume of procedures or care for a large volume of patients with similar conditions at a lower cost. Hospitals can reduce costs by eliminating inefficiencies, including unnecessary services, excessively long hospital stays, excessive compensation to noncritical staff, inefficient staffing levels and so forth. Hospital executives will find innovative ways to cut costs when they have better incentives to do so.108
“Selective contracting provides opportunities to negotiate discounts.”
Selective contracting provides opportunities to negotiate discounts for most medical services. Many states use competitive bidding and selective contracting for eyeglasses, medical equipment, transportation and other services.109 For example, Medi-Cal, California’s Medicaid program, began selective contracting for hospital services in the early 1980s. Four years later the state was spending nearly 8 percent less than it was projected to spend without selective contracting.110 The Centers for Medicare and Medicaid Services (CMS) found that contracting reduced the daily cost of a hospital stay about 16 percent below what it otherwise would have been. The greatest savings were in areas with stiff competition among hospitals.111
Other states have also had success with selective contracting. For example: 112
- Oregon implemented selective contracting for its Medicaid transportation services and saved 15 percent while increasing patients’ access to care.
- Colorado saved about $6.5 million by contracting out its mental health services in 1996.
Substituting Less-Expensive for More-Expensive Drugs. Private-sector managed care plans use a variety of techniques to control drug costs, including preferred-drug lists, formularies, negotiated prices with drug companies and single-source drug distributors. For example, many plans require enrollees to use a specific mail-order drug supplier to avoid higher copays. Health plans frequently contract with a pharmacy benefit manager (PBM) to handle drug benefits. PBMs require enrollees to obtain a preauthorization to purchase brand-name drugs that aren’t on their list of preferred or formulary drugs, or to use a non-network pharmacy.
However, patients may prefer a drug that is not on the formulary; an alternative drug may be more effective, or have fewer side effects, for them. If a patient is willing to pay a higher share of the costs, they can usually obtain coverage for these drugs. Health Savings Accounts or Flexible Spending Accounts can also help defray the increased cost of nonformulary drugs. And the same principle can be applied to Medicaid enrollees (see the section on Personal Health Accounts following).
Medicaid managed care plans generally also use PBMs to manage their drug benefits. However, some states have rules and regulations that limit the ability of PBMs to control drug costs. For instance, some states have laws that prevent a PBM from requiring the substitution of generic drugs for expensive brand-name drugs.113 Other states have bills pending that would further limit PBMs. In New York, for example, legislation was introduced to limit the ability of PBMs to require the use of mail-order pharmacies.114 Another bill would require PBMs to reimburse any pharmacy willing to meet the requirements of a drug plan. These measures would limit the discounts PBMs are able to negotiate with competing pharmacies.
“Generic drugs often can save money without any reduction in quality.”
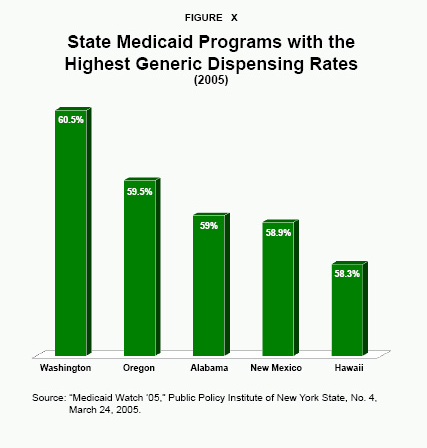
Additionally, several states do not take advantage of cheaper generic drugs that are of the same quality as name-brand drugs. Generics account for 51.9 percent of all drugs dispensed by state Medicaid programs. Washington, Oregon, Alabama New Mexico and Hawaii have the highest dispensing rates. [See Figure X]. On the other hand, California, Connecticut, Texas, Louisiana and New Jersey use far fewer generic drugs than the average state.115 These states should en-courage the use of less-expensive drug alternatives when quality is the same – including therapeutic, generic and over-the-counter substitutes. Patients who prefer brand-name drugs should be able to choose them if they make a copayment, as they would in a private insurance plan.
A 2003 study from Brigham and Women’s Hospital and Harvard Medical School examined the effect of substituting comparable generic drugs for brand-name drugs in an unnamed state’s Medicaid program. The cost of the brand-name drugs purchased through Medicaid totaled about $95.3 million.116 Among commonly prescribed drugs, they found:
- The use of generic anti-anxiety medicine would have saved $461,000.
- Using generic calcium channel blockers would have saved $420,000.
- Generic nonsteroidal, anti-inflammatory drugs would have saved Medicaid $294,000.
There were other drugs savings as well. Using just the generic form of the top-three prescribed drugs would have saved the state’s Medicaid program well over $1 million. Total savings on all drugs examined would have totaled $3.4 million.
“Medicaid will not pay for over-the-counter drugs that can substitute for prescription drugs.”
In the past few years, a number of prescription drugs have been moved over the counter and are available at a much lower cost and without a prescription. For example, when Claritin, a prescription drug used by allergy sufferers, became available over the counter, the price fell substantially. The current prescription version of the drug, called Clarinex, is chemically similar.117 Yet a year’s supply of Clarinex costs about $800, compared to only $190 for Claritin and less than $16 for an over-the-counter generic equivalent.118 Another example is Nexium, the prescription version of the heartburn medication Prilosec. Nexium costs $146 for 30 capsules at drugstore.com, for a daily cost of about $4.83. Costco.com sells a box of over-the-counter Prilosec with 42 capsules for $25.99, for a daily cost of $0.62.
In 2006, the drug company GlaxoSmithKline USA asked the FDA for the right to sell the obesity drug Xenical (Orlistat) over the counter. Glaxo expects the over-the-counter version to cost about two-thirds less than the prescription price.119 However, past experience indicates that many doctors will continue to prescribe the prescription version because it will cost Medicaid patients less out of pocket, even if they are charged a small copay (usually $3). Unfortunately, Medicaid (and Medicare) will not pay for over-the-counter drugs, even if they can be substituted for more-expensive prescription drug therapies.
Furthermore, there is a danger that drug formularies will become bureaucratic obstacles to needed therapies, particularly for patients who cannot pay higher copays for nonformulary drugs. Economist Linda Gorman of the Independence Institute reports that substituting generics for brand-name drugs can adversely affect patients. For example:120
- A survey of 200 physicians in Tennessee’s TennCare program found that two-thirds of doctors reported they had patients who had serious adverse reactions, including death and stroke, when they were switched to generic substitutes.
- In a British Columbia survey, 27 percent of doctors reported admitting patients to hospital emergency rooms as a result of having switched them to drugs mandated by government formularies.
One way to resolve these problems is to allow Medicaid patients to control some of the funds for their own health care. States should consider allowing patients and their physicians, rather than bureaucrats, to make these choices.
Contracting with the Private Sector. Instead of paying for Medicaid services on a fee-for-service basis, states could contract with hospitals, clinics and physicians for specific services and therapies. This would allow the program to coordinate care and establish quality standards.
Disease Management and Care Coordination. Many patients have multiple illnesses that require treatment by different specialists or in different facilities.121 Unfortunately, these health care providers often have little (if any) contact with one another. The lack of coordination leads to poor-quality health care and medical errors, such as harmful drug interactions.
“Coordinated care could reduce harmful drug interactions.”
Coordinating care typically involves a case manager who reviews the patient’s medical history and claims data, ensures providers communicate with each other about the patient’s condition and monitors the patient’s progress. Case managers can help ensure appropriate care is given and clinical protocols are followed. Coordinated care allows health care providers and state social service agencies to exchange relevant information about all the services received by a patient.
Coordinated care can reduce the risk of adverse drug interactions from inappropriate or contraindicated drugs. Recent studies have found that seniors often take too many medications – many of which are contraindicated. About 20 percent of seniors – seven million – have at least one prescription each year that is questionable.122 Often, one medication is used merely to combat the side effects of another drug.123 A demonstration project funded by the Robert Wood Johnson Foundation reduced the use of medications judged to be potentially inappropriate by more than one-third (36 percent) over the course of 18 months.124
Disease management involves developing a treatment plan based on current treatment protocols for patients and training them how to the follow protocols.125 With the help of a case manager, patients formulate a plan for the control and treatment of their condition. The plan is essentially a list of established guidelines indicating which actions to take in response to various symptoms.126 Although monitored by a physician, much of the day-to-day care is administered by patients themselves so training is a necessary part of such programs.
As of 2004, nine states had implemented disease management programs. While results are preliminary, these programs appear to reduce costs and improve treatment for chronic conditions:127
- In Colorado, average costs for asthmatics participating in disease management programs dropped 37 percent.
- The proportion of asthmatics receiving inhaled steroid treatment increased from 49 percent to 95 percent.
- In Washington, a diabetic disease management program saved $900,000 in its first year, and the percentage of diabetics taking daily aspirin or other blood thinners increased from 41 percent to 64 percent.
“In Colorado, disease management reduced costs 37 percent for asthmatics.”
In 2005, Utah established a Primary Care Network (PCN) that stresses preventive care and disease management.128 In fact, in a 2005 performance survey, recipients rated the Utah plan (on a scale of 1 to 10) more highly than recipients rated Medicaid nationwide with respect to getting needed care, how well doctors communicated with patients and the helpfulness of office staff. Furthermore, Utah’s plan ranked above the national average in the timeliness of prenatal and post-partum care and the rate of immunizations for children up to two years of age.129 [See the sidebar on “The Utah Experience.”]
“Patients can be trained to manage chronic conditions.”
Self-Managed Care. Patients can also be trained to manage their own care, including administering drugs, monitoring vital signs, caring for wounds and so forth. For example, numerous studies have shown considerable benefit from self-management training for patients with Type 2 diabetes.130 Diabetes is the sixth leading cause of death by disease in the United States. Diabetics spend four times more money on health care than nondiabetics.131 By one estimate, nearly $2.5 billion in annual hospital costs for diabetes complications could be averted with appropriate self-managed care.132 Patients can be taught to inject insulin, monitor and maintain a log of blood glucose levels, and use the results to adjust their dietary intake, activity levels and medicine doses.133 In addition, many diabetics can reduce reliance on medications and control their diabetes completely by adhering to a meal plan, losing weight and exercising.134
Uncontrolled asthma is another costly chronic disease.135 The Asthma and Allergy Foundations of America estimates nearly 20 million Americans suffer from asthma – resulting in 500,000 hospital stays each year.136 More than 2.5 million school-age children suffer from asthma, missing nearly 15 million school days per year. The economic loss averages out to nearly $800 per child per year.137 A Dutch study comparing self-management to standard care with a primary physician found that the treatment costs of those patients who monitored their own asthma cost about 7 percent less than conventional care the first year and 28 percent less the second year.138
Caring for Special-Needs Patients. The problems of people with disabilities and chronic conditions range from schizophrenia to mental retardation to blindness to diabetes. These conditions require special therapies and specialists that many Medicaid patients may have difficulty accessing. If payments to managed care plans are not adjusted for the cost of caring for these patients, they have an incentive to avoid enrolling them or to skimp on care. Medicaid should contract with specialists and specialized facilities for these patients, pay risk-adjusted premiums based on the cost of care and offer incentives for performance (discussed below). For example, a network providing care for psychiatric patients could be given incentives to use outpatient therapy and drug treatment rather than more costly institutional care when it can achieve the same therapeutic outcomes.
Florida contracts with various private-sector entities to serve people with specific types of disabilities. This allows benefits to be tailored to the needs of the individual enrollee.139 States that do not use private-sector contractors should explore such opportunities. For example, different providers could serve the mentally ill, the physically disabled, the drug addicted and so forth. The comparative advantage of these various providers would reduce costs and increase the quality of service.140
The services provided by contractors could be limited to those related to the disability. Regular Medicaid could provide other health services, or the disabled/chronically ill could be offered premium support to purchase other coverage. Higher-cost individuals with disabilities could be provided a larger personal health account to cover their needs (discussed below). This would allow them a choice of benefits and health plans similar to the HIFA waivers in Florida and South Carolina.
“Patient satisfaction with Cash and Counseling programs is almost 100 percent!”
Cash Accounts for Patients with Disabilities. About half of the states have set up cash accounts disabled Medicaid enrollees can use to manage their own health care dollars and directly purchase needed services.141 These pro-grams, often called “Cash and Counseling,” use a defined contribution approach.142 The patient is given a set dollar contribution and is free to choose his or her providers. The programs also involve counseling to assure that the patient is well-informed. Under traditional Medicaid, the states select the providers without patient input. Under this program, the patient can now choose his or her own provider. Surveys of participants in the program show that they have a higher quality of life with fewer unmet health needs.143 Remarkably, patient satisfaction is almost 100 percent.144
Pay for Performance. A 2002 National Academy of Sciences report recommended that all federal health programs begin paying for quality care rather than paying for services rendered.145 The NAS says the programs should initially focus on the treatment of health conditions that account for most of the spending in public health programs, such as diabetes, depression, osteoporosis, asthma, heart disease and stroke.
Medicare has begun implementing pay-for-performance initiatives.146 Medicaid would also benefit from such initiatives. If a state program only paid providers for outcomes it deemed worthwhile, it might reap significant savings. For example, Bridges to Excellence, an initiative of the Robert Wood Johnson Foundation, pays additional funds to physicians of diabetics in private health plans who achieve certain quality standards. The cost per diabetic is about $175, but that is only half of the estimated saving per diabetic patient from the reduction in treatment complications.147
Reducing Medical Errors and Improving Quality of Care. Eliminating errors in diagnosis can lead to better treatment at lower cost.148 Many states have created patient safety databases, which allow consumers to research the outcome records of hospitals and physicians. These help to level the playing field of information between patients and health care providers. Currently, 20 out of 50 states have some type of patient safety database. Most require only the reporting of errors that lead to serious injury or death, while less-serious errors can be reported on a voluntary basis. Additionally, 19 states have confidentiality rules barring information on medical errors from being used in malpractice litigation against hospitals or physicians.149
A recent study examined the effect of New York’s Cardiac Surgery Reporting System (CSRS) on patient health outcomes. Authors David Cutler, Robert Huckman and Mary Beth Landrum examined CSRS data from 1991 to 1999 on death rates in New York hospitals that performed cardiac catheterization procedures. The study, published by the National Bureau of Economic Research, found:150
- Moving from a low-quality to a higher-quality hospital would significantly reduce a patient’s risk-adjusted mortality rate.
- Patient admissions increased at hospitals with low mortality rates the first year following a favorable CSRS report; however, the increased number of cases dropped off after the first year.
- Patient admissions at hospitals identified as having a lower quality of surgery declined by about 10 percent during the year following a poor CSRS rating report; the decline remained stable for three years.
- Low-quality hospitals were still performing the same number of emergency surgeries as before the report, indicating that some patients cannot or do not shop around for better-quality hospitals in emergency situations.
“Paying for results improves quality.”
Furthermore, the NBER study suggests that since cardiac surgery is profitable for hospitals, they will improve their quality of care to attract new patients to replace ones that have gone elsewhere.
Medicaid should contract only with providers that institute infection-control programs. Payments to hospitals could be adjusted to reward facilities that achieve low infection rates and penalize those with higher infection rates. Hospital-acquired infections are a type of medical error that should be measured for quality ratings and addressed in contracts with providers.
Some hospitals are taking aggressive steps to improve quality of care by reducing infection rates, and both state and federal policies are changing to reduce this spreading epidemic:
- Some hospitals, such as the University of Pittsburgh system, are imposing stiff penalties, including termination and suspension of practice privileges for staff and doctors who fail to wash their hands.
- Some states have passed laws that publicize a hospital’s “infection report card,” allowing patients to compare hospital infection rates before surgery; ideally, hospitals would compete for patients by reducing infection rates.
Additionally, the 21st Century Information Act, introduced in Congress last year, would authorize grants to establish regional electronic databases among groups of hospitals, health care providers, insurers and patient groups. The government would make matching payments to states whose electronic health care networks benefit Medicaid providers.151
Health care providers are already taking steps to establish electronic medical records. Many hospitals are using bar-code or radio-frequency technology on patient identification bracelets to ensure medications are administered to the correct patient at the correct dosage. Nursing homes can benefit from such a program as well, since, as discussed earlier, medication errors can be a problem for the elderly in long-term care institutions. [For a discussion of steps states can take to improve the quality of nursing home care, see the sidebar “Improving Nursing Home Quality.”]
“Software can help identify fraud.”
Pursuing Fraud Aggressively. Some states have established Medicaid provider information exchange databases to identify fraud, abuse, overuse and unnecessary care. In other states, most abuse is identified through tips and other unreliable means. Establishing a state database of billing information on Medicaid providers in New York has proven useful. If one provider’s Medicaid billing began to increase significantly, case workers can quickly identify and check into the trend.152 The provisions of current “whistleblower” laws that allow private citizens who identify fraudulent providers to receive some of the recovered funds may also be useful in fighting fraud.
Software firms have developed information technology to more easily examine Medicaid billings using a number of different criteria. Salient Corporation is working with Chemung County, New York, to better manage Medicaid spending. Using Muni-Minder software, officials can analyze the billings of individual suppliers and track product and service utilization, allowing them to uncover inefficiency, waste and abuse anywhere in the program. For example, Muni-Minder allows investigators to quickly identify the number and cost of prescriptions for brand-name drugs filled when a generic was available. A chart of the amount per recipient spent for any provider is easily created with only a few keystrokes.153
Despite the political difficulties in cracking down on fraud, states have taken action on Medicaid fraud and abuse. In 2003, Texas established an inspector general’s office responsible for detecting Medicaid fraud. As a result, Texas recovered $441 million in 2005 from erroneous or fraudulent charges.154 Kansas recently followed suit. In addition, a recently-enacted Kansas law makes Medicaid fraud a civil matter – as well as a criminal offense – thereby enabling the state to recover improperly paid Medicaid money.155
[page]“Ultimately, Medicaid reform should move patients to private health plans.”
The ultimate goal of Medicaid reform should be to move patients to the same type of private health plans most Americans have. Medicaid enrollees should have the same opportunities to benefit from the innovations and greater access to care found in the private sector. In order to move in that direction, states should encourage private insurance, remove barriers to competition and allow Medicaid recipients to participate in private plans.
Encouraging Private Insurance. In many states, taxpayers foot the bill for Medicaid benefits that are more generous than the coverage provided by private health insurance plans. This is unfair and unwise. It is unfair because taxpayers should not be forced to provide others with better health benefits than they purchase for themselves and their families. It is unwise because Medicaid recipients are largely insulated from many of the cost-controlling, quality-improving innovations used by private-sector plans. For example, Medicaid enrollees are not subject to copays and deductibles, and they are provided benefits such as free transportation to appointments and virtually free prescription drugs – perks that are almost unheard of in private health plans.156
“Private-sector competition would benefit Medicaid Patients.”
Private-sector plans may appear less generous on paper than the current Medicaid program, but they usually allow enrollees access to a greater range of providers and facilities. For example, enrollees in a Florida pilot program will be allowed to use their Medicaid funds to pay premiums for employer-sponsored plans where they work or choose coverage from among competing private insurers. For some patients, this will essentially move Florida Medicaid from a defined benefit entitlement to a defined contribution plan.157 Beneficiaries will receive risk-adjusted credits that reflect their health status with which to purchase managed care plans from providers.158 They will be able to choose among competing plans with different benefit packages.159
Private-sector plans have incentives to control costs and improve quality when they compete for customers in the marketplace. Other states should allow Medicaid patients to enroll in private-sector plans, including employer plans and individually owned insurance. They should also be allowed to enroll in the same plans that cover state employees. Medicaid patients should be allowed to benefit from such competition.
Competition to Insure Medicaid Enrollees. One way a state can provide an incentive for insurers to compete for Medicaid enrollees is by creating a marketplace where providers offer health insurance to beneficiaries. The role of the state would change from being the buyer of health care to facilitating a real marketplace in Medicaid.160 The state could underwrite actuarially fair credits for enrollees to purchase services from providers. Properly designed risk-adjusted payments could avoid the problem of “cherry picking” healthier (that is, cheap-to-treat) enrollees. Software is being developed for risk-adjustment. The Centers for Medicare and Medicaid Services has implemented a new plan to rate-adjust Medicare managed care payments based on more than 70 variables. Medicaid managed care programs could use a similar system.161
An additional method to avoid “cherry picking” is to require an actuarial payment from one provider to another when enrollees switch plans.162 If a chronically ill enrollee leaves one plan for another, the provider would be required to make a payment to the new health plan. This would make firms less afraid to enroll chronically ill people since a payment would accompany the enrollee. It would also induce providers to cover chronic disease management to prevent enrollees from leaving.163
To further encourage participation in disease management and healthy behaviors, a state could provide a reverse health savings account, a type of flexible spending account that allows enrollees to earn credits in return for participating in programs that improve health.164 These noncash credits could be used to pay out-of-pocket costs. Florida is currently experimenting with this idea in its Medicaid reform plan.
Reducing the Cost of Private Insurance. As states continue to reform the ways in which they provide Medicaid services, they should also consider reform of private insurance regulations, since the rising cost of private insurance has affected both the number of Medicaid enrollees and the costs of health services across the board.
Direct state subsidies are a better way than community rating and guaranteed issue to cover patients who are uninsurable due to chronic health conditions. Thirty-two states have some type of high-risk pool for medically uninsurable residents. Those allowed to join generally have preexisting conditions that make insurance prohibitively expensive or impossible to obtain on their own, but they are not necessarily indigent or low-income. Each state program differs slightly and maximum lifetime benefits vary. Most have waiting lists to join or waiting periods before covering preexisting conditions. The pools are state-subsidized and are expected to lose money.165
Massachusetts Gov. Mitt Romney recently signed into law an innovative plan to insure at least 90 percent of the state’s residents. While the plan has its flaws, it also contains features to change the state’s Medicaid program and make private insurance more affordable. Massachusetts’ plan partially deregulates the small-group and individual health insurance markets in the state. Individuals between the ages of 19 and 26 will be able to purchase mandate-free insurance coverage with fewer benefits at a lower cost. The new law is based on the assumption that limited-benefit insurance is better than no insurance – especially for young people.
[page]“When patients have fi nancial incentives, they are better consumers.”
In the private sector, patients are increasingly required to directly share in the cost of health care. They also have increasing opportunities to make their own choices and manage their own health care dollars.166 This is the consumer-driven health care (CHDC) revolution. CDHC usually involves health plans in which a person pays some medical expenses directly, usually from a personal account established for that purpose. Evidence has shown that when individuals have the proper financial incentives, they will be better consumers of health care. A decade-long RAND study from the 1970s examined the effect of cost-sharing on the use of health care services. It found that individuals required to make a copayment for their care reduced their use of medical services, compared to those who received free care. After a decade, there were no significant differences in health among the two groups.167
Consumer-driven health accounts can also be used in Medicaid.
Health Opportunity Accounts. The Deficit Reduction Act allows 10 state Medicaid programs to set up five-year demonstration projects to provide Medicaid recipients with Health Opportunity Accounts (HOAs), similar to Health Savings Accounts (HSAs) used in the private sector.168 Proponents hope these accounts will create an awareness of health care costs and inject an element of consumerism into the purchase of medical services. The states that choose to participate will receive federal matching funds to contribute up to $1,000 per child and $2,500 per adult into the HOAs. HOAs can be used to purchase a variety of medical goods and services, and unused funds will be available for future use by participants. Moreover, if patients become ineligible for Medicaid, they have up to three years to use up to 75 percent of their HOA balances to purchase private health insurance.169 South Carolina, which had already applied for a HIFA waiver to restructure its Medicaid program, has applied to become one of the 10 states. [See the sidebar “Florida’s Consumer-Driven Medicaid Reforms.”]
A traditional objection to cash-balance accounts is the belief that the poor will forgo needed health care to accrue more cash; but unlike private-sector HSAs, the uses of personal health accounts could be limited. Through a debit card, a state could ensure that a recipient completed certain medical procedures such as child immunizations or prenatal care before accessing any of his or her HOA balance. The recipient could then use the remaining funds for specified health, social, child education or job training needs.
“Patients could use personal health accounts to purchase services.”
Enhanced Benefit Accounts. A new pilot program in Florida aims to improve outcomes by providing Medicaid enrollees with incentives to become actively involved in their care and treatment. Deposits will be made to personal accounts for enrollees who practice healthy lifestyles. They can use the funds to purchase health care goods and services not covered by their plan. A panel will ultimately decide which activities qualify for this “enhanced benefit credit,” but they will likely include such things as participating in wellness programs, obtaining annual immunizations, or partaking in disease management, smoking cessation and weight loss programs. Similar to HOAs, participants who leave Medicaid will have access to the funds for up to three years and can use them to pay premiums for private insurance.170
However, restricting HOAs and other benefit accounts to health care services may not be optimal. Those who find that their balances are greater than required for their health care needs would have an incentive to simply consume more health care services in order to fully utilize their accounts. Individuals should instead be able to convert health care services into credits that would go toward purchasing private health insurance.
Another objection to allowing Medicaid beneficiaries to exercise choice in health care providers is that the poor, elderly, blind and disabled either lack the ability to choose between plans or may be hoodwinked by unethical sales people. Although this may be true of certain populations, it isn’t true for most Medicaid recipients. Evidence shows that for certain services, the poor have just as much ability to choose as the middle class.171 Even individuals with mild cognitive disabilities can participate in decision-making regarding their own care if given the opportunity to do so, according to research by the San Francisco-based Family Caregiver Alliance. This might improve their satisfaction, since their preferences often differ from those of family caregivers.172
[page]Although long-term care is an optional benefit, it is one of the fastest growing areas of state Medicaid spending. Every state provides this benefit – and not just to the poor. Medicaid is paying for the long-term care of a growing number of middle-class seniors. When they retire, most Medicare enrollees do not meet Medicaid income and asset tests for long-term care coverage. However, Medicare has annual and lifetime maximum benefits for nursing home care, which it provides mainly for rehabilitation following injury, illness or surgery. Seniors in need of long-term care who max-out their Medicare coverage, or those who need custodial care rather than medical treatment, must pay out of pocket. Seniors who exhaust their assets paying for nursing home care may be eligible for Medicaid, if their incomes are low enough. This provides incentives for seniors to arrange their financial affairs just to meet asset and income tests for Medicaid long-term care benefits.
“Some seniors transfer assets to their children to qualify for Medicaid.”
There are several methods that allow individuals to legally impoverish themselves and qualify for Medicaid. They can 1) transfer assets to their children, 2) divorce, and 3) set up irrevocable (Miller) trusts. They must plan in advance and make financial arrangements several years before the need arises. When a state is determining eligibility, federal law allows it to “look back” and include as assets any funds that a senior transferred within five years of applying for long-term care benefits.173
An entire industry of attorneys practicing “elder law” has sprung up in recent years to help seniors transfer assets in order to qualify. However, it is difficult to identify abuses because most asset transfers by seniors are not made to skirt Medicaid asset tests. According to the 2002 Health and Retirement Study of the National Institute on Aging, one in five elderly households (22 percent) transferred assets in the prior two years.174
Seniors are often advised to have enough financial assets to pay for a year’s worth of care. Good-quality nursing homes can turn down individuals who rely solely on Medicaid for their long-term care and cannot pay for the first year. But once a year’s worth of assets are spent down, a nursing home cannot legally kick someone out.
A growing number of seniors have established Miller Trusts, also known as Qualified Income Trusts.175 Seniors may assign their investment income to the trust, which is designed to limit how the funds are distributed. Trust funds can be used to make certain payments including insurance premiums, support for a spouse and $60 per month for personal needs. These trusts effectively allow people to hold back income that otherwise would reduce Medicaid’s long-term care costs.
Encouraging Community Care over Institutional Care. Medicaid encourages institutional care over home care. Although many state programs are changing, they could increase their use of less-expensive home care.176 Home care often costs only half as much as a nursing home.177 In some high-cost areas, the cost savings from home care may be even greater. For instance, home care in Washington, D.C., costs less than one-third as much as nursing home care. In Manhattan, a year of home care costs only about one-fifth as much as a year-long stay in a nursing home.178 Home providers offer a range of medical services, including occupational or physical therapy.
Ohio, Oregon, Washington and Wisconsin expanded home- and community-based care to help control rapidly increasing institutional care expenditures. These states were able to serve more people while controlling the growth in overall long-term care spending. Between 1982 and 1992 the combined total of nursing home beds in the three states declined 1.3 percent, while total nursing facility beds nationwide increased 20.5 percent.179
“Reverse mortgages could be used to pay for nursing home care.”
Ohio’s Commission to Reform Medicaid has proposed rewarding families who choose lower-cost options that save the state money, such as care in the home or community. This would allow an elderly parent living with family members to receive a few hours of home or personal care per week that could delay their entry into a nursing home. The financial incentive could be to exclude some assets from eligibility tests or shield them from cost recovery.180
Private insurance is available to cover nursing home and in-home care, but few seniors purchase it. There are limited state programs to encourage more private coverage. A pilot project in New York, Connecticut, California and Indiana called the Partnerships for Long-Term Care (PLTC) provides financial incentives to purchase long-term care insurance. The plan allows people to shelter their assets by purchasing a qualifying private insurance policy with a defined amount of coverage. When a policyholder enters a nursing home, he or she first relies on the insurance. When the insurance is exhausted, special eligibility rules allow them to receive Medicaid benefits while retaining assets equal to the value of the policy.
In California and Connecticut Partnership programs, individuals purchase coverage from competing private insurers. For each dollar of coverage, they protect a dollar’s worth of assets. For instance, a long-term care policy with $120,000 in benefits allows an individual to shelter $120,000 in assets and still qualify for Medicaid long-term care. Since most nursing home stays are less than one year, very few of those who have purchased policies have applied for Medicaid benefits.
The Deficit Reduction Act allows all 50 states to establish partnership programs. Individuals who purchase such policies can access Medicaid benefits after their insurance runs out – without the means testing required for non-insured applicants.181
Encouraging the Use of Assets to Finance Long-Term Care. There are more than 13 million households headed by people aged 62 years or older. Many seniors own their homes but are reluctant to tap their equity to pay for nursing home care out of fear of losing their homes. However, they could obtain a reverse mortgage, which is a home loan that does not have to be repaid as long as the owner (which could include the spouse of a nursing home resident) lives in the house.182 More than six million of these households could access more than $72,000 in home equity using reverse mortgages.183 This would pay for a year or more of nursing home care and two or more years of home care in most areas. Currently, seniors rarely use reverse mortgages for long-term care. Why should they? Home equity is generally an exempt asset when qualifying for Medicaid long-term care. Since seniors can obtain long-term care without taking out a reverse mortgage, they have little reason to do so.
The solution is to remove the home-equity exemption and specify that seniors must first exhaust home equity using a reverse mortgage before qualifying for Medicaid long-term care.184 An added benefit is that more people may plan ahead and purchase long-term care insurance if they are not allowed to shelter their largest asset while still qualifying for Medicaid.
A home sales contract is similar to a reverse mortgage; it allows a senior couple to sell their home now, but live in it the rest of their lives. This would be appealing to married seniors and seniors who are getting rehabilitative care and expect to leave the nursing home.
“Long-term care insurance helps seniors shelter assets.”
Seniors with life insurance policies who enter a long-term care facility may qualify for viatical settlements to assist them with expenses. Viatical settlements are financial arrangements that allow terminally-ill individuals to sell their life insurance policies at a discount in return for cash. The purchasing firm pays less than face value (generally 50 percent to 80 percent) depending upon life expectancy. The purchaser pays any remaining premiums and assumes the risk for life expectancy. In other words, the insured is not penalized for living longer than expected. However, one problem is that not everyone qualifies for this arrangement. Insurers, providers and states use different definitions for what they consider terminal illness. For instance, seniors expected to live more than five years likely will not qualify for this arrangement.185
According to the Federal Trade Commission, there are also tax implications that can be quite complicated. Viatical settlements, where life expectancy is less than two years, are exempt from federal taxes – although some states do not provide this exemption.186
The federal government should facilitate viatical arrangements and life settlements for people facing long-term care, including limiting tax liability. It should require such arrangements for life insurance owned by individuals applying for Medicaid long-term care coverage. Transfer of ownership of life insurance policies should be treated the same way as other asset transfers.
Increasing Estate Recovery. When beneficiaries die, states can recover the cost of their nursing home care from their estates. That could include a house, for example, since a home is typically not included in assets for determining Medicaid eligibility. The Deficit Reduction Act now makes individuals ineligible for Medicaid nursing home coverage if their home equity value is greater than $500,000.187 Federal law also permits states to recover personal and real property in which the individual has an interest or legal title that aren’t included in the probated estate. Some states are aggressively pursing estate recovery, and all states receive federal funds to do so.188
Future legislation should require that any funds placed in qualified income trusts be considered income for determining Medicaid eligibility. It could even eliminate the use of trusts that reduce current income. Furthermore, property settlements in divorces made prior to Medicaid eligibility should be subject to the same five-year rule as other divisions of property.
“Children could be asked to contribute to their parents’ care.”
Holding Children Responsible for Their Parents’ Care. States should seek to recover current nursing home costs from beneficiaries’ families who are financially able to pay.189 About 30 states currently have filial responsibility statutes that require adult children to care for their indigent elderly parents. There is no uniform federal filial responsibility statute. The state statutes vary, but in general they force adult children to reimburse the state for programs or institutions that have cared for an indigent parent. States with filial responsibility statutes take a variety of approaches to enforcement: 21 allow some sort of civil court action to obtain financial support (or cost recovery) and 12 specify a criminal penalty for filial nonsupport; three states allow both civil and criminal actions. Children’s liability is limited under a variety of conditions. These include whether the adult child has enough income to actually contribute and if they were abandoned or deserted by the parent.
Medicaid costs could be reduced if states began to systematically enforce filial responsibility laws. When adult children understand they could be responsible for a portion of their indigent parents long-term care needs, they will have an incentive to encourage their parents to plan for the future.
A state could automatically consider an adult child able to pay toward care of an indigent parent unless they file a public notice that they are not responsible for the debts of the parent. Additionally, adult children who refuse to support their parents could be required to relinquish inheritance rights and rights to any trust set up for them by a parent.
[page]States can take many steps on their own to improve their Medicaid programs. The recently-passed Deficit Reduction Act is a good step in allowing states more flexibility in redesigning their Medicaid programs. But federal legislative changes are required to fundamentally reform the system.
Block Grant Federal Funds. In the 1990s there were proposals in Congress to give states more flexibility and responsibility through a block grant program.190 A report by the National Governors Association suggests an inflation-indexed block of money for long-term care. Each state would then decide who and how much to cover.191 This is a good idea for all portions of Medicaid.
Under the current system, every time a state wastes a dollar, at least half of that waste is paid for by the federal government. Every time a state eliminates a dollar of waste, at least half the savings stays in the state, while the remainder is realized in Washington, D.C. Block grants would allow states to realize the full benefits of every dollar saved and pay the full costs of every dollar of additional spending. Put differently, block grants would allow states to realize the full benefits of their good decisions and pay the full costs of their bad decisions.
“Medicaid funds could be block-granted to the states.”
In 2003, the Bush Administration proposed converting Medicaid’s federal match to a fixed block grant to the states.192 A block grant converts a defined benefit entitlement into a defined contribution. Under the former system, payments are based on the state’s willingness to spend. Under the latter, spending is based on the federal government’s willingness to pay. This is similar to how Congress allocates federal funds for state welfare programs. One of the advantages of a block grant is predictability.193 It would limit the federal government’s financial exposure while allowing states to design programs to meet their unique needs with maximum flexibility.
If five or six states requested a block grant, Congress would probably approve the request. However, some states are concerned that the federal government might renege on a block grant deal. One solution to this problem is to write into a pilot program the specific formula that would determine how much participating states receive. For example, if New York currently receives 13 percent of all federal Medicaid dollars, the agreement could specify that it would continue to receive 13 percent of all federal Medicaid dollars for the next few years.
A further advantage of the block grant approach is that all the funds the states currently receive would be at their disposal to allocate as they choose. Currently, Medicaid is a convoluted system of matching grants with separate pots of money for specific purposes. One of these pots is disproportionate share hospital (DSH) payments, which are designed to reimburse hospitals that care for a larger-than-average number of indigent patients. Texas is a perfect example of some of the ways this fractured funding distorts incentives.
In 2003, the Texas Legislature passed a law requiring the Texas Department of Health and Human Services (HHS) to provide Medicaid services in the most efficient manner possible. Subsequent research found Medicaid HMOs were the most cost-effective way. In early 2005 the director of HHS announced plans to expand a pilot project and place 400,000 Medicaid recipients into Medicaid HMOs for an estimated savings of $401 million dollars over two years. However, Texas HHS was fought by public hospitals that stood to lose DSH payments. They argued that they would lose more federal matching funds and state DSH funds than the proposed program would save.
A block grant would give a state the flexibility to use DSH payments to reimburse hospitals or use the funds to cover indigent patients in more efficient ways. Thus it would target funds to the most appropriate facility and pay for care only through the most efficient provider.194 For instance, a state could use the funds to reimburse neighborhood clinics or community hospitals rather than pay for expensive care in emergency rooms. It could also provide incentives for hospitals to provide indigent care in the most efficient manner rather than seek federal funds for care rendered in their emergency departments.
Allow Cost-Sharing. Copayments and increased cost-sharing have been used successfully by private health insurers for years to reduce unnecessary use of medical services.195 In the past, a state was only allowed to charge nominal copayments of $1 to $3 for medical services and prescription drugs, unless it received a waiver.196
The new Deficit Reduction Act (DRA), however, allows states to charge nominal copays for all nonpreferred prescription drugs for Medicaid recipients 150 percent or more above the federal poverty level. Furthermore, states are permitted to increase copays commensurate with rises in the medical component of the consumer price index, and they are not prohibited from requiring mandatory populations to make copayments for nonpreferred prescription drugs.197 The National Governors Association favors allowing states to require cost-sharing and copayments from both optional and mandatory populations of up to 5 percent of a family’s income. One way to apply this principle to Medicaid is to offer enrollees who wish to purchase a nonformulary drug the opportunity to receive the same drug if they make a higher copayment. If a physician thinks a nonformulary drug offers significant benefits, copayments could be waived.
The DRA also allows states to implement cost-sharing (through higher copays) for nonemergency services provided in an emergency room setting. However, cost-sharing should not be imposed for those services and treatments that have been shown to reduce preventable medical costs. States should, for example, provide first-dollar coverage for asthma treatments because hospitalizations for severe asthma attacks are costly, but can be easily prevented.198 But doctor visits for routine sore throats are almost always unnecessary; they occur so frequently because they cost the patient very little.
“Benefi ts could be tailored to fi t different patients’ needs.”
Allow Flexibility in Benefits among Medicaid Populations. Medicaid populations include old and young adults, children and individuals with special needs, such as the blind and disabled. One of the problems with providing benefits for mandatory populations is “comparability” – the requirement that everyone in a state eligible for Medicaid must have the same benefits. Prohibitions against tailoring benefits to individual needs often forces states to drop optional populations from their rolls in order to reduce costs, instead of simply reducing benefits for some populations that would not likely need them. Under the Deficit Reduction Act, however, states now have the flexibility to provide different benefits for different groups of Medicaid beneficiaries.
The governor of Kentucky recently announced a plan to cover the state’s current mandatory and optional Medicaid populations, but vary benefits based on the needs of four eligibility groups: the general adult Medicaid population, children, people with disabilities or needing institutional care, and the elderly. The new program will also provide incentives to encourage healthy behaviors similar to programs in West Virginia and other states and provide disease management benefits for those with chronic conditions such as diabetes. Kentucky’s Medicaid Commissioner estimates the program revisions will save the state $200 million over two years.199
Level the Playing Field for Individually-Purchased Private Health Insurance. Federal tax laws increase the cost of private health insurance, encouraging individuals who buy their own health policies to drop them. Most Americans receive private health coverage through employer-sponsored group health plans. Employer-paid premiums are tax-deductible as a business expense, and any premium payments the employee makes are paid with pretax dollars – which means they are not counted as taxable income and payroll taxes are not withheld. However, nearly 17 million people currently purchase insurance for themselves and their families in state-regulated individual insurance markets. Unlike employer plans, which are purchased with pretax dollars, individual health insurance is purchased with after-tax dollars, creating an unlevel playing field for those without employer-sponsored health insurance. The federal government should allow individuals to pay health insurance premiums with pretax dollars.200
“Federal tax laws increase the cost of private health insurance.”
Make Long-Term Care Premiums Tax-Deductible. Individual long-term care insurance is available from commercial carriers, but few seniors – and fewer working-age adults – purchase it, even though 40 percent of nursing home residents are under age 65. One reason is that long-term care insurance is not given the same tax treatment as employer-sponsored group health insurance.
People can use their health savings accounts (HSAs) as well as their flexible spending accounts (FSAs) to pay a limited amount of long-term care premiums tax free. Unfortunately, most Americans don’t have access to either HSAs or FSAs. And the amount of long-term care premiums that are nontaxable is limited based on age. For instance, individuals under 40 years of age can only deduct $260 per year while those 41 to 50 can deduct $490, 51- to 60-year-olds can deduct $980, 61- to 70-year-olds can deduct $2,600, and seniors over 70 can deduct $3,250.201 Long-term care premiums are a medical expense under section 213(d) of the tax code, but those expenses are only deductible to the extent that they exceed 7.5 percent of adjusted gross income.
The deductibility of premiums should not depend on adjusted gross income or age. Long-term care insurance is cheaper if purchased when young; full deductibility of premiums would encourage individuals to purchase coverage in advance of their need.
[page]“Medicaid reform is not simple, but it is essential.”
An alternative to uncontrolled Medicaid growth exists. It is not simple, and in many ways it is unsettling. It will require standing up to powerful interest groups. It will require dedicated staff. The alternative will not stop Medicaid budget growth, but it will lower the rate of that growth. It will provide policymakers with significantly greater control over costs and improve health outcomes. It will introduce some of the efficiency of the marketplace into Medicaid programs. And it will allow patients and providers to make more of their own decisions.
Out-of-control increases in Medicaid costs are not inevitable. But if reforms are not made soon, the question in a few years will be: Why didn’t policymakers take control of our destiny when they had the chance?
NOTE: Nothing written here should be construed as necessarily reflecting the views of the National Center for Policy Analysis or as an attempt to aid or hinder the passage of any bill before Congress.
[page]

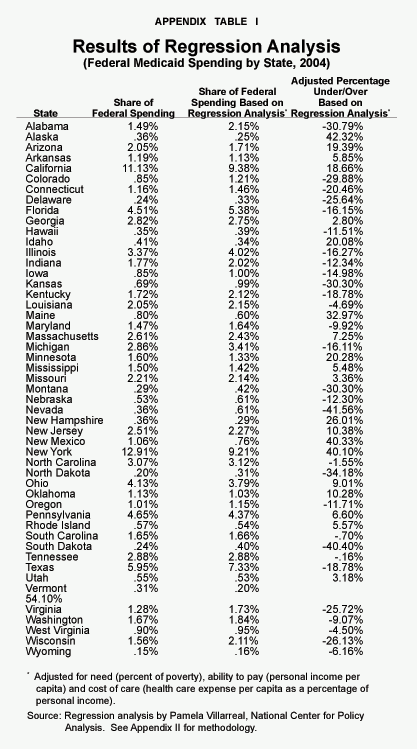



- “The Fiscal Survey of States,” National Governors Association and National Association of State Budget Officers, June 2005.
- Ibid. Medicaid and other health expenses already account for about 22 percent of state spending.
- Vernon Smith et al., “The Continuing Medicaid Budget Challenge: State Medicaid Spending Growth and Cost Containment in Fiscal Years 2004 and 2005, Results from a 50-State Survey,” Kaiser Commission on Medicaid and the Uninsured, Kaiser Family Foundation, October 2004.
- Centers for Medicare and Medicaid Services, Office of the Actuary, National Health Statistics Group, “National Health Expenditures Aggregate and Per Capita Amounts, 1960-2004,” U.S. Department of Commerce, Bureau of Economic Analysis and U.S. Bureau of the Census.
- Enrollment is expected to grow an average of about 4 percent annually through 2006. See “The Fiscal Survey of States,” National Governors Association and National Association of State Budget Officers, June 2005.
- “The Uninsured in America,” Blue Cross Blue Shield Association, February 27, 2003. Estimates of eligibility for public health care programs vary.
- Raymond C. Scheppach, Executive Director, National Governors Association, statement before the Medicaid Commission on Short-Term Medicaid Reform, August 17, 2005.
- “Changes in Participation in Means-Tested Programs,” Congressional Budget Office, Economic and Budget Issue Brief, April 2005. Available at http://www.cbo.gov/ftpdocs/63xx/doc6302/04-20-Means-Tested.pdf; “Change in Number of AFDC/TANF Recipients – Fiscal Years 1996-2002,” Table 1:11:a, U.S. Department of Health and Human Services, Office of Family Assistance, May 13, 2004. Available at http://www.acf.hhs.gov/programs/ofa/annualreport6/chapter01/0111a.htm. Access verified May 1, 2006.
- “Medicaid: An Overview of Spending on ‘Mandatory’ vs. ‘Optional’ Populations and Services,” Kaiser Commission on Medicaid and the Uninsured, Kaiser Family Foundation, June 2005. Available at http://www.nfprha.org/uploads/KFFMandatoryvOptionalBrief.pdf. Access verified June 1, 2006.
- Based on 2002 estimates from “Medicaid Expenditures for Dual Eligibles (full and partial) by State, 2002,” Kaiser Commission on Medicaid and the Uninsured, Kaiser Family Foundation. Available at http://www.kff.org/medicaid/7024.cfm. Access verified January 4, 2006. See also John Holahan and Brian Bruen, “Medicaid Spending: What Factors Contributed to the Growth between 2000 and 2002?” Kaiser Commission on Medicaid and the Uninsured, Kaiser Family Foundation, September 2003.
- Potential medical providers, including physicians and clinics, were called by surveyors who posed variously as Medicaid, uninsured or insured patients seeking an appointment for a specific condition with a set of symptoms. The conditions described by the callers are considered medically urgent. Attempted access was considered successful when the caller was able to schedule an appointment within seven days. The surveys were conducted in major, geographically-dispersed urban areas. Brent R. Asplin et al., “Insurance Status and Access to Urgent Ambulatory Care Follow-Up Appointments,” Journal of the American Medical Association, Vol. 294, No. 10, September 14, 2005, pages 1,248-54.
- Outside of New York City, Medicaid uses traditional managed care organizations. See Richard Pérez-Peña, “At Clinic, Hurdles to Clear Before Medicaid Care,” New York Times, October 17, 2005.
- Richard Pérez-Peña, “Trying to Get, and Keep, Care Under Medicaid,” New York Times, October 18, 2005.
- Allison Sherrym, “Doctors Say Colorado Hospital Is Refusing Poor Patients,” Denver Post, October 22, 2003.
- Heath Foster, “Low-Income Patients Left Waiting for Care,” Seattle Post-Intelligencer, January 26, 2004.
- Presumably, these plans are able to pay more because of other cost-reducing efficiencies.
- “2004 Medicaid Managed Care Enrollment Report,” Centers for Medicare and Medicaid Services, 2004, page 3, table, “Managed Care Trends.” Available at http://www.cms.hhs.gov/MedicaidDataSourcesGenInfo/downloads/mmcer04.pdf . Access verified July 11, 2006.
- “Medicaid Managed Care Penetration Rates and Expansion Enrollment by State: Penetration Rates as of December 31, 2004,” Center for Medicare and Medicaid Services. Available at http://www.cms.hhs.gov/MedicaidDataSourcesGenInfo/downloads/mmcpr04.pdf. Access verified July 11, 2006.
- Richard Pérez-Peña, “Trying to Get, and Keep, Care Under Medicaid.”
- However, these plans cannot use the techniques private plans use to control utilization and costs – such as requiring preauthorization of services and having patient copays and deductibles.
- “Medicaid: An Overview of Spending on ‘Mandatory’ versus ‘Optional’ Populations and Services,” Kaiser Commission on Medicaid and the Uninsured, Kaiser Family Foundation, June 2005.
- “HIFA: Will It Solve the Problem of the Uninsured?” National Health Law Program, Health Insurance Flexibility and Accountability (HIFA) Talking Points, February 28, 2002. Available at http://www.healthlaw.org. Access verified August 14, 2006.
- Pamela Villarreal, “Federal Medicaid Funding Reform,” National Center for Policy Analysis, Brief Analysis No. 566, July 31, 2006.
- For a discussion of factors that influence state Medicaid spending see Robert J. Buchanan, Joseph C. Cappelleri and Robert L. Ohsfeldt, “The Social Environment and Medicaid Expenditures: Factors Influencing the Level of State Medicaid Expenditures,” Public Administration Review, Vol. 51, No. 1, January/February 1991, pages 67-73.
- See Appendix II and Appendix Table I. Regression analysis by Pamela Villarreal, National Center for Policy Analysis, is based on U.S. Census data and Medicaid data from the Kaiser Family Foundation.
- “Medicaid’s architects envisioned a program that would provide poor people with mainstream medical care in a fashion similar to that of private insurance. As the decades have passed, that vision has largely faded…poor people continue to rely on providers that make up the nation’s medical safety net: public and some not-for-profit hospitals and clinics [that] by virtue of their location or social calling provide a disproportionate amount of care to the poor.” John K. Iglehart, “The American Health System-Medicaid,” New England Journal of Medicine, Vol. 340, No. 9, February 4, 1999, pages 403-408.
- Medicaid spending per recipient varied from $4,425 to $2,101, a difference of about $2,300. Adding spending on free care for the uninsured to Medicaid spending reduced the variation in health care spending to less than $1,200. See John C. Goodman, “Minority Report of the Texas Blue Ribbon Task Force on the Uninsured,” in Sen. Chris Harris (Chairman) and the Members of the Texas Blue Ribbon Task Force on the Uninsured, “Texas Blue Ribbon Task Force on the Uninsured,” Report to the 77th Legislature, State of Texas, February 2001, page 42.
- The difference among groups receiving “good” care ranged from 56.6 percent of women to 53.1 percent for those with annual incomes of less than $15,000. Researchers examined 439 indicators for quality of care in four areas: screening, diagnosis, treatment and follow-up. Steven M. Asch et al., “Who Is at Greatest Risk for Receiving Poor-Quality Health Care?” New England Journal of Medicine, Vol. 354, No. 11, March 16, 2006, pages 1,147-55.
- For instance, it was widely assumed that the 1996 welfare reforms, which limited the eligibility of immigrants for Medicaid, would increase the uninsured rate of that population. Instead, the immigrant uninsured rate fell slightly as more immigrants purchased private insurance. See George Borjas, “Welfare Reform, Labor Supply, and Health Insurance in the Immigrant Population,” Journal of Health Economics, Vol. 22, No. 6, November 2003, pages 933-58.
- However, the loss of private insurance is likely to cause a small, offsetting increase in government revenues as employers substitute taxable wages for previously untaxed health benefits.
- David M. Cutler and Jonathan Gruber, “Does Public Insurance Crowd Out Private Insurance?” Quarterly Journal of Economics, Vol. 111, No. 2, May 1996, pages 391-430. Also see Tanya T. Alteras, “Understanding the Dynamics of ‘Crowd-Out’: Defining Public/Private Coverage Substitution for Policy and Research,” Academy for Health Services Research and Health Policy, prepared for the Robert Wood Johnson Foundation’s Changes in Health Care Financing and Organization Program, June 2001, pages 14-15; and RAND Health, “State Efforts to Insure the Uninsured: An Unfinished Story,” RAND, Research Highlights, 2005.
- David M. Cutler and Jonathan Gruber, “Does Public Insurance Crowd Out Private Insurance?” Quarterly Journal of Economics, Vol. 111, No. 2, May 1996, pages 391-430. Cutler and Gruber found that most of the reduction came from workers deciding to drop private coverage (particularly for dependents) rather than because their employers stopped insurance coverage.
- Peter J. Cunningham and Michael H. Park, “Recent Trends in Children’s Health Insurance: No Gains for Low-Income Children,” Center for Studying Health System Change, Issue Brief No. 29, April 2000.
- Based on NCPA calculations comparing 1997 to 2003 data. See HSC Community Tracking Surveys, 1997 to 2003, Center for Studying Health System Change.
- Bradley C. Strunk and James D. Rescholsky, “Trends in U.S. Health Insurance Coverage, 2001-2003,” Center for Studying Health System Change, Tracking Report No. 9, August 2004.
- Janet Currie and Jonathan Gruber, “Health Insurance Eligibility, Utilization of Medical Care, and Child Health,” Quarterly Journal of Economics, Vol. 111, No. 2, May 1996, pages 431-66.
- “Learning from SCHIP and Learning from SCHIP II,” Agency for Health Care Policy Research, June 1998.
- See Janet Currie and Jonathan Gruber, “Saving Babies: The Efficacy and Cost of Recent Expansions of Medicaid Eligibility for Pregnant Women,” Journal of Political Economy, Vol. 104, No. 6, December 1996, pages 1,263-96.
- See Janet Currie and Jonathan Gruber, “Health Insurance Eligibility, Utilization of Medical Care, and Child Health,” National Bureau of Economic Research, NBER Working Paper No. 5052, March 1995.
- Laura-Mae Baldwin et al., “The Effect of Expanding Medicaid Prenatal Services on Birth Outcomes,” American Journal of Public Health, Vol. 88, No. 11, November 1998, pages 1,623-29.
- “Increased Access to Medicaid Had Little Effect on Pregnancy Care or Outcome,” Project Report, Effect of Expanding Medicaid Coverage on Health Outcomes, Robert Wood Johnson Foundation, January 2001. Available at http://www.rwjf.org/reports/grr/019672.htm. Access verified August 26, 2005.
- Jonathan Gruber and Aaron Yelowitz, “Public Health Insurance and Private Savings,” Journal of Political Economy, Vol. 107, No. 6, part 1, December 1999, page 1,259.
- Michael F. Cannon, “Medicaid’s Unseen Costs,” Cato Institute, Policy Analysis No. 548, August 18, 2005.
- Shawna Orzechowski and Peter Sepielli, “Net Worth and Asset Ownership of Households: 1998 and 2000,” U.S. Census Bureau, Current Population Reports, P70-88, May 2003, page 11, Table F.
- See the discussion in the section “Paying for Long-Term Care.”
- “2004 State Expenditure Report,” National Association of State Budget Officers, 2005. Available at http://www.nasbo.org/Publications/PDFs/2004ExpendReport.pdf. Access verified August 10, 2006.
- NCPA analysis by Pamela Villarreal, based on the American Chamber of Commerce Research Association (ACCRA) cost of living index for the 2nd quarter of 2004 and figures for Medicaid spending. ACCRA compiles a quarterly cost of living index based on comparative survey data from various metropolitan and micropolitan areas. The index measures the cost of living based on a basket of goods, such as housing, groceries, health care and utilities, and are weighted according to government survey data on expenditure patterns.
- Denise Soffel, “Federal Medicaid Reform: What’s at Risk for New York,” Community Service Society, Policy Brief No. 11, June 2003.
- Data from Centers for Medicare and Medicaid Services; accessed December 2005. Population figures from the Census Bureau, U.S Department of Commerce.
- Tarren Bragdon, “Maine’s State-Run Health Plan Faltering,” Heartland Institute, January 1, 2006. Also, see “Maine and the United States,” State Medicaid Fact Sheets, Kaiser Family Foundation; available at http://www.kff.org/mfs/medicaid.jsp?r1=ME&r2=US; accessed on May 4, 2006.
- Tarren Bragdon, “Maine’s State-Run Health Plan Faltering,” Heartland Institute, January 1, 2006.
- “Confronting the Tradeoffs in Medicaid Cost Containment,” Citizens Budget Commission (New York), February 2004. Available at http://www.cbcny.org/medicaid04.pdf. Access verified December 22, 2005.
- “Distribution of Medicaid Spending by Service FY2004,” StateHealthFacts.org, Kaiser Family Foundation, 2004.
- Ibid.
- “2002 State and National Medicaid Enrollment and Spending Data (MSIS)” Kaiser Commission on Medicaid and the Uninsured, March 24, 2006, table 1a. Available at http://www.kff.org/medicaid/upload/kcmu032106atable1a.pdf; and “Quantitative Analysis of New York State Medicaid Spending,” Health Economics and Outcomes Research Institute, Greater New York Hospital Association, October 24, 2003.
- Jeff Clabaugh, “D.C. Nursing Homes among Nation’s Priciest,” Washington Business Journal, August 4, 2003.
- Alan Johnson et al., “Nursing-Home Industry Has Clout; Lobby Again Surfs Plans for Cuts in Governor’s Budget,” Columbus Dispatch, April 17, 2005.
- Allen J. LeBlanc, M. Christine Tonner and Charlene Harrington, “State Medicaid Programs Offering Personal Care Services,” Health Care Financing Review, Vol. 22, No. 4, Summer 2001, page 157.
- Robyn I. Stone, “Long-Term Care for the Elderly with Disabilities: Current Policy, Emerging Trends, and Implications for the Twenty-First Century,” Milbank Memorial Fund, August 2000.
- Allen J. LeBlanc, M. Christine Tonner and Charlene Harrington, “State Medicaid Programs Offering Personal Care Services,” Health Care Financing Review, Vol. 22, No. 4, Summer 2001, page 155. Also see “Confronting the Tradeoffs in Medicaid Cost Containment,” Citizens Budget Commission (New York), February 2004. Available at http://www.cbcny.org/medicaid04.pdf.
- Allen J. LeBlanc, M. Christine Tonner and Charlene Harrington, “State Medicaid Programs Offering Personal Care Services,” page 162.
- Ibid, page 163.
- Federal regulations require that states must provide access to transportation to and from Medicaid-related appointments, although the law gives wide latitude in how they implement transportation services. See “Medicaid Transportation: Assuring Access to Health Care; A Primer for States, Health Plans, Providers and Advocates,” Community Transportation Association of America, January 2001.
- Clifford J. Levy and Michael Luo, “New York Medicaid Fraud May Reach into Billions,” New York Times, July 18, 2005.
- Ibid.
- Direct Research LLC, “Medicare Physician Payment Rates Compared to Rates Paid by the Average Private Insurer, 1999-2001,” Medicare Payment Advisory Commission, No. 03-6, August 2003.
- “Kansas Medicaid Facts,” American Academy of Pediatrics, July 2005.
- See Stephen Zuckerman et al., “Changes in Medicaid Physician Fees, 1998-2003: Implications for Physician Participation,” Health Affairs, Web Exclusive, June 23, 2004.
- Ibid.
- Based on provider fee schedules obtained from New York State Department of Health and Mississippi Envision.
- Laurence C. Baker and Anne Beeson Royalty, “Medicaid Policy, Physician Behavior, and Health Care for the Low-Income Population,” Journal of Human Resources, Vol. 35, No. 3, Summer 2000, pages 480-502.
- “Medicaid Watch ‘05,” Public Policy Institute of New York State, Issue No. 4, March 24, 2005.
- A panel modeled after the federal military base closure commission has been established to recommend hospitals and nursing homes for closure, consolidation or merger, and is due to report December 1, 2006. Raymond Hernandez and Al Baker, “Close Hospitals, Pataki Says in Medicaid Cost Proposal,” New York Times, March 17, 2005. See the Commission on Health Care Facilities in the 21st Century. Available at http://www.gnyha.org/pubinfo/chcf/CHCF_Origin_Mission.pdf. Access verified March 15, 2006.
- Analysis of Medicaid spending on inpatient care. See Kaiser Family Foundation Web site www.StateHealthFacts.org.
- Kathleen M. King, “Medicaid: States’ Payments for Outpatient Prescription Drugs,” U. S. Government Accountability Office, Report GAO-06-69R, October 31, 2005, page 12.
- Clifford J. Levy and Michael Luo, “New York Medicaid Fraud May Reach into Billions,” New York Times, July 18, 2005.
- Linda Gorman, “Medicaid Drug Formularies: Do They Perform as Advertised?” Health Care Policy Center, Independence Institute, Issue Paper No. 2-2002, April 2002.
- Frank Lichtenberg, “Benefits and Costs of Newer Drugs: An Update,” National Bureau of Economic Research, NBER Working Paper No. 8996, June 2002.
- Linda Gorman, “Medicaid Drug Formularies: Do They Perform as Advertised?” Health Care Policy Center, Independence Institute, Issue Paper No. 2-2002, April 2002.
- Ibid.
- This excludes Tennessee’s program, where 100 percent of enrollees are in TennCare. “Medicaid Managed Care Penetration Rates and Expansion Enrollment by State: Penetration Rates as of December 31, 2004,” Center for Medicare and Medicaid Services. Available at http://www.cms.hhs.gov/MedicaidDataSourcesGenInfo/downloads/mmcpr04.pdf.
- Ibid.
- See Robyn Tamblyn et al., “Adverse Events Associated with Prescription Drug Cost-Sharing Among Poor and Elderly Persons,” Journal of the American Medical Association, Vol. 285, No. 4, January 24/31, 2001, pages 421-29. Tamblyn found that after Quebec implemented a cost-sharing policy in 1996 using co-insurance deductibles of $100 annually and 25 percent prescription copays for beneficiaries who were previously receiving free medication, the use of essential drugs fell 9 percent among the elderly and 14 percent among the poor. Emergency room visits increased 14 percent among the elderly and 54 percent among the poor.
- See “State Law Requiring Medicaid Copays Violates Federal Law, State Court Decides,” Health Care Policy, Vol. 13, No. 38, September 26, 2005; Also, see “Michigan Medicaid Beneficiaries Who Cannot Make Copays Must Receive Drugs, U.S. Judge Rules,” Medical News Today, March 22, 2006; Available at www.medicalnewstoday.com.
- Betsy McCaughey, “Unnecessary Deaths: The Human and Financial Costs of Hospital Infections,” Committee to Reduce Infection Deaths and the National Center for Policy Analysis, December 2005.
- A ground-breaking hospital study in the 1960s showed that treatment caused complications in one out of five patients, and about 7 percent of the complications were fatal. See Elihu Schimmel, “The Hazards of Hospitalization,” Annals of Internal Medicine, January 1964, pages 100-110.
- “Medical Errors: The Scope of the Problem,” Agency for Healthcare Research and Quality, U. S. Department of Health and Human Services, Fact Sheet, Publication No. AHRQ 00-P037, February 2000. Available at http://www.ahrq.gov/qual/errback.htm.
- Kohn, Corrigan and Donaldson, eds., To Err is Human: Building a Safer Health System, page 52.
- Marlene R. Miller and Chunliu Zhan, “Pediatric Patient Safety in Hospitals: A National Picture in 2000,” Pediatrics, Vol. 113, No. 6, June 2004, pages 1741-46.
- Ibid.
- J.H. Gurwitz et al., “Incidence and Preventability of Adverse Drug Events in Nursing Homes,” American Journal of Medicine, Vol. 109, No. 2, August 1, 2000, pages 166-68.
- Betsy McCaughey, “Unnecessary Deaths: The Human and Financial Costs of Hospital Infections,” Committee to Reduce Infection Deaths and the National Center for Policy Analysis, December 2005. Available at http://www.ncpathinktank.org/pub/special/pdf/RIDBooklet_120605.pdf.
- See Thomas T. Yoshikawa, “Editorial Viewpoint: Antibiotic-Resistant Pathogens in Geriatric Care,” Annals of Long-Term Care, Vol. 6, No. 3, March 1998; and Lynn L. Chilton, “Infections and Antimicrobial Resistance in the Elderly Living in Long-term Care Settings,” MedScape Today, September 29, 2004; Available at http://www.medscape.com/viewarticle/493678. Access verified July 11, 2006.
- Leslie G. Aronovitz, “Medicaid Fraud and Abuse: Stronger Action Needed to Remove Excluded Providers from Federal Health Programs,” U.S. Government Accountability Office, GAO/HEHS-97-63, March 1997.
- Maurice Passley, Bonita Brodt and Tim Jones, “Medicaid: System in Chaos,” a series in nine parts, Chicago Tribune, October 31-November 9, 1993.
- Patrick D. Hansen, “Medicaid Transportation Provider Sentenced for Fraud,” Roger A. Heaton, U.S. Attorney, Central District of Illinois, United States Attorney’s Office, December 16, 2005.
- Paul Loriquet, “Essex County Owner of Invalid Transportation Company Sentenced to Jail for Medicaid Fraud,” Office of the Attorney General, New Jersey Department of Law and Public Safety, November 1, 2002.
- Clifford J. Levy and Michael Luo, “New York Medicaid Fraud May Reach into Billions,” New York Times, July 18, 2005.
- “Supplemental Security Income: Action Needed on Long-Standing Problems Affecting Program Integrity,” Report to the Commissioner of Social Security, U.S. Government Accountability Office, GAO Report HEHS-98-158, September 1998.
- Victoria Craig Bunce, J.P. Wieske and Vlasta Prikazsky, “Health Insurance Mandates in the States, 2006,” Council for Affordable Health Insurance, March 2006.
- Gail A. Jensen and Michael Morrisey, “Mandated Benefit Laws and Employer-Sponsored Health Insurance,” Health Insurance Association of America, January 25, 1999.
- In August 2001, under authority granted by Congress, the Centers for Medicare and Medicaid Services (CMS), formerly known as the Health Care Financing Administration (HCFA), announced the Health Insurance Flexibility and Accountability (HIFA) Demonstration Initiative.
- Clarke Cagey, “Health Reform, Year Seven: Observations about Medicaid Managed Care,” Centers for Medicare and Medicaid Services, Health Care Financing Review, Vol. 22, No. 1, Fall 2000, page 127. Available at http://www.hcfa.gov/Med-icaid/obs7.htm.
- John C. Fortney, “VA Community-Based Outpatient Clinics: Access and Utilization Performance Measures,” Medical Care, Vol. 40, No. 7, July 2002, pages 561-69.
- “Avoidable Hospitalizations in Pennsylvania,” Pennsylvania Health Care Cost Containment Council, Research Brief, Issue No. 3, November 2004.
- “West Virginia and Kentucky Alter Medicaid,” Associated Press, May 23, 2006.
- “Analysis and Description of the Governor’s 2005-2006 State Budget and Health Care Reform Act Proposals,” Healthcare Association of New York State, January 21, 2005. Available at http://cumc.columbia.edu/dept/gc/issues/docs/01-20-05budgetattachmenttoElertFINAL.doc. Access verified July 11, 2006. Gov. Pataki’s proposal to selectively contract for certain services has not been implemented. The most recent regulations still use the old system of DRGs, SIWs and Trimpoints.
- See, for example, Edwin Rubenstein, “Emergency Surgery for Medicaid,” Manhattan Institute, City Journal, Spring 1991.
- Texas Comptroller of Public Accounts, “Chapter 6: Health and Human Services,” in Challenging the Status Quo toward Smaller, Smarter Government, Texas Performance Review, Vol. 2, March 1999.
- James C. Robinson and C. S. Phibbs, “An Evaluation of Medicaid Selective Contracting in California,” Journal of Health Economics, Vol. 8, No. 4, 1989, pages 437-55.
- Jack Zwanziger, Glenn A. Melnick and Anil Bamezai, “The Effect of Selective Contracting on Hospital Costs and Revenues,” Health Services Research, October 2000.
- Kala Ladenheim et al., “Chapter 10: Selective Contracting,” in “Medicaid Cost Containment: A Legislator’s Tool Kit,” National Conference of State Legislatures. Available at http://www.ncsl.org/programs/health/forum/cost/strat10.htm; Access verified August 9, 2006.
- “The Value of Pharmacy Benefit Management and the National Cost Impact of Proposed PBM Legislation,” Pharmaceutical Care Management Association, July 2004. Available at http://www.pcmanet.org/research/istudies/PricewaterhouseCoopers_Report_V.pdf. Access verified July 7, 2006.
- Assembly Bill 2766, Senate Bill 2894 and Assembly Bill 6934 are similar in that they would prevent insurers from requiring prescription drugs be purchased through a mail-order pharmacy. This is referred to as the “employee’s mail order pharmacy bill of rights.”
- Testimony to the House Energy and Commerce Committee by Craig L. Fuller, President & CEO, National Association of Chain Drug Stores, June 22, 2005.
- Michael A. Fischer and Jerry Avorn, “Potential Savings from Increased Use of Generic Drugs in the Elderly: What the Experience of Medicaid and Other Insurance Programs Means for a Medicare Drug Benefit,” Pharmaceoepidemiology and Drug Safety, Vol. 13, 2004, pages 207-14. The data examined included 358,965 brand-name prescriptions (for which FDA-approved generic substitutes were available) among 80,000 patients. The study only examined A-rated generic drugs, which are defined as both biologically and pharmaceutically equivalent by the U.S. Food and Drug Administration.
- Some scientists would say it is pharmacologically the same. See Sylvester J. Schieber, “Why Coordination of Health Care Spending and Savings Accounts Is Important,” Watson Wyatt Worldwide, July 2004.
- The price for Clarinex is for 90 doses from Wal-Mart accessed online at destinationrx.com, and the price for Claritin is for 60 doses from Costco.com. The price for the generic version of Claritin (Loratadine) is from Sam’s Club. All prices surveyed May 24, 2006.
- If approved, the OTC dose of Orlistat will be half that of the prescription version. A 60mg dose has about 85 percent of the effectiveness of the 120mg prescription dose, however. Many private insurers do not cover the cost of Orlistat. Many state Medicaid programs may not cover it as well. See Christopher Snowbeck, “Glaxo Seeks Approval to Sell Obesity Drug Over the Counter,” Pittsburgh Post-Gazette, January 23, 2006.
- Linda Gorman, “Medicaid Drug Formularies,” Independence Institute, Issue Paper 2-2002, April 2002.
- Brian Abery, Rhonda Cady and Erin Simunds, “Health Care Coordination for Persons with Disabilities: Its Meaning and Importance,” Institute on Community Integration, University of Minnesota, Impact, Vol. 18, No. 1, 2005. Available at http://ici.umn.edu/products/impact/181/over5.html. Access verified August 15, 2006.
- Salynn Boyles, “Too Many Elderly Are Taking Dangerous Drugs,” WebMD Medical News, August 9, 2004; Lesley H. Curtis et al., “Inappropriate Prescribing for Elderly Americans in a Large Outpatient Population,” Archives of Internal Medicine, Vol. 164, No. 15, August 9/23, 2004.
- Christopher Tedeschi, “Pill Overkill,” USC Health & Medicine, Summer 1996.
- Description of MainNET, Muskie School of Public Service, University of Southern Maine. Available online at http://muskie.usm.maine.edu/projectbriefs/MaineNET.jsp.
- According to the Disease Management Association of America, “disease management is a system of coordinated healthcare interventions and communications for populations with conditions in which patient self-care efforts are significant.” Disease Management Association of America. Available at http://www.dmaa.org/definition.html. Access verified January 20, 2006.
- For instance, an asthma self-management plan could stipulate that if a patient’s “peak airflow” falls to 80 percent of their personal best peak airflow, they should increase medications at a pre-established rate and schedule a physician appointment. Patients should go to the emergency room if their peak airflow falls below 50 percent. See “Take Control – Q&A to Having a Self Management Plan,” AsthmaAssistant.com.
- Claudia Williams, “Medicaid Disease Management: Issues and Promises,” Kaiser Commission on Medicaid and the Uninsured, September 2004.
- Susan Konig, “Medicaid Reform: Florida, South Carolina Lead the Way,” Heartland Institute, August 1, 2005.
- “2005 Performance Report for Utah Commercial HMOs and Medicaid and SCHIP Health Plans,” Utah Department of Health, November 2005.
- Susan L. Norris, Michael M. Engelgau and K. M. Venkat Narayan, “Effectiveness of Self-Management Training in Type 2 Diabetes,” Diabetes Care, March 2001.
- Ibid.
- “Economic and Health Costs of Diabetes,” Agency for Healthcare Research and Quality, U.S. Department of Health and Human Services, Healthcare Cost and Utilization Project Highlights, No. 1, AHRQ Pub. No. 05-0034, January 2005.
- Teresa Pearson, “Getting the Most from Health-Care Visits,” Diabetes Self-Management, March/April 2001.
- Patti Bazel Beil and Laura Hieronymus, “Money-Saving Tips: Supplies, Nutrition, and Exercise,” Diabetes Self-Management, March/April 1999.
- Tjard R. Schermer et al., “Randomized Controlled Economic Evaluation of Asthma Self-Management in Primary Health Care,” American Journal of Respiratory and Critical Care Medicine, Vol. 166, No. 8, August 2002, pages 1062-72. For an evaluation of direct medical treatment costs for asthma, see Michael T. Halpern et al., “Asthma: Resource Use and Costs for Inhaled Corticosteroid vs. Leukotriene Modifier Treatment – A Meta-Analysis,” Journal of Family Practice, Vol. 54, No. 5, May 23, 2005.
- “Asthma Overview,” Web site document, Asthma and Allergy Foundations of America. Available at http://www.aafa.org/display.cfm?id=8&cont=5. Access verified August 10, 2006.
- Li Yan Wang, Yuna Zhong and Lani Wheeler, “Direct and Indirect Costs of Asthma in School-Age Children,” Preventing Chronic Disease, Vol. 2, No. 1, January 2005.
- Ibid. Implementation costs were mostly incurred in year one and amounted to about $200.
- Susan Konig, “Florida Medicaid Plan Receives Federal Approval,” Heartland Institute, Health Care News, January 1, 2006.
- See “Medicaid Managed Care: Four States’ Experiences with Mental Health Carve-Out Programs,” U.S. Government Accountability Office, GAO/HEHS-00-118, September 1999.
- Jeffrey S. Crowley, “An Overview of the Independence Plus Initiative to Promote Consumer-Direction of Services in Medicaid,” Kaiser Commission on Medicaid and the Uninsured, Henry J. Kaiser Family Foundation, Issue Paper 4151, November 2003.
- Ibid. While “cash and counseling” is the term commonly used, states may have slightly different programs with different names.
- Leslie Foster et al., “Does Consumer Direction Affect the Quality of Medicaid Personal Assistance in Arkansas?” Mathematica Policy Research, Inc., March 2003.
- James Frogue, “The Future of Medicaid: Consumer-Directed Care,” Heritage Foundation, Backgrounder No. 1618, January 10, 2003. Available at http://www.heritage.org/research/healthcare/BG1618.cfm. Access verified August 10, 2006.
- The National Academy of Sciences recommends that all federal health programs begin paying for quality care rather than for services rendered. See Janet M. Corrigan, Jill Eden and Barbara M. Smith, eds., Leadership by Example: Coordinating Government Roles in Improving Health Care Quality (Washington, D.C.: National Academies Press, 2002).
- Eric Henley, “Pay-for-Performance: What Can You Expect?” Journal of Family Practice, Vol. 54, No. 7, July 2005.
- John W. Rodat, “Pay for Performance – What’s Going On?” Signal Health, December 15, 2005. Available at http://www.signalhealth.com/node/512. Access verified January 17, 2006.
- Michael L. Millenson, Demanding Medical Excellence: Doctors and Accountability in the Information Age (Chicago: University of Chicago Press, 1997). An example of the possible magnitude of savings is shown by a study reported in Employee Benefit News, which estimates that the cost of poor-quality health care services is $1,350 per employee. If even a fraction of that amount can be saved per Medicaid recipient, hundreds of millions or even billions of dollars in taxes can be saved. See Craig Gunsauley, “Estimate: 30 percent of Health Spending Is Wasted,” Employee Benefit News, August 1, 2002.
- Joel B. Finkelstein, “Patient Safety Laboratories: States Pave the Way for a National Effort,” AMNews, January 3/10, 2005; Available at http://www.ama-assn.org/amednews/2005/01/03/gvsa0103.htm. Access verified on July 11, 2005.
- David M. Cutler, Robert Huckman and Mary Beth Landrum, “The Role of Information in Medical Markets: An Analysis of Publicly Report Outcomes in Cardiac Surgery,” National Bureau of Economic Research, NBER Working Paper w10489, May 2004.
- “H.R. 2334, 21st Century Health Information Act of 2005,” Thomas, Library of Congress. Available online at http://thomas.loc.gov/cgi-bin/query/z?c109:H.R.2234: Accessed on May 31, 2006.
- This database is referred to as a Medicaid provider information exchange. See Sarah F. Jaggar, “Medicare and Medicaid: Opportunities to Save Program Dollars by Reducing Fraud and Abuse,” U.S. Government Accountability Office, GAO/T-HEHS-95-110, March 22, 1995.
- Communication from Jim McDermott of Salient Corporation. To learn more about their software, see http://www.salient.com/Medicaid.pdf. Access verified January 12, 2006.
- Steven Malanga, “How to Stop Medicaid Fraud,” Manhattan Institute, City Journal, Spring 2006.
- Office of the Governor (State of Kansas), “Sebelius says new law will crack down on Medicaid fraud,” press release, May 16, 2006; available at http://www.governor.ks.gov/news/NewsRelease/nr-06-0516b.htm. Two states, New York and North Carolina, mandate that counties pay a significant share of Medicaid funds from their budgets. Hence, counties should have the power to investigate Medicaid billings of all providers and utilization of enrollees within their boundaries. They should, at the very least, have the authority to suspend providers and suppliers suspected of fraud. In cases where there is substantial evidence, counties should also have the authority to prosecute Medicaid fraud within their county. Since New York’s local governments pay one-fourth of the cost of Medicaid, the benefit to them of discovering and eliminating fraud is 25 cents on the dollar. If they were allowed to keep half of any funds recovered, they would have an incentive to double their efforts.
- John R. La Plante, “Are Medicaid Benefits Too Healthy?” Oklahoma Council of Public Affairs, June 1, 2003.
- Robert Pear, “U.S. Gives Florida a Sweeping Right to Curb Medicaid,” New York Times, October 20, 2005.
- Michael Bond, “Medicaid Pilot Takes Flight,” Journal of the James Madison Institute, Summer 2005, pages 8-10.
- Information obtained from “Governor Bush Signs Landmark Medicaid Reform Legislation,” EmpoweredCare.com, June 3, 2005. Accessed August 10, 2005.
- Michael Bond, “Reforming Medicaid in Kansas: A Market-Based Approach,” Flint Hills Center Public Policy, Policy Paper, Vol. 3, No. 3, February 2, 2006.
- For information about this program, see Gregory C. Pope et al., “Risk Adjustment of Medicare Capitation Payments Using the CMS-HCC Model,” Health Care Financing Review, Vol 25, No. 4, Summer 2004, pages 119-41.
- This is discussed in detail in John C. Goodman, “Characteristics of an Ideal Health Care System,” National Center for Policy Analysis, Policy Report No. 242, April 2001.
- Michael Bond, “Reforming Medicaid in Kansas: A Market-Based Approach.”
- “Reverse” health savings accounts differ from regular HSAs in that money or credit for services is deposited to the account as a reward after, not before, healthy behaviors occur.
- “Risk Pools: State Health Insurance High-Risk Pools,” Communicating for Agriculture and the Self-Employed. Available at http://www.selfemployedcountry.org/riskpools.html. Access verified February 2, 2006.
- A recent Milliman employer survey found that almost all (98 percent) employers are considering offering high-deductible health plans, whereas in 2003 less than half (48 percent) considered offering them. See “Healthcare Coverage: Insurance Company Launches New Health Plans and Health Savings Accounts,” Managed Care Weekly Digest, February 28, 2005.
- Emmett B. Keeler, “Effects of Cost Sharing on Use of Medical Services and Health.” RAND Corporation, 1992. Available at http://www.rand.org/pubs/reprints/RP1114/index.html. Access verified August 10, 2006. The study was based on 5,809 participants divided into four insurance plans: no cost-sharing, 25 percent, 50 percent and 95 percent coinsurance rates with an annual household maximum deductible of $1,000. Free care individuals tended to self-report more illness and worried more about illness than cost-sharing individuals.
- States contribute toward a deductible that is a 100% to 110% of the annual contribution to the health opportunity account (HOA). The maximum average annual contribution to an HOA is $2,500 for adults and $1,000 for children (indexed in future years). States may provide preventive care coverage without a deductible. Individuals may purchase services from Medicaid participating providers at the Medicaid rate, and from nonparticipating providers at 125% of the Medicaid rate. Three-fourths of the amount left in the HOA is available to the individual for 3 years. It may be used to purchase health insurance or (after participating one year) for additional expenditures (such as job training and tuition expenses) specified by the state and approved by the secretary of Health and Human Services. For a critical review, see Edwin Park and Judith Solomon, “Health Opportunity Accounts for Low-Income Medicaid Beneficiaries: A Risky Approach,” Center for Budget and Policy Priorities, November 1, 2005.
- Rep. Mike Rogers, “The Truth About Medicaid Reform: Puts America’s Most Vulnerable Families on Road to Self-Sufficiency,” letter, U.S. House of Representatives, November 7, 2005. Bill text available at: http://thomas.loc.gov.
- One limitation is that participants lose access to the funds once their income surpasses 200 percent of the federal poverty level.
- For a discussion on giving Medicaid enrollees choice, see Irene Fraser, Elizabeth Chait and Cindy Brach, “Promoting Choice: Lessons from Managed Medicaid,” Health Affairs, Vol. 17, No. 5, September/October 1998.
- A. E. Benjamin and Rani E. Snyder, “Consumer Choice in Long-Term Care,” in To Improve Health and Health Care, Volume V: The Robert Wood Johnson Anthology (Hoboken, New Jersey: Jossey-Bass, 2003) Chapter 5.
- The recently-passed Deficit Reduction Act of 2005 extends the “look back” period from three to five years. The waiting period to sign up for Medicaid after an asset transfer would be the amount of the money transferred divided by the annual cost of nursing home care in the state multiplied by 12 months. For example, under the previous law, if $20,000 was transferred less than three years prior in a state where a year of nursing home care costs $60,000, the waiting period before eligibility for coverage would be four months ($20,000/$60,000 = .333 years). However, the waiting period would officially begin not when the senior applied for Medicaid, but much earlier – four months after the actual date the funds were transferred. As a result, the four months waiting period might have lapsed a year or two earlier. Under the previous law, seniors could conceivably give away sufficient funds to cover up to two years or more worth of care without having to wait for Medicaid eligibility. Suppose a senior gave $20,000 to a granddaughter for college tuition four years prior to needing long-term care. Under the previous law, the $20,000 would not be included in assets when qualifying for Medicaid. However, the transfer would fall within the five year period resulting in a waiting period of four months. Under the DRA the waiting period begins not at date of transfer four years prior, but on the date of an individual starting institutional care.
- Kathryn G. Allen, “Medicaid: Transfers of Assets by Elderly Individuals to Obtain Long-Term Care Coverage,” U. S. Govern-ment Accountability Office, GAO-05-968, September 2005.
- See Ronald Lipman, “Trust Helps Person Qualify for Medicaid Nursing Care,” Houston Chronicle, August 11, 2002.
- Enid Kassner, “Medicaid and Long-Term Services and Supports for Older People Fact Sheet,” AARP Public Policy Institute, February 2005.
- For a pamphlet comparing the annual cost of home care and nursing home care across the country, see “Can You Afford the Cost of Long-Term Care?” U.S. Office of Personnel Management. Available at http://arc.publicdebt.treas.gov/files/pdf/fscombined.pdf. Access verified June 19, 2006.
- Ibid.
- See “Medicaid Long-Term Care: Successful State Efforts to Expand Home Services While Limiting Costs,” U.S. Government Accountability Office, Report No. 152298, August 1994.
- Ohio Commission to Reform Medicaid, “Transforming Ohio Medicaid: Improving Health Quality and Value,” State of Ohio, January 2005.
- “Summary of the Deficit Reduction Act of 2005 (Pl 109-171) Excerpt from the Jan-Feb. Issue of The ARC/UCP Disability Collaboration Washington Watch,” Association of University Centers on Disabilities, February 17, 2006. Available online at http://www.aucd.org/Medicaid/DRA_Summary.htm. Access verified June 8, 2006.
- For more information about reverse mortgages see the National Center for Home Equity Conversion at http://www.reverse.org. Access verified July 10, 2006.
- “Use Your Home to Stay at Home: Program Study Shows That Reverse Mortgages Can Help Many with Long-Term Care Expenses,” National Council on the Aging, Press Release and Fact Sheet, April 15, 2004.
- Stephen A. Moses, “How to Save Medicaid $20 Billion Per Year and Improve the Program in the Process,” Center for Long-Term Care Financing, 2005.
- A life settlement is similar to a viatical settlement but does not require terminal illness to qualify. Policy owners can sell a life insurance policy for an amount much higher than the cash surrender value. See “Viatical Settlements,” Centers for Medicare and Medicaid Services, March 31, 2005. Available at http://www.medicare.gov/LongTermCare/Static/ViaticalSettlements.asp?dest=NAV%7CPaying%7CPrivateInsurance%7CViaticalSettlements. Access verified January 25, 2006.
- “Viatical Settlements: A Guide for People with Terminal Illness,” U.S. Federal Trade Commission, May 1998. Available at http://library.findlaw.com/1998/May/1/126790.html. Access verified January 6, 2006.
- “Deficit Reduction Act of 2005: Implications for Medicaid,” Kaiser Commission on Medicaid and the Uninsured, February 2006. Available at http://www.kff.org/medicaid/upload/7465.pdf. Access verified June 19, 2006. The Act allows the states to raise the exemption to $750,000.
- John C. Goodman and Devon M. Herrick, “Reforming Medicaid: More Flexibility for the States,” National Center for Policy Analysis, Brief Analysis No. 515, May 13, 2005.
- This section is based on Matthew Pakula, “The Legal Responsibility of Adult Children to Care for Indigent Parents,” National Center for Policy Analysis, Brief Analysis No. 521, July 12, 2005.
- Jeanne M. Lambrew, “Making Medicaid a Block Grant Program: An Analysis of the Implications of Past Proposals,” Milbank Quarterly, Vol. 83, No. 1, January 26, 2005.
- Vernon K. Smith and Greg Moody, “Medicaid 2005: Principles and Proposals for Reform,” National Governors Association, February 2005.
- President Bush proposed a block grant that was budget-neutral for 2004. This would essentially lock into place each state’s 2004 payment for acute care.
- Jeanne M. Lambrew, “Making Medicaid a Block Grant Program: An Analysis of the Implications of Past Proposals.”
- “Budget Options 2005,” Congressional Budget Office, Section 550 Health, 550-08–Mandatory Convert Medicaid Disproportionate Share Hospital Payments into a Block Grant (Section 13 of 22), February 15, 2005.
- James C. Robinson, “Renewed Emphasis on Consumer Cost Sharing in Health Insurance Benefit Design,” Health Affairs, Web Exclusive, March 20, 2002. Available at http://content.healthaffairs.org/cgi/content/abstract/hlthaff.w2.139v1. See also Jason S. Lee and Laura Tollen, “How Low Can You Go? The Impact of Reduced Benefits and Increased Cost Sharing,” Health Affairs, Web Exclusive, June 19, 2002. Available at http://content.healthaffairs.org/cgi/content/abstract/hlthaff.w2.229v1. Access verified August 15, 2006.
- Utah received a waiver in 2002 that allowed it to increase cost-sharing through enrollment fees and copayments. Oregon received a waiver to impose nominal premiums of $6 to $20 per month. For a discussion see Marilyn Werber Serafini, “Balancing Act,” National Journal, August 13, 2005.
- “Deficit Reduction Act of 2005: Implications for Medicaid,” Kaiser Commission on Medicaid and the Uninsured, February 2006. Available http://www.aucd.org/medicaid/docs/kaiser_medicaid_uninsured.pdf; Access verified August 10, 2006.
- For a discussion on a health plan where cost-sharing varies by type of condition, see Shaun Matisonn, “Medical Savings Accounts and Prescription Drugs: Evidence from South Africa,” National Center for Policy Analysis, Policy Report No. 254, August 2002.
- A portion of this savings will also come from limiting prescription drug coverage and limiting physical therapy and speech therapy visits to 15 per year. “Kentucky, West Virginia First States to Revise Medicaid Programs Under New Federal Law,” Medical News Today, May 25, 2006.
- Devon M. Herrick, “How to Create a Competitive Insurance Market,” National Center for Policy Analysis, Brief Analysis No. 558, Thursday, June 15, 2006.
- “Medical and Dental Expenses,” IRS Publication 502, 2004. Available online at http://www.irs.gov/publications/p502/.
John C. Goodman is the founder and president of the National Center for Policy Analysis. The National Journal recently dubbed him the “Father of Health Savings Accounts,” and he has pioneered research in consumer-driven health care.
Dr. Goodman is the author/coauthor of eight books and more than 50 published studies on health care policy and other topics. He received a Doctor of Philosophy degree in economics from Columbia University. He has taught and done research at several colleges and universities including Columbia University, Stanford University, Dartmouth University, Southern Methodist University and the University of Dallas.
Michael Bond is Director of the Center for Health Care Policy at the Buckeye Institute and a professor in the Department of Finance at Cleveland State University. His work on Medical Savings Accounts (MSAs) and health-care policy reform has received national attention and appeared in a wide range of professional and popular publications, including Health Care Financial Management, Public Personnel Management, Compensation and Benefits Review, Benefits Quarterly and Business Horizons. He is the author of the nation’s first practical guide to establishing MSAs (published by the Buckeye Institute in 1997). He earned his Doctor of Philosophy degree and Master of Arts degree in economics from Case Western Reserve University.
Devon Herrick is a senior fellow with the National Center for Policy Analysis. He concentrates on such health care issues as Internet-based medicine, health insurance and the uninsured, and pharmaceutical drug issues. His research interests also include managed care, patient empowerment, medical privacy and technology-related issues.
Herrick received a Doctor of Philosophy degree in Political Economy and a Master of Public Affairs degree from the University of Texas at Dallas with a concentration in economic development. He also holds an Master of Business Administration degree with a concentration in finance from Oklahoma City University and an Master of Business Administration degree from Amber University, as well as a Bachelor of Science degree in Accounting from the University of Central Oklahoma.
Pamela Villarreal is a graduate student fellow at the National Center for Policy Analysis. She received a Bachelor of Science in Economics degree from the University of Texas at Dallas in 2003, and a Master of Science in Applied Economics degree in the summer of 2006. Ms. Villarreal has authored or coauthored a number of NCPA publications on such diverse topics as the estate tax, big-box retailers and aid for Hurricane Katrina evacuees.
She is currently pursuing a doctorate in public policy and political economy from the University of Texas at Dallas.